- LOGIN
- MemberShip
- 2026-05-01 13:10:16
- Policy
- Fitusiran for hemophilia receives orphan drug designation
- by Lee, Hye-Kyung May 09, 2025 06:01am
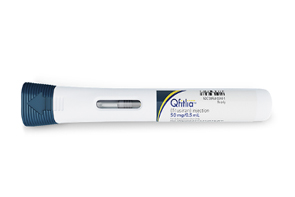
- Sanofi A long-acting treatment for all types of hemophilia, administered every 2 months, has been designated as an orphan drug in South Korea. According to the “Regulations on the Designation of Orphan Drugs” released by the Ministry of Food and Drug Safety on the 7th, Sanofi's Fitusiran was designated as the 386th orphan drug in Korea. Fitusiran was released under the brand name Qfitlia in the U.S.. In March, the U.S. FDA approved Fitusiran as the first antithrombin inhibitor-based therapy with the convenience of a twice-monthly subcutaneous injection, for the routine prophylaxis to prevent bleeding in patients aged 12 years and older with hemophilia A or B. Fitusiran is an siRNA (small interfering RNA) therapy designed to target antithrombin, a protein involved in blood clotting, for the treatment of patients with hemophilia A and B. It works by lowering antithrombin levels to promote thrombin production, thereby improving hemostasis and preventing bleeding in hemophilia patients. Currently, the hemophilia treatment market is dominated by Hemlibra for hemophilia A, while concizumab by Sanofi and Novo Nordisk is under development as a treatment for both hemophilia A and B. Regarding its designation as an orphan drug, according to the minutes of the Central Pharmaceutical Affairs Council meeting released by the MFDS on the 7th, there was an opinion that Fitusiran is a drug that can meet unmet needs and requires post-marketing surveillance. The committee members believe that Fitusiran is expected to provide patients with a better treatment option by addressing the limitations of current treatments in key areas such as ABR, joint bleeding, patient compliance, and the impact on quality of life. Additionally, while existing medications are currently available, if Fitusiran demonstrates superiority over existing products in terms of ensuring a smooth supply of medications for patients, reducing treatment costs, decreasing administration frequency, alleviating pain, and reducing bleeding, it was deemed to meet the criteria for having an unmet need. In particular, existing treatments have low convenience due to the burden of intravenous injections and frequent administration (2–3 times per week). However, Fitusiran, which is an intravenous injection usable for both hemophilia A and hemophilia B, has the advantage of subcutaneous injection every 4–8 weeks, offering improved convenience. However, while it appears to have improved safety and efficacy compared to alternatives, given its new pharmacological mechanism, careful review is necessary regarding data submission exemptions.. Although the structure of N-acetylgalactosamine and its pharmacologic mechanism when used as a target ligand in oligonucleotide and siRNA therapy are already well known, a detailed review of domestic clinical results would be necessary due to safety concerns identified in previous clinical trials. Therefore, regarding safety, the CPAC decided that the risk level could be judged as acceptable for approval by referencing overseas approval criteria, but appropriate patient monitoring would be necessary. The CPAC members stated that “Hemophilia is a disease with a clear pathophysiology and no significant differences in response between races. The submitted Phase III clinical trial results showed that Asian patients accounted for a relatively high proportion of participants, and submitted the opinion that domestic approval is reasonable. Meanwhile, it is reported that the annual cost of Fitusiran in the United States amounts to approximately USD 642,000 (approximately KRW 944 million).
- Policy
- Ofev reimbursed from May... inflow of generic versions
- by Lee, Hye-Kyung May 09, 2025 05:59am
- The generic drug market is growing for Boehringer Ingelheim's idiopathic pulmonary fibrosis treatment ‘Ofev Soft Capsules (nintedanib),’ which was granted reimbursement and was listed from this month, 8 years after approval. On the 7th, the Ministry of Food and Drug Safety approved 2 items, 100 mg and 150 mg of Whan In Pharm’s ‘Ofenip Tab (Nintedanib Esylate).’ Ofenip is the fourth generic version approved for Ofev, which was approved in 2016. Generic drug approvals began with Yungjin Pharmaceutical's ‘Nintebro Tab’ in December last year, followed by Daewoong Pharmaceutical's ‘Ofevia Tab and Ildong Pharmaceutical's ‘Cuninta Tab’. The Ofev generics have been granted marketing authorizations upon the original drug's patent expiration on January 25. Ofev, which contains nintedanib, has three indications: ▲treatment of idiopathic pulmonary fibrosis, ▲delaying the decline in lung function in patients with systemic sclerosis-associated interstitial lung disease, and ▲treatment of chronic fibrosing interstitial lung disease with progressive phenotype. However, the generic versions of Ofev do not have the indication for the treatment of idiopathic pulmonary fibrosis and have only been approved for the remaining two indications. The reason for this can be found in the reimbursement process for Ofev. According to the results of the reimbursement adequacy review conducted by the Drug Reimbursement Evaluation Committee of the Health Insurance Review and Assessment Service in January, Ofev was only granted reimbursement for two indications: systemic sclerosis-associated interstitial lung disease and chronic fibrosing interstitial lung disease with progressive phenotype. Although Ofev was initially approved for idiopathic pulmonary fibrosis, the pharmaceutical company did not submit separate cost-effectiveness data for the indication, so no discussion had been made regarding its reimbursement. In particular, in South Korea, Ildong Pharmaceutical’s ‘Pirespa Tab (Pirfenidone) had dominated the reimbursement market for idiopathic pulmonary fibrosis since 2015, so Boehringer Ingelheim, which owns Ofev, had no choice but to pursue a differentiation strategy. This is why latecomers following Ofev that are attempting reimbursement have also entered the market with indications that are being reimbursed for the original drug. Currently, the number of patients eligible for Ofev’s use with reimbursement in Korea is estimated to be about 329. With reimbursement, patients will see a significant reduction in their annual medication costs from KRW 19.14 million to KRW 5.74 million. In addition to the pharmaceutical companies that have already received approval, domestic companies such as Chong Kun Dang, Sama Pharm, and Samoh Pharm are also developing generic versions of Ofev, so more generics are expected to be released in the future.
- Policy
- Drug-switching to AZ Ultomiris increases with aHUS reimb
- by Lee, Tak-Sun May 07, 2025 06:02am
- Product photo of Soliris and Ultomiris Drug switching for atypical Hemolytic Uremic Syndrome (aHUS) has become common practice. As 'Ultomiris (ravulizumab)' becomes reimbursed as of January in addition to previously reimbursed 'Soliris (eculizumab),' patients on Soliris are switching to Ultomiris. Two drugs are pre-reviewed medications distributed by AstraZeneca. According to industry sources on the 30th, the Health Insurance Review & Assessment Service (HIRA)'s Medical Practice Assessment Division has recently disclosed that the number of pre-reviewed cases between February and March was 15. Ten of these cases were submitted by Ultomiris for pre-review assessment. Nine of the ten Ultomiris cases were approved, while one was not. Two Soliris cases are related to the termination of administration. Two were approved, while one was not. aHUS is a rare disease in which chronically uncontrolled complement activity leads to thrombotic microangiopathy (TMA), causing persistent damage by thrombosis and inflammation to the small blood vessels throughout the body. It is known that approximately 79% of patients die or require dialysis within three years of onset and suffer permanent renal damage. The only treatment, Soliris, has been reimbursed by national health insurance since July 2018. However, because it is an expensive drug, reimbursement decisions are made through pre-review authorization as part of benefit management. The problem is that the approval rate for pre-review authorization is as low as 30–40%, prompting calls to either ease the pre-review authorization requirements or switch to follow-up review to improve patient access. Meanwhile, Ultomiris, an upgraded alternative to Soliris, has been reimbursed for aHUS since January of this year. Ultomiris is a next-generation C5 complement inhibitor with a half-life approximately four times longer than Soliris. In contrast, Soliris must be administered every two weeks, while Ultomiris extends the dosing interval to eight weeks, thereby improving convenience. As administration convenience has dramatically improved, patients on Soliris are now switching to Ultomiris. All ten cases disclosed were drug-switching administrations. In nine approved cases, Soliris had been administered in three cases in 2024, two cases in 2023, two cases in 2022, one case in 2021, and one case in 2018, and applications for coverage as Ultomiris drug-switching met the criteria and were approved. In a case where Soliris was not approved in 2022, the review committee concluded that treatment discontinuation was necessary due to symptom improvement, leading to non-approval. Drug-switching from Soliris to Ultomiris is expected to increase further. When setting the reimbursement criteria for Ultomiris, the Ministry of Health and Welfare also clarified the criteria for drug-switching. It specified that patients currently on Soliris who switch to Ultomiris must meet the maintenance criteria under the Ultomiris coverage guidelines and not meet any discontinuation criteria. MOHW also announced that the starting point for monitoring treatment efficacy and calculating the treatment period would be when Soliris was administered. However, whether reimbursing Ultomiris will raise the pre-review authorization approval rate for aHUS patients is still uncertain. This is because non-approval cases continue to occur among new patients. An industry professional said, "Since last November, pre-review authorizations for Soliris and Ultomiris in PNH have been converted to standard reviews, but for patient care, pre-review authorization should also be abolished for aHUS."
- Policy
- Increasing requests for BESREMi reimbursement
- by Whang, byung-woo May 07, 2025 06:02am
- Whether the polycythemia vera (PV) treatment BESREMi (ropeginterferon alfa-2b) will be considered for the Drug Reimbursement Evaluation Committee (DREC) review gains attention. Product photo of BESREMiAccording to the pharmaceutical industry sources, the 5th DREC of the Health Insurance Review & Assessment Service (HIRA) is scheduled to convene on the 8th. BESREMi is a next-generation interferon that targets the JAK2 mutation gene, which causes polycythemia vera. It was developed with improved purity and tolerability over existing interferons so that it can be administered every two weeks for the first 1.5 years and then every four weeks thereafter. However, despite having its reimbursement criteria set by the Cancer Drug Reimbursement Committee in March of last year, BESREMi has not yet been submitted to the Drug Reimbursement Evaluation Committee (DREC) even after 14 months, and it remains unclear whether it will be on the agenda for the upcoming 5th committee meeting. On May 2, the Korea Leukemia Patients Association called for a discussion of BESREMi's reimbursement to provide a treatment option for polycythemia vera patients with no alternatives. The Association explained, "The only treatment currently reimbursed by national health insurance is hydroxyurea. However, approximately 10–20% of all patients are either refractory or cannot continue to take the drug due to side effects. For these patients, BESREMi is virtually the only treatment alternative." As of 2023, there are 4,995 polycythemia vera patients in South Korea, who are classified into low- and high-risk groups. Professor Seong-Yun Lee of the Division of Hematology-Oncology at Ilsan Paik Hospital remarked, "Although polycythemia vera may seem small in patient pool as a rare haematologic malignancy, the patient population continues to grow. Over time, low-risk patients transition to the high-risk category, increasing the likelihood of resistance or intolerance, so the scale should not be underestimated." Notably, during the parliamentary petition in February last year to urge BESREMi's reimbursement, the initiative collected 50,552 signatures in just 30 days, demonstrating broad social consensus on the need for treatment, and the Association insists that the system and administration must respond swiftly. The Association stated, "The fact that BESREMi has not been submitted to the DREC even 14 months after the Cancer Drug Reimbursement Committee's decision reflects that the government and the pharmaceutical company are ignoring the desperate reality of patients without treatment options," and demanded, "BESREMi must be placed on the committee's agenda, approved, and quick price negotiations must follow." Nevertheless, there is reason to hope that BESREMi will be on the 5th DREC's agenda, as the HIRA's Economic Evaluation Committee has already confirmed its cost-effectiveness. The next steps will proceed based on whether the company accepts the government's proposal, and industry sources say that PharmaEssentia Korea, which has BESREMi, has agreed to the proposal after persuading its global headquarters. Although further discussions remain, some predict that BESREMi's bid for reimbursement will advance rapidly now that some compromises have been reached. The key will be the specific price-setting since, with global interferon shortages continuing and more cases of BESREMi adoption emerging, the price set in Korea may serve as a reference. It is also anticipated that PharmaEssentia Korea may propose a risk-sharing agreement (RSA) during negotiations, meaning that even after DREC approval, negotiations with the HIRA on pricing will remain a challenge for the company. Professor Lee said, "It would be ideal for all patients to receive treatment without financial burden, but considering the limits of national health insurance finances, priority reimbursement for patients who are resistant or intolerant to hydroxyurea is urgently needed. These patients have no other treatment options if they cannot be treated with hydroxyurea."
- Policy
- Reimb for ovarian cancer treatment lacks full coverage
- by Whang, byung-woo May 02, 2025 05:56am
- Despite expanded reimbursement for homologous recombinant deficiency (HRD)-positive ovarian cancer, HRD-related tests remain non-reimbursed. The Korean medical community has taken the initiative to resolve this issue. Sources reported that the Korean Society of Gynecologic Oncology is collecting evidence to propose reimbursing the HRD tests to the Ministry of Health and Welfare (MOHW). HRD is the loss of homologous recombination repair, which is one of the DNA repair processes. When a patient tests positive for HRD, cancer cells are unable to repair DNA damage effectively. In particular, mutations in BRCA1/2 genes, commonly occurring in breast cancer and ovarian cancer, cause HRD. The HRD prevalence in ovarian cancer is clinically reported to be about 50%. The Korean Society of Gynecologic Oncology focuses on the HRD tests because of expanded reimbursement for the ovarian cancer treatment Zejula. The National Health Insurance reimbursement criteria for Zejula expanded since October last year to the treatment of HRD-positive ovarian cancer. Previously, reimbursement of Zejula was approved for patients with BRCA mutations-associated ovarian cancer who responded to platinum-based therapy in first-line treatment. Due to expanded reimbursement, Zejula is now the only PARP (Poly ADP-ribose Polymerase) inhibitor with insurance coverage for first-line maintenance therapy in HRD-positive ovarian cancer patients. Product photo of ZejulaAbout seven months after the reimbursement expansion, prescriptions for Zejula have continued to increase. Ovarian cancer patients take two 100 mg tablets once daily, and among conventional ovarian cancer treatments, Zejula is the only one with a once-daily dosing regimen. In particular, since long-term PFS extension benefits have been confirmed in the PRIMA trial and follow-up observational studies, increased prescriptions following reimbursement expansion were expected. The issue lies in the HRD-positive status that is central to the reimbursement expansion. Since the reimbursement criteria are for HRD-positive ovarian cancer treatment, confirming HRD positivity is essential. However, unlike Zejula being reimbursed, the HRD tests remain non-reimbursed. The HRD test requires a next-generation sequencing (NGS)-based gene panel assay, for which the patient must bear approximately KRW 2.5 million in costs. In contrast, BRCA1/2 mutation testing has relatively greater accessibility through national programs and partial health insurance coverage, creating a gap between the two tests. In other words, patients seeking a reimbursed prescription for Zejula must pay out-of-pocket for an expensive and non-reimbursed test. The Korean Society of Gynecologic Oncology has also recognized this issue and plans to propose a policy measure to address it. A society official stated, "From a patient's perspective, it is difficult to understand that a non-reimbursed test is required in order to prescribe a reimbursed drug," and added, "We are planning to review Korea's testing infrastructure and foreign precedents and convey related opinions to the MOHW." The society's proposal on HRD testing is scheduled to be submitted to the MOHW and the Health Insurance Review & Assessment Service (HIRA) as early as the first half of the year. However, whether they will lead to substantive discussions on formal reimbursement remains to be seen. Considering that the prevalence of HRD in ovarian cancer reaches about 50% and that most patients require testing before treatment, the real-world issue of financial burden persists. A Korean Society of Gynecologic Oncology representative added, "To improve treatment outcomes for ovarian cancer patients, the introduction and utilization of HRD testing are necessary. Therefore, institutional support will be necessary."
- Policy
- Ofev will be reimbursed next month
- by Lee, Tak-Sun Apr 29, 2025 05:57am
- Product photo of Ofev Ofev Soft Cap (nintedanib esylate, Boehringer Ingelheim Korea) , which was approved in South Korea in 2016, will be listed for reimbursement next month, creating an opportunity for follow-on drugs. It took a long time to secure reimbursement, and with its compound patent already expired, generic manufacturers have obtained marketing authorization and are now awaiting reimbursement. Generic manufacturers plan to apply for reimbursement immediately upon Ofev’s listing to receive the same reimbursement price and commence market sales soon. Some generic companies are even securing distribution channels by launching non-reimbursed versions before the reimbursement takes effect. According to industry sources on the 28th, Ofev soft cap will be reimbursed from next month at KRW 26,220 for the 150 mg and KRW 20,960 for 100 mg. After Ofev was approved in South Korea in October 2016, the drug applied for reimbursement in October 2020 but was deemed non-reimbursable, and the company re-applied for reimbursement in March of last year. Ofev has secured three indications. At the time of its domestic approval in October 2016, it was indicated for idiopathic pulmonary fibrosis (IPF), in February 2020, for systemic sclerosis-associated ILD, and in June 2020, for chronic fibrosing ILD with a progressive phenotype (PPF). The current reimbursement criteria cover only ILD with a PPF. The Health Insurance Review & Assessment Service (HIRA) determined that reimbursement for IPF was not appropriate, as the company did not submit separate cost-effectiveness evidence. In the case of IPF, Ildong Pharmaceutical's Pirespa Tab (pirfenidone) established a dominant position when they were reimbursed under a risk-sharing agreement (RSA) starting in October 2015. Subsequently, generic pirfenidone formulations entered the market, and Pirespa Tab's RSA ended in October 2017. Currently, pirfenidone formulations from Ildong Pharmaceutical, Yungjin Pharmaceutical, Kolon Pharma, and Korea United Pharm are listed for reimbursement. When Pirespa entered the RSA, it was difficult for follow-on products in the same indication to be included in the scheme, making reimbursement listing for Ofev challenging. After securing Ofev's three indications in 2020, the company was reportedly focused on obtaining reimbursement for PPF, a segment with no market competition. The Drug Reimbursement Evaluation Committee (DREC) recognized clinical utility, citing the significant improvement in the annual decline rate of forced vital capacity (FVC) compared with placebo and judging that the cost-effectiveness ratio fell within an acceptable range, deeming reimbursement appropriate. Reimbursement also includes patients with systemic sclerosis-associated interstitial lung disease who exhibited delayed lung function decline. It is estimated that approximately 329 patients will be eligible for Ofev reimbursement in Korea. With reimbursement, annual out-of-pocket drug costs are expected to amount to KRW 5.74 million, significantly reducing the financial burden. Under non-reimbursed status, costs amounted to approximately KRW 19.14 million. However, the imminent entry of generic versions poses a threat to Ofev. Ofev's compound patent expired on January 25 of this year. As a result, generic manufacturers have either already launched their products or are preparing to do so following approval. The currently approved generics are Daewoong Pharmaceutical's Opevia Tab, Yungjin Pharm's Nintebro Tab, and Ildong's Cuinnta Tab. With Ofev being listed as an innovator drug, these generics are now more likely to receive reimbursement within three months of their listing applications. If they apply for reimbursement in May, they could be covered as early as August. The fact that the compound patent has expired and that nintedanib is designated as an orphan drug allows it to receive the same top reimbursement price as the original, creating opportunities for the generics. In particular, companies that have already established a foothold in the pulmonary fibrosis market with pirfenidone formulations can expect synergies by maintaining their existing customer base while expanding their product line. Pirfenidone and nintedanib have different reimbursed indications. Last year, pirfenidone formulations posted sales of KRW 34 billion for Ildong's Pirespa (according to UBIST) and KRW 4.9 billion for Yungjin's Fybro. Yungjin began marketing immediately after the patent expired, while Ildong recently started non-reimbursed marketing. Ildong held a symposium on the launch of Cuinnta Tab on the 26th–27th at the Gravity Chosun Seoul Pangyo Hotel, attended by approximately 80 respiratory medicine specialists from across the country.
- Policy
- 13 items including Jakavi receive price cuts in May
- by Lee, Tak-Sun Apr 29, 2025 05:56am
- Starting May 1, the insurance price ceiling of 13 items on the drug reimbursement list will be reduced. Among them, five items are voluntary reductions requested by the manufacturers. According to industry sources on the 28th, the insurance ceiling prices of 13 items will be reduced in May, including the price of Jakavi Tab, which will be lowered based on the Price-Volume Agreement. Jakavi Tab (ruxolitinib phosphate, Novartis), a treatment for myelofibrosis, will have its price reduced under Type B Price-Volume Agreement negotiations. Type B negotiations are conducted if the maximum price was previously adjusted under Type A negotiations, or if the claims amount for the same product group has increased by more than 60% compared to the previous year's claims amount without Type A negotiations, or the increase is 10% or more and the increase amount exceeds KRW 50 billion. In such cases, the price is adjusted through price negotiations with the National Health Insurance Service. Accordingly, the price of Jakavi 5mg tablets will be reduced from KRW 25,962 to KRW 25,339, Jakavi 10mg tablets from KRW 38,943 to KRW 38,398, Jakavi 15mg tablets from KRW 52,199 to KRW 59,460, and Jakavi 20 mg tablets will be reduced from KRW 52,213 to KRW 50,960. Lorviqua, reimbursement for which has been expanded to cover the reimbursement of first-line treatment for anaplastic lymphoma kinase (ALK)-positive locally advanced or metastatic non-small cell lung cancer, underwent a procedure to adjust the maximum price in accordance with the expansion of the scope of use of risk-sharing agreement drugs. As a result, the price of Lorviqua Tab 25mg will be reduced from KRW 52,819 to KRW 51,234, and the price of Lorviqua Tab 100mg will be reduced from KRW 158,457 to KRW 153,703. Two migraine treatment drugs that contain naratriptan, will have their prices reduced due to the expiration of the pricing premium. This is because there are now four or more Naratan ODT 2.5mg products available. The health authorities terminate the premium pricing immediately when the number of companies with the same formulation registered after the expiration of the premium pricing period (one year) reaches four or more. As a result, the price of CMG Pharm’s Narafil ODF 2. 2.5mg will be reduced from KRW 2,437 to KRW 2,193, and Yuyu Pharmaceutical's Nagran ODT 2.5mg will be reduced from KRW 2,867 to KRW 2,193. These products were previously granted first-generic exclusivity last month, but the premium was terminated within a month due to the introduction of same-ingredient products. A total of 5 products will have their price ceiling reduced following voluntary price reduction requests from manufacturers. These include 3 products from Daewoong Bio (Serotapin Tab), one from Bukwang Pharm (Ariplus Tab), and one from Hyundai Pharm (DM Duo Tab). The price of Serotapin Tab 25mg will be reduced from KRW 274 to KRW 230, Serotapin Tab 100mg from KRW 688 to KRW 544, and Serotapin Tab 200mg from KRW 1,012 to KRW 927. The price of Ariplus Tab will be adjusted from KRW 3,879 to KRW 2,990, and DM Duo Tab will be adjusted from KRW 3,879 to KRW 3,658. Ariplus and DM Duo are donepezil + memantine combination drugs that were listed for reimbursement in March. Bukwang and Hyundai voluntarily lowered their drug prices just two months after their release.
- Policy
- Will Enhertu be reimb for HER2-low cancer in Korea?
- by Whang, byung-woo Apr 28, 2025 05:55am
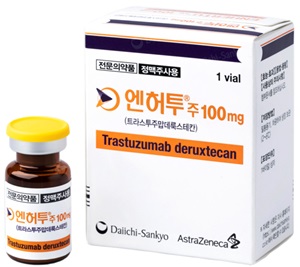
- Results of the deliberation on the reimbursement expansion of the new antibody-drug conjugate (ADC) Enhertu (trastuzumab deruxtecan) for HER2-low breast cancer and lung cancer are drawing attention. Pic of Enhertu According to industry sources, the Health Insurance Review and Assessment Service's Cancer Disease Deliberation Committee (CDDC) is scheduled to hold a meeting on the 30th to review 2 additional indications for Enhertu. The indications under review are ▲HER2-low metastatic breast cancer and ▲HER2-mutated non-small cell lung cancer (NSCLC). If the reimbursement expansion is approved, this is expected to expand treatment access for breast cancer and lung cancer in Korea. Both indications were approved by the Ministry of Food and Drug Safety in May last year based on the DESTINY-Breast04 and DESTINY-Lung02 clinical studies. Notably, the trials demonstrated the efficacy of Enhertu in HER2-low breast cancer, where treatment options were previously for HER2-negative status patients, and marks the emergence of the first and only targeted therapy for HER2-mutated lung cancer. Additionally, Enhertu has expanded its indication to include HER2 ultra-low expression in the United States by the FDA, suggesting its potential as a new standard treatment option for patients with metastatic breast cancer across the entire spectrum of HER2 expression, including HER2-positive, HER2-low, and HER2 ultra-low expression breast cancer. The main point of the CDDC review was also focused on how to evaluate Enhertu's efficacy in HER2-low expression breast cancer, where existing HER2-targeted therapies have shown limited efficacy, despite the significant improvement in treatment outcomes for HER2-positive breast cancer achieved by existing HER2-targeted therapies. Previously, HER2-positive breast cancer was defined as “HER2-positive if IHC 3+ or IHC 2+ and ISH-positive, and HER2-negative if IHC 0, IHC 1+, or IHC 2+ and ISH-negative.” Joohyuk Sohn. Professor of Medical Oncology at Yonsei Cancer Center, said, “With the domestic approval of Enhertu's indication for HER2-low metastatic breast cancer, patients previously classified as HER2-negative with limited treatment options now have a new treatment option. This is expected to further improve the treatment landscape for HER2-positive metastatic breast cancer in Korea.” Enhertu is the first anti-HER2 agent to demonstrate treatment benefits in HER2-low metastatic breast cancer, redefining the definition of HER2-low and presenting a new paradigm for metastatic breast cancer treatment. Another key point is that patients with HER2-low breast cancer account for nearly half - approximately 45% to 55% - of all breast cancer patients. Additionally, HER2-low breast cancer accounts for approximately 60% of HER2-negative breast cancer cases. Apart from the benefits of Enhertu, this means that the financial burden on health insurance due to the large number of patients would also likely need to be taken into consideration to a certain extent. If reimbursement is expanded to include indications such as HER2-low breast cancer and HER2-mutated non-small cell lung cancer, this is expected to increase Enhertu’s insurance claims amount significantly. This is why there are industry views that the reimbursement expansion will depend on the financial sharing plan proposed by the pharmaceutical company. However, when Enhertu was listed for reimbursement in Korea last April as a treatment for HER2-positive metastatic breast cancer and gastric cancer, the government had flexibly applied the ICER threshold to grant its reimbursement. In March, Daiichi Sankyo reportedly applied for and held a drug briefing session on Enhertu’s use in HER2-mutated non-small cell lung cancer. Drug information briefing sessions were introduced in 2010 to enhance the transparency and objectivity of evaluations by facilitating mutual sharing of information between pharmaceutical companies and reviewers regarding new drugs. Daiichi Sankyo also utilized this system during the initial approval of Enhertu. Enhertu was jointly developed and commercialized by Daiichi Sankyo and AstraZeneca. In South Korea, it is co-developed and promoted by Daiichi Sankyo Korea and AstraZeneca Korea, with distribution handled by Daiichi Sankyo Korea.
- Policy
- 'Social discussions needed for indication-based pricing'
- by Lee, Jeong-Hwan Apr 28, 2025 05:54am
- Won-Joon Cho, head of the Democratic Party There have been calls for caution regarding the introduction of an “indication-based drug pricing system,” to improve patient access to multi-target anticancer drugs that treat various types of cancer. The concern is that if the insurance drug price for a specific disease among the multiple indications of an anticancer drug increases, the insurance drug price for other diseases may decrease, thereby hindering patient access. Suggestions were also made that it is necessary to discuss whether the introduction of an indication-based drug pricing system is a good alternative, whether expanding the risk-sharing agreement (RSA) is a more realistic option in the short term, or whether other policy approaches are needed, and to go through a process of reaching social consensus. On the 25th, Won-Joon Cho, senior expert on health and welfare policy and head of the Democratic Party's presidential election pledge task force, made the following statement regarding the indication-based drug price system. Recently, a debate on “Eliminating inequality in access to innovative new drugs and improving regulations” was held at the National Assembly, hosted by Democratic Party lawmakers Mi-hwa Seo, Yoon Kim, and Jong-tae Jang and organized by the Korean Research-based Pharmaceutical Industry Association (KRPIA). At the debate, there was a wide argument on how the current single drug pricing system in Korea is limiting patients' access to high-cost anticancer drugs like Keytruda and Opdivo, despite their approval for various indications, and that an indication-based drug pricing system should be introduced to address this issue. Won-Joon Cho noted how certain lung cancer treatments have over 30 indications and that he understands why an indication-based drug pricing system is being proposed. However, he pointed out that it is important to consider the paradoxical issue that raising the price of the drug for a specific indication could reduce patient access to the drug itself or lower the likelihood of its health insurance reimbursement listing. Cho explained, “If the price for a specific indication becomes excessively high, it could paradoxically reduce patients' access to medications or lower the likelihood of insurance coverage. Theoretically, while drug prices may decrease for some indications, others will inevitably increase.” He added, “On a practical level, there are concerns about whether the Health Insurance Review & Assessment Service (HIRA) will be able to track and manage (drug price claims, etc.) for each indication and whether errors in entering indications and false claims can be controlled. The drug price negotiation process is also likely to become complicated and opaque.” Cho explained that this is why it is necessary to carefully examine whether introducing a system that differentiates drug prices by indication is the best alternative whether there are other policy alternatives, and the need to secure empirical evidence. He stated, “At this point, we need to discuss whether a differential drug pricing system based on indications is a significantly better alternative than the current drug pricing system, whether expanding the RSA is a more realistic alternative for now, or whether a different approach is necessary. Any discussion of institutional changes must be preceded by verification and evaluation, and there must be sufficient empirical evidence based on case studies.”
- Policy
- ‘Should apply blended pricing and reimbursement rates’
- by Lee, Jeong-Hwan Apr 25, 2025 05:59am
- With multiple drugs with multiple indications, such as multi-targeted immunotherapy drugs, being approved in Korea, there have been claims that the introduction of an “indication-based drug pricing system” is necessary to improve patient access to treatment and ensure equity. In particular, the argument was made that ‘blended pricing,’ which sets different prices for each indication, could reflect the value of each indication while maintaining a single price, thereby increasing social acceptability, and that it could be introduced without conflicting with the current drug pricing system in Korea, which is based on a single price structure. Ultimately, after taking the first step with “blended pricing,” the industry recommended that the government should introduce a “differentiated reimbursement rate system” based on real-world data accumulated for each indication in order to reflect the value of drugs for each disease and speed up reimbursement for patients. Jung-hoon Ahn, Professor of Health Convergence at Ewha Womans University Graduate School, will present these views at a policy discussion forum titled “Resolving Inequality in Innovative New Drugs and Regulatory Reform” co-hosted by the Democratic Party of Korea lawmakers Mihwa Seo, Byung-Hoon So, Yoon Kim, and Jong-Tae Jang on the 24th. The forum is organized by the Korean Research-based Pharmaceutical Industry Association (KRPIA). Professor Ahn will give a presentation on the reimbursement policy for drugs with multiple indications. Professor Ahn pointed out that there are an increasing number of cases in which drugs with multiple indications are being approved in the field of anticancer drugs. In fact, as of 2018, 75% of tumor treatment drugs in the United States were approved as drugs with multiple indications, and in South Korea, 32 anticancer drugs with multiple indications are eligible for reimbursement. In South Korea, drug prices are determined based on the active pharmaceutical ingredient contained in the drug, making it difficult to set and reflect separate prices for individual indications. This means that even drugs with multiple indications are assigned a single insurance reimbursement ceiling. Professor Ahn expressed concerns that the value of individual indications is not sufficiently reflected in drug prices, leading to issues such as access to treatment for patients that are covered with the expanded indications in South Korea. Taking the multi-indication immunotherapy drug Keytruda as an example, he pointed out that while it is reimbursed in Italy, Switzerland, France, Australia, Japan, and Belgium for both first-line treatment of head and neck squamous cell carcinoma and second-line treatment of endometrial cancer, it is not reimbursed for either in South Korea. In response, Professor Ahn suggested the need to introduce or improve a drug pricing system for multi-indication drugs. Specifically, Professor Ahn proposed that while methods such as “individual approval for each indication” or “differentiated reimbursement rates” could transparently reflect the value of each indication, they require legal amendments or raise concerns about equity in reimbursement amounts between patients that are applied different indications, as well as the need for preparation in the current system, including settlement mechanisms. He emphasized that the blended pricing method is highly feasible under the current reimbursement and drug price system. The logic is that applying blended pricing within the framework of risk-sharing agreements (RSAs), which are legal contracts, would allow the value of drugs to be reflected according to their indications while managing the financial risk of drugs with uncertain cost-effectiveness. Professor Ahn stated, “The country has established a value-based drug pricing system. However, while value is recognized primarily based on the primary indication, appropriate values for individual indications are not reflected. As a result, pharmaceutical companies are delaying or abandoning the launch of subsequent indications, leading to reduced access to new treatments for patients.” “I propose collecting and analyzing real-world data on claims made for each indication to establish actual value evidence for drugs, and building a system that applies differential reimbursement rates that reflect the clinical value differences by indication based on accumulated data,” said Ahn. “This is a strategic approach that complements the limitations of Korea's single drug pricing system while flexibly realizing the effects of indication-based drug price adjustments.” He added, “We can start with a practical approach, such as blended pricing (indication-weighted average price), and gradually evolve toward a differentiated reimbursement rate system that reflects indication-specific value. Blended pricing maintains a single price while reflecting the value of individual indications, making it more acceptable within the social framework.”