- LOGIN
- MemberShip
- 2026-05-02 11:39:33
- Policy
- Samil voluntarily cuts price of its Vemlino to lowest price
- by Lee, Tak-Sun Nov 19, 2024 06:13am
- Samil Pharm is voluntarily reducing the price of its hepatitis B drug Vemlino (Tenofovir Alafenamide Hemimalate). This will render the drug to be the lowest-priced drug among tenofovir alafenamide drugs, increasing its price competitiveness. According to industry sources on the 18th, the price of Vemlino will be reduced from KRW 2,425 to KRW 2,358 starting next month. There are currently 9 tenofovir alafenamide-based hepatitis B treatments, including the original Vemlidy (tenofovir alafenamide hemifumarate, Gilead). The other 8 are salt-modified agents. Vemlidy is an upgraded version of Gilead's Viread. Viread was associated with side effects of decreased kidney function or bone density in some patients, so the upgraded Vemlidy has become the most commonly recommended initial treatment on site as it contains one-tenth the active ingredient dose of Viread while providing the same level of viral suppression. The salt-modified versions of Vemlidy have been sequentially released to the market starting with Dong-A ST’s ‘Vemlia Tab (tenofovir alafenamide citrate). The companies were able to enter the market by avoiding patents through salt modification. However, even with the introduction of such versions, the original's status remained unchanged. Vemlidy’s sales continued to soar, reaching KRW 27.9 billion in 2021, KRW 39.3 billion in 2022, and KRW 49.2 billion in 2023, according to UBIST. This is the third consecutive year that the drug’s upper limit has been reduced through the price-volume agreement negotiations due to increased usage. The price of Vemlino, whose price was lowered this time, was only KRW 300 million (UBIST) last year. Samil had listed its drug at KTW 2,425, lower than the calculated amount when it was listed in July last year, to gain price competitiveness. However, the lowest price title went to Dongkook Pharmaceutical’s Alfoterin Tab (Tenofovir Alafenamide Hemimalate). The upper limit for Alfoterin is KRW 2,424. This time, Samil lowered the price of Vemlino to KRW 2,328 and took over the lowest price title. The highest price for tenofovir alafenamide is currently KRW 3,235 for the original Vemlidy Tab, and the difference between Vemlidy and Vemlino is KRW 887. HBV patients are sensitive to the price because they need to take medications for life. Therefore, it will be interesting to see if Vemlino can gain market share with its competitive price. An industry insider said, “The market for tenofovir alafenamide preparations has only 8 generic contestants that entered the market through patent evasions, so there is less competition and the companies can take more of the market share. However, the generic companies are struggling due to high dependence on the original, and the eyes are on whether the low-price competition can break this pattern.”
- Policy
- HK Inno.N to distribute Tamiflu as Roche’s new partner
- by Lee, Tak-Sun Nov 18, 2024 05:49am
- HK Inno.N will be responsible for the domestic distribution of ‘Tamiflu Cap’ in addition to the distribution of the antiviral drug ‘Xofluza.’ The company is expected to gain external growth with the distribution of Tamiflu, which has an annual sales volume of KRW 15 billion. According to industry sources on the 15th, HK Inno.N sent a letter to its business partners and announced that it will distribute Roche Korea’s Tamiflu Cap. 30/45/75mg from the 14th. Tamiflu is “the” antiviral flu drug. Its sales were sluggish in 2020 and 2021 during the height of the COVID-19 pandemic, but have risen significantly since last year with the rise of the flu epidemic. Last year, its outpatient prescriptions amounted to KRW 15 billion based on UBIST. Its previous distributor, Chong Kun Dang had distributed Tamiflu in Korea since 2012, but the companies’ partnership ended last year and Roche has been seeking a new domestic partner since. Last year, HK Inno.N signed an exclusive domestic distribution and commercialization agreement with Roche Korea for the antiviral flu drug Xofluza (baloxavir marboxil). Under the agreement, HK Inno.N will distribute Xofluza for 2 years and jointly conduct marketing and sales activities with Roche Korea. Xofluza is a new drug that can treat influenza with just one dose, unlike other oral influenza treatments that require 5 days of administration. It is the first flu antiviral drug to be developed in 20 years. However, Xofluza is still non-reimbursed in Korea, so it has not been able to raise significant domestic sales. If it succeeds in being reimbursed in Korea, it is expected to take over Tamiflu's sales. Roche had shown its trust in HK Inno.N, signing for Tamiflu following Xofluza. HK Inno.N is expected to become Roche's new partner in Korea after Chong Kun Dang. “HK Inno.N has recently emerged as a key player in the domestic respiratory virus drug market, supplying Pfizer's new COVID-19 vaccine,” said a pharmaceutical industry insider. ”Its distribution of Tamiflu will help accelerate the company's external growth and raise company awareness in the antiviral drug market.”
- Policy
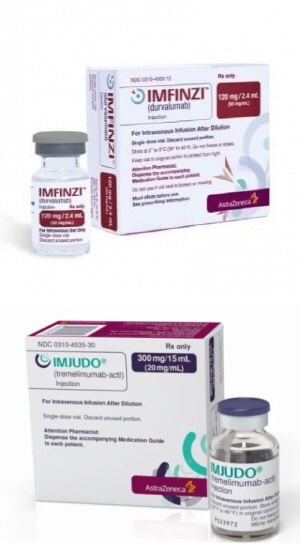
- AZ’s Imjudo and Imfinzi both make reimbursement progress
- by Lee, Tak-Sun Nov 15, 2024 05:49am
- AstraZeneca (AZ) Korea’s ‘Imjudo Inj.’ Has passed the first step to reimbursement listing in Korea. Also, reimbursement standards for ‘Imfinzi Inj,’ which is seeking reimbursement expansions, were set. However, these are only the first steps to reimbursement. On the 13th, the Health Insurance Review and Assessment Service held the 8th Cancer Disease Review Committee in 2024 to deliberate on the reimbursement standards for anticancer drugs. As a result of the deliberation, reimbursement standards were set for the new drug Imjudo Inj (tremelimumab) but not for Tecvayli Inj (teclistamab, Janssen). Imjudo is indicated for the first-line treatment of adult patients with advanced or unresectable HCC in combination with durvalumab. Here, durvalumab is AZ's immuno-oncology drug Imfinzi. Imfinzi is indicated for the treatment of patients with unresectable locally advanced non-small cell lung cancer (NSCLC) whose disease has not progressed after platinum-based concurrent chemoradiotherapy (CCRT). However, based on clinical results, the company has been seeking to expand its coverage to include liver and biliary tract cancers. One such example is the Imfinzi-Imjudo combination as a first-line treatment for liver cancer. Another is biliary tract cancer. Since February, Imfinzi+gemcitabine+cisplatin has been used for the first-line treatment of patients with locally advanced or metastatic biliary tract cancer. However, Imfinzi is currently paid fully out-of-pocket. As Imfinzi is an expensive drug, costing KRW 3,347,202 per bottle, healthcare professionals as well as patients have been requesting Imfinzi be covered by the government. The patients' voices were also discussed as an agenda at the last national audit. In response, HIRA had promised a proper review. On this day, their efforts bore fruit. Reimbursement standards were finally set for the drugs. With both drugs being set reimbursement standards, AZ can now look forward to the prompt reimbursement of both of its drugs. However, another AZ drug - Tagrisso (osimertinib mesylate), the company's flagship treatment for non-small cell lung cancer- failed to make the cut. The company sought to set reimbursement standards for Tagrisso in combination with pemetrexed plus platinum-based chemotherapy in the first-line treatment of patients with locally advanced or metastatic non-squamous NSCLC with an EGFR exon 19 deletion or exon 21 (L858R) substitution mutation, but the application was not accepted. On the same day, the CDDC deliberated on reimbursement standard improvements proposed by medical societies. As a result, requests to improve the phrase - “failed chemotherapy including docetaxel” - wording in the subjects for prostate cancer chemotherapy, and suggestions regarding the administration of palliative therapy in case of recurrence/metastasis during or after the administration of adjuvant therapy, were accepted.
- Policy
- NHIS-Roche enters pricing negotiations for Perjeta’s reimb
- by Lee, Tak-Sun Nov 12, 2024 05:50am
- Roche has started drug price negotiations with the National Health Insurance Service for its breast cancer drug Perjeta (pertuzumab). The negotiations are expected to be held on the drugs whose reimbursement standards were set by the Cancer Disease Review Committee in May. According to industry sources on the 11th, the NHIS recently included Perjeta in its list of drug price negotiation subjects in November. The items subject to drug price negotiation are new drugs, drugs that are not subject to drug price negotiations, and drugs with expanded use. This negotiation appears to be a case of expanded scope of use, as Perjeta was already listed for reimbursement in June 2017. In its May meeting, the NHIS’s Cancer Disease Review Committee set reimbursement standards for Perjeta. Currently, Perjeta is reimbursed for HER2-positive metastatic or unresectable locally recurrent breast cancer. It also applied a 30% coinsurance rate as an adjuvant therapy for breast cancer. The newly reimbursed indication is for lymph node-positive HER2-positive patients who are eligible for pertuzumab-based neoadjuvant therapy. The reimbursement standard was established according to recommendations from the medical community. In December last year, HIRA received feedback from medical associations, including the Korean Medical Association and the Korean Hospital Association, regarding its reimbursement criteria. The proposed item for anti-cancer drugs was then discussed in detail by the TFT and was presented to the Cancer Disease Review Committee in June. In breast cancer, pertuzumab is the only drug for the indication. Clinical trials have shown the effectiveness of pertuzumab in patients with lymph node-positive breast cancer. However, in the past, only neoadjuvant therapy with pertuzumab for early breast cancer patients was covered with selective reimbursement, and adjuvant therapy was not covered, so many voices were calling for reimbursement expansions. In that context, the newly set reimbursement standards are an example of access being strengthened through the voice of the field. However, the final expansion of reimbursement benefits will be finalized only after completing negotiations with the National Health Insurance Service. “Recently, the reimbursement expansions proposed by the medical community and academic societies, not pharmaceutical companies, are entering the negotiation stage,” said an NHIS official, explaining, ”We are closely examining the agendas because the measures for sharing those drugs’ financial burden has not been sufficiently discussed yet.” Meanwhile, Perjeta continues to build on its reputation as a blockbuster breast cancer drug that generated KRW 111.3 billion in sales last year, according to IQVIA. Roche recently launched Phesgo, a combination of Perjeta and Herceptin, to continue to expand its share of the breast cancer treatment market.
- Policy
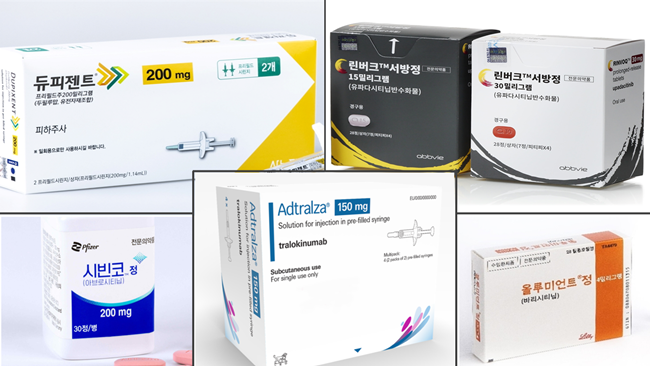
- Drug switching for atopic dermatitis measure submitted
- by Lee, Tak-Sun Nov 07, 2024 05:47am
- Pharmaceutical companies have submitted their measures for voluntary drug price reduction as part of financial allotment following expanded reimbursement. Discussions about allowing drug switching between biological agents and JAK inhibitors used to treat severe atopic dermatitis are speeding up. The Health Insurance Review and Assessment Service (HIRA) has already prepared the reimbursement criteria, and pharmaceutical companies have submitted their measures for voluntary drug price reduction as part of financial allotment following expanded reimbursement. Attention is drawn to whether it will pass the Drug Reimbursement Evaluation Committee (DREC) review, the final stage for reviewing reimbursement appropriateness. According to industry sources on November 6th, pharmaceutical companies Pfizer for Cibinqo and Lily for Olumiant submitted their financial impact analysis to the HIRA. The drug pricing reduction system for expanded scope of use requires the submission of financial impact analysis reports. The government excludes drug price reduction when the estimated additional claim amount following the expanded scope of use is below KRW 1.5 billion. The drug price reduction is applied for products over KRW 1.5 billion and below KRW 10 billion. In this case, pharmaceutical companies are required to submit a financial impact analysis, including measures to voluntarily lower prices, to the HIRA. In mid-October, the HIRA required each pharmaceutical company to submit financial impact analysis. Earlier this month, pharmaceutical companies have started to submit their reports. The issue of allowing drug switching for the treatment of severe atopic dermatitis was dealt with in the parliamentary audit held last month, so the health and welfare authority appears to be rushing the measure. The HIRA has been discussing with experts since September about whether to allow drug switching between biological agents and JAK inhibitors. The reimbursement criteria have been prepared, reflecting the latest evidence and clinical application. The remaining step is to minimize the financial impact following the expanded scope of use. Pharmaceutical companies' percentage of voluntary drug price reduction is the key. As pharmaceutical companies have submitted their measures for voluntary price reduction, the the Drug Reimbursement Evaluation Committee (DREC) review of the HIRA will make a final decision. The 11th DREC review is scheduled for July 2024. Attention is drawn to whether drug switching for severe atopic dermatitis will be considered for the agenda. When it passes the DREC review, the final reimbursement expansion will be decided through negotiation with the National Health Insurance Service (NHIS). Meanwhile, treatments for severe atopic dermatitis have been listed for reimbursement, starting with the biological agent, 'Dupixent Inj,' approved in January 2020. It was followed by the JAK inhibitors, Olumniant Tab, Linvoq ER Tab, and Cibinqo Tab. In May, another biological agent, Adtralza PFS, was listed for reimbursement. As a result, patients have more drug options. However, reimbursement and special cases do not cover drug switching between biological agents and JAK inhibitors, so it remains an issue. When clinical practices initially use high-cost drugs, and then the effects seen are not apparent, they may continue administering first-line treatments. Therefore, the medical community has been demanding the allowance of drug switching.
- Policy
- Novartis cuts price of Cosentyx after PVA negotiations
- by Lee, Tak-Sun Nov 07, 2024 05:46am
- Cosentyx UnoReady Pen The price of Novartis’s Cosentyx(secukinumab) is set to be reduced due to its increased use. This is because the National Health Insurance Service recently reached an agreement during Price-Volume Agreement negotiations with the company for Cosentyx. According to industry sources on the 6th, the insurance price ceiling of Cosentyx was adjusted for the second time under the PVA system after 2021. The affected products are the Cosentyx SensoReady Pen and Cosentyx UnoReady Pen. Cosentyx was listed for reimbursement in Korea in August 2017. Currently reimbursed indications include ▲chronic severe plaque psoriasis, ▲active and progressive psoriatic arthritis, and ▲severe active ankylosing spondylitis. According to the market research institution IQVIA, Cosentyx SensorReady Pen has seen an increase in sales every year since its reimbursement. In 2019, sales reached KRW 12.3 billion, then KRW 19.9 billion in 2020, KRW 25.1 billion in 2021, KRW 30.3 billion in 2022, and KRW 31.7 billion in 2023. In addition, Cosentyx UnoReady Pen, a high-dose product that was launched last year, generated sales of KRW 4.5 billion. Due to such high demand, the insurance price ceiling of Cosentyx had been adjusted in 2021 under the PVA system. At the time, the price of Cosentyx Sensoready Pen dropped by 7.3% from KRW 682,938 to KRW 630,084. At the time, 'Type A’ of the PVA negotiations was applied. Type A negotiations are applied to listed new drugs whose claims in the same product category have increased by more than 30% from the expected claims amount. In 2020, the drug had already well exceeded the expected claims amount. Three years have passed, and this year, ‘Type B’ PVA negotiations were applied. Type B negotiations are applied when the claims for the same product group, whose insurance price ceiling had been adjusted by Type A negotiations, or four years passed after the date of initial listing or the date the price ceiling was adjusted through negotiations, have increased by 60% or more than the previous year's claims, or by 10% or more but the increase is more than KRW 5 billion. Since Cosentyx had its price ceiling adjusted through Type A negotiations, it is possible that the additional negotiation for price adjustments was ordered because its claims increased by more than 60% or more than KRW 5 billion over the previous year's claims. Given that Cosentyx Sensoready’s sales grew 5% YoY in 2023 by KRW 1.4 billion (IQVIA), the introduction of Cosentyx UnoReady Pen, which falls in the same product group, may have triggered the PVA negotiation. Combined, the increase in sales amounted to more than KRW 5 billion compared to the previous year. Upon the agreement, the final price of Cosentyx is expected to be announced after deliberation by the Ministry of Health and Welfare’s Health Insurance Policy Review Committee.
- Policy
- 'Eutropin·Biktarvy' price drop amid sales hike
- by Lee, Tak-Sun Nov 06, 2024 05:52am
- Product photos of Eutropin and Biktarvy. Due to the increased volume of usage, drug pricing for 'Eutropin Inj (somatropin, LG Chem)' and 'Biktarvy (Bictegravir/Emtricitabine/Tenofovir Alafenamide, Gilead Science),' which recently showed a sales hike, is expected to be reduced. Sources said on November 5th that the Health Insurance Review and Assessment Service (HIRA) recently agreed on drug pricing adjustment of these products through the 'Type-Na' negotiation. As a result, the final adjusted prices will be listed on the reimbursement list following a review from the Health Insurance Policy Review Committee. Eutropin has been a top-selling growth hormone drug in the Korean market. 'Eutropin S Pen,' introduced in April 2022, is skyrocketing in sales. Eutropin S Pen's expiration date has been extended from 18 months to 24 months, and, based on UBIST, it generated sales of KRW 81.5 billion last year. Eutropin recorded KRW 21.3 billion in sales in the same period. The combined sales growth rate for the two products is 24% compared to last year. Biktarvy also successfully achieved two-digit sales figures. Based on IQVIA last year, it generated sales of KRW 54.5 billion, up 11% from the previous year (KRW 49.1 billion). Biktarvy received the MFDS approval in January 2019, and it has been in sales following reimbursement listing in July. It is a single-capsule combination drug for the treatment of HIV containing three active ingredients: Bictegravir, Emtricitabine, and Tenofovir alafenamide. With Yuhan and Gilead Sciences in a joint-sales agreement, Biktarvy is a top-selling drug in the HIV market. "Eutropin and Biktarvy show rapid growth in the market," an expert in the pharmaceutical industry said. "With the increased usage volume, reducing its ceiling price according to the Price-Volume Agreement (PVA) is inevitable." In 2022, the ceiling prices of Eutropin and Biktarvy were lowered due to the PVA agreement. Eutropin was reduced by 2.9%, and Biktarvy was reduced by 3.0%. Meanwhile, the negotiation of the PVA 'Type-Na' is conducted when the ceiling price is adjusted by the type-Ga price or when the bill amount of the same product has increased by more than 60% or 10% from the previous year's bill, and the increase is more than KRW 5 billion.
- Policy
- How will the new drug review process change with fee hike?
- by Lee, Hye-Kyung Nov 06, 2024 05:52am
- The Ministry of Food and Drug Safety (MFDS) announced plans to raise the fee for new drug approvals to KRW 410 million from January 1 next year. The agency has prepared the approval and review process to implement the plan and has begun collecting industry opinion. According to MFDS’s press corp coverage, the MFDS recently delivered a revised version of the “Operating Procedures for Approval and Examination of New Drug Products (Guideline for public officials)” to the pharmaceutical and biotech industries and relevant associations. The guidelines contain specific measures to implement the “Innovative Measures for New Drug Approval” that was announced by the MFDS on Sept. 9, including the operation of a dedicated review team for each product and prioritizing GMP-GCP on-site inspections. “Upon the announcement of the rise in the approval fee of new drugs under the Innovative Plan for New Drug Approval, the pharmaceutical industry raised the question of whether the actual approval period will be shortened,” said an MFDS official. ”By recruiting reviewers, GMP inspections will be prioritized to be completed within 90 days from the date of the application receipt, and pre-registration of supplementary materials and explanatory meetings will reduce unnecessary delays in the approval process, dramatically shortening the approval period for new drugs from 420 days to 295 days.” The enactment of the Guideline on Operating Procedures for New Drug Approval and Review was promoted in line with the redetermination of new drug approval fees, which will take effect on January 1, 2025, and includes various changes to differentiate it from the existing approval process, such as the formation of a dedicated team, the establishment of explanatory meetings, and the introduction of a procedure for pre-registration of supplementary materials. From next year, when a new drug approval application is filed, MFDS will conduct an independent preliminary review within 7 days. During the preliminary review period, 80% of the fee will be refundable, and the MFDS will check the submission requirements. If there are any missing materials during this process, the applicant will have 14 days to submit them before an “initiation meeting” is held. Given the overall review timeline, the preliminary review process is crucial as data not submitted by the initiation meeting will be difficult to submit later and the application will be categorized as an application that requires primary supplementary data. A key part of this process is the establishment of a dedicated team for each item before the initiation meeting. The head of the approval division will lead the team, and a representative from the approval division will take charge as each item’s manager, and the team will be composed of representatives from ▲safety, efficacy, ▲quality control, ▲GMP (good manufacturing practice), and ▲GCP (good clinical practice). In addition, an initiation meeting is held within 14 days of receipt to coordinate the entire approval and review process and to provide the applicant with the necessary materials and procedures. The initiation meeting may be held face-to-face, via video, or in parallel, which is expected to increase the efficiency of the new drug review process. According to the proposed Operating Procedures for Approval and Examination of New Drug Products, GMP inspections will be conducted within 90 days from the date of application receipt, and GCP inspections will be conducted within 60 days after the first supplement. By accelerating the inspection schedule compared to the existing procedure, the verification required for the manufacturing and clinical management procedure will be completed at an earlier stage. This is intended to speed up the approval process and ensure adequate quality control. A number of improvements have also been made to the supplement requests. Previously, there were only first and second supplementary notifications, but the reform introduces a first supplementary request briefing session and a second supplementary request briefing session to ensure that the applicant fully understands the supplementary request. In particular, the explanatory meetings provide detailed information on the scope and requirements of the required materials and provide time to answer the applicant’s questions. In particular, for the first round of supplemental data submissions, a pre-registration process and a request for an information session can be made by the applicant. Applicants can pre-register their supplementary data and request the KFDA to hold an explanatory meeting. This allows the adequacy of the supplementary data to be reviewed in advance, reducing additional supplementary work and increasing the efficiency of the approval process. In addition, a final meeting will be held 5 days before the final approval target date to discuss the results of the approval review. “In addition to the effect of shortening the approval period, the revised procedure will improve the transparency of the approval and review process and help pharmaceutical and biotech companies develop new drugs efficiently while protecting the public's health,” said an MFDS official. ”We will collect opinions from relevant associations and industries to prepare the final draft and continue to optimize and implement the approval review service for the development of the domestic pharmaceutical industry.”
- Policy
- Reimb standards that prevent abuse of HA Eye Drops imminent
- by Lee, Tak-Sun Nov 05, 2024 05:45am
- Health authorities are expected to establish reimbursement standards to prevent the misuse of hyaluronic acid eye drops after failing to reach a conclusion during last year's reimbursement adequacy evaluations. It is reported that the Ministry of Health and Welfare is preparing an administrative notice to announce the reimbursement standards set by HIRA. HIRA’s reimbursement standard plan is expected to focus on the issue of abuse and misuse of HA eye drops and includes some restrictions on the number of uses and combinations. According to industry sources on the 3rd, HIRA’s proposed salary standards for HA eye drops are expected to be administratively notified soon. HA eye drops received reimbursement reevaluations in 2023, but no conclusion was made at the time. In September last year, during the first deliberation by the Drug Reimbursement Evaluation Committee, the committee determined that its use for “exogenous diseases such as postoperative, pharmaceutical, trauma, and contact lens wear” is not adequate for reimbursement. On the other hand, endogenous diseases such as Sjögren's syndrome, skin mucosal eye syndrome, and dry eye syndrome were deemed reimbursable, and it was concluded that it was necessary to set reimbursement standards such as single prescription per patient visit and total number of prescriptions per patient per year to encourage its appropriate use. However, opposition arose due to reasons such as weakened access and increased costs for elderly patients who use HA eye drops, and the issue was raised during the NA audit. As a result, DREC was unable to make a conclusion during its second deliberation and decided to review it further. At the MOHW’s Health Insurance Policy Review Committee meeting, which was held in December last year, the committee also said, “In the case of HA eye drops, we will make a final decision at a later date based on the evaluation results as it is necessary to consider setting the reimbursement standard for disposable eye drops as a whole in consideration of the users’ switch to other disposable eye drops.” So in the light of the new year, the health authorities reportedly came up with a reimbursement plan focused on preventing misuse. “It is expected that there will be some restrictions on the number of doses, combined use, etc.,” said a pharmaceutical industry insider, adding, ”The new reimbursement standards will have more restrictions on its use than now, but I understand that they are more aimed at preventing abuse.” After the first round of deliberations last year, there was a proposal to limit the number of boxes containing 60 individual vials to 4 per year. The pharmaceutical industry opposed the proposal, saying it was too restrictive. The current proposal, while still limiting the number, is said to be more eased than the 4 boxes per year. HIRA reportedly prepared a reimbursement standard and reported it to MOHW. The industry believes that MOHW will issue an administrative notice soon after a long discussion. HA eye drop prescriptions amount to around KRW 230 billion a year. They are widely used for eye diseases. Therefore, it will be interesting to see how the proposed reimbursement standard will affect the drug market.
- Policy
- Anticipating reimb for DPP4·SGLT2 combination drugs
- by Lee, Jeong-Hwan Nov 01, 2024 05:51am
- The government has announced a plan to address the necessity of the National Health Insurance reimbursement·expansion for two-drug combination drugs containing DPP-4 inhibitors and SGLT-2 inhibitors for the treatment of type 2 diabetes. In South Korea, reimbursement for combination drugs containing DPP-4 inhibitors and SGLT-2 inhibitors is only provided for three-drug combination therapy that involves an additional prescription of metformin. Approval of reimbursement for two-drug combination therapy, excluding metformin, is expected to offer more treatment options and convenience for diabetes patients while preventing unnecessary national health expenditures. On October 31, the Ministry of Health and Welfare (MOHW) and Health Insurance Review and Assessment Service (HIRA) responded to the question regarding the National Health Insurance coverage of type 2 diabetes treatments asked by Rep. Seo Miwha, a member of the People Power Party, during the parliamentary audit. Rep. Seo pointed out that reimbursement of combination drugs containing SGLT-2 inhibitors and DPP-4 inhibitors for treating diabetes must be approved to broaden treatment choices for diabetes. Rep. Seo stated that the current reimbursement for combination drugs is complicated for physicians to prescribe and restricts treatment choices for patients. Since May 2023, the scope of reimbursement for combination drugs containing DPP-4 inhibtors and SGLT-2 inhibitors prescribed to patients with type 2 diabetes has been expanded·changed so that it can be reimbursed when metformin is additionally prescribed. The problem is that the use of SGLT-2 inhibitors and DPP-4 inhibitors in combination or a combination drug is not covered by the National Health Insurance reimbursement. The current reimbursement policy is illogical for diabetes treatment because patients who can benefit simply from two-drug combination therapy are unnecessarily prescribed three-drug combination therapy because three-drug combination therapy is reimbursed, but two-drug combination drug are not. The HIRA responded to such criticism that they would review the need to expand the National Health Insurance reimbursement for a two-drug combination containing SGLT-2 inhibitors and DPP-4 inhibitors or a combination drug. "We will assess the safety·clinical utility of oral combination drugs for treating diabetes and communicate with related associations so that improved policy for two-drug combination drugs can be generalized," the MOHW said. "However, reimbursement expansion of diabetes drugs requires an impact on the National Health finance. We will discuss this with related associations." The HIRA explained the reason for the exclusion of two-drug combination drugs from the current reimbursement list, and they announced a plan to pursue improvements to the scope of reimbursement. "In 2018, we have written reimbursement criteria for the concurrent use of SGLT-2 inhibitors and DPP-4 inhibitors by discussion with an advisory committee. However, we retracted our stance that reimbursement of concurrent use by drug classes is appropriate and decided to maintain the current policy," the HIRA said. "After the previous discussion, we have checked the updated approvals from the Ministry of Food and Drug Safety (MFDS) and assessed the revision plan by comprehensively reviewing the latest resources and expert opinions, such as clinical practice guidelines, clinical research documents." "In addition to restricting the overall general policy for diabetes drugs, we plan to review issues related to reimbursement expansion for the combination therapy containing SGLT-2 inhibitors+DPP-4 inhibitors, prescription ease, and patient choices by discussing with related associations and experts," they added.