- LOGIN
- MemberShip
- 2026-04-29 06:35:10
- Policy
- Pace of expanding low-priced purchase incentive has been adjusted
- by Jung, Heung-Jun Mar 16, 2026 09:25am
- The government is expected to adjust the schedule of its implementation policy, considering the potential side effects of expanding low-priced purchase incentives for medical institutions.While the original plan was to increase the incentive for low-priced purchases from 20% to 50%, officials are now reviewing a plan to lower the target to 35%.According to industry sources on the 16th, the government's fundamental policy direction of transitioning market price reductions into a 'market-linked, transaction-based price system' remains unchanged.However, given the potential negative consequences of a rapid expansion of incentives, the Health Insurance Policy Deliberation Committee is expected to lower the planned increase rate at its meeting this month.The low-price purchase incentive is a system that provides a portion of the savings as a grant to medical institutions when they purchase medicines at a transaction price below the maximum reimbursement limit. Under the current standards notified by the Ministry of Health and Welfare (MOHW), approximately 20% to 30% of the price difference is paid to these institutions.The reform plan released last November included a proposal to expand the incentive payout rate to a maximum of 50%. It is intended to lower actual transaction prices through market competition without relying on government-mandated price cuts.Since the announcement, there have been persistent concerns about overheated price competition and chaos in the distribution order. Critics have pointed out that the side effects of damaging the industry ecosystem could outweigh the benefits of reduced pharmaceutical expenditures.During a recent National Assembly debate on the drug pricing system, specific concerns were raised regarding the potential for rebates following the expansion of these incentives.Hong Seok-hwan, the Policy Director of the Korean Confederation of Trade Unions, criticized the move by stating that rather than the government directly removing the price bubble, the policy induces pharmaceutical companies and hospitals to enter into side agreements at prices lower than the officially notified price, effectively legalizing rebates by guaranteeing the price difference as profit.The government is adjusting the rate of increase in incentives downward to address these concerns. The proposed 35% rate is currently under discussion, and the final payout rate will be decided at this month's Health Insurance Policy Deliberation Committee meeting.Meanwhile, this expansion of low-price purchase incentives applies only to private tertiary general hospitals, general hospitals, clinics, and pharmacies. National and public hospitals are expected to maintain the current 20% rate.
- Policy
- Stepwise price reduction applied from 13th listed product
- by Jung, Heung-Jun Mar 16, 2026 09:25am
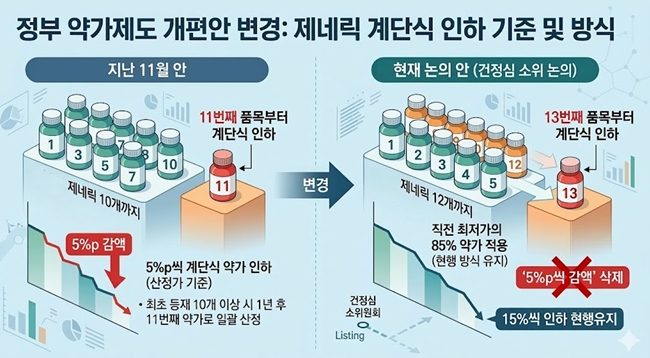
- The government, which had planned to implement stepwise drug price reductions of 5 percentage points starting from the 11th listed product, has decided to revise both the criteria for listing items and the reduction method.The new direction under discussion is to apply stepwise reductions starting from the 13th listed product, while maintaining the current method of applying 85% of the previous lowest price as the new price.According to industry sources on the 16th, the government’s drug pricing system reform proposal discussed at the recent Health Insurance Policy Deliberation Committee (HIPDC) subcommittee differs from the proposal announced in November last year.The stepwise drug price reduction reform plan is expected to undergo partial changes. AI-generated imageThe reform plan from last November included a method whereby “the price of the first generic would be reduced by 5 percentage points starting from the 11th product listing of the same formulation.” This represented a significant strengthening of the current product reduction system, which is applied starting from the 21st listed product.Additionally, the plan stipulated that if there were 10 or more initially listed generics, the price would be uniformly set at the 11th product’s level one year later.At this HIPDC subcommittee meeting, a proposal to apply the stepwise reduction starting from the 13th product was discussed. While the method of reducing the price by 5 percentage points each time would be removed, discussions are focused on maintaining the approach of applying a price set at 85% of the lowest price for subsequent listings. This effectively means maintaining the current reduction rate of 15% applied from the 21st product onward.Products listed at the point where stepwise reductions begin will have their prices adjusted to 85% of the lowest price after one year.For example, if there were 10 products this month and the number exceeds 13 with next month’s listings, the price for the newly listed products will be set at 85% one year later. However, if additional items are listed the following month, their prices would be further reduced by an additional 85% on top of the 85% already applied.Although the threshold number of products used as the basis for stepwise reductions has been slightly relaxed, the system still effectively results in an additional 15% reduction following the initial 15% reduction, depending on the listing timing.However, the details currently under discussion are not yet finalized. There is a possibility that the application method or specific figures could change at the HIPDC meeting on the 26th.Additionally, since the generic drug pricing rate is not clearly defined as being in the “mid-to-high 40% range,” the exact drug price calculations under stepwise reductions will likely be possible only after the HIPDC decision is finalized.
- Policy
- Debate over fast-track listing of new drugs continues
- by Jung, Heung-Jun Mar 12, 2026 08:35am
- Debate continues over the proposed reform of the drug pricing system aimed at shortening the reimbursement listing period for new drugs. On one side are calls to strengthen treatment access, while on the other are concerns that the reform could sharply increase the burden on Korea’s national health insurance budget.While working bodies like HIRA are preparing to strengthen post-listing control, concerns persist about the effectiveness and potential side effects of expedited listing.The Korean Pharmacists for Democratic Society, which previously called for reconsideration of the fast-track listing initiative together with the Citizens' Coalition for Economic Justice (CCEJ) last month, plans to hold a briefing session next week to point out issues in the proposed new drug pricing reform.AI-generated imageOn the 10th, the Korea Alliance of Patient Organizations urged the government to promptly implement the fast-track listing and post-listing evaluation system, arguing that delays in national health insurance reimbursement after regulatory approval for anticancer drugs and rare disease treatments are reducing treatment accessibility.The government recently announced that starting in 2026, it will launch a pilot program for a “fast-track listing–post-evaluation system,” which would shorten the reimbursement listing period for rare disease treatments from the current maximum of 240 days to within 100 days. The alliance called for the swift implementation of the measures.KAPO emphasized, “Rather than blocking entry at the early stage, it is important to establish a sophisticated post-listing evaluation and management system based on treatment performance.”Until recently, attention surrounding the drug pricing reform had focused largely on price cuts for already-listed drugs, while the direction of the fast-track listing reform for new drugs received relatively less attention. The pharmaceutical industry, which has little reason to oppose faster market entry, had been cautiously waiting for details of the implementation plan.However, the issue gained prominence in February when groups including CCEJ, the Korean Association for Serious Diseases, and the Korean Pharmacists for Democratic Society urged reexamination of the fast-track listing policy. They also called for a public hearing on issues including raising the ICER threshold and introducing flexible drug pricing agreements.Criticism calling for broader social discussion is expected to continue this month. The Korean Pharmacists for Democratic Society is expected to hold a briefing on March 18 on the proposed new drug pricing reform and express opposition to the fast-track listing policy.An official from the organization said, “Although there are measures to evaluate outcomes and provide refunds if necessary, there are no clear post-management mechanisms, such as price reductions or market withdrawal, after post-evaluation. As the financial burden on the National Health Insurance is expected to surge, preparing countermeasures must be prioritized.”The official continued, “There are also doubts about whether strengthened post-listing management measures are appropriate for Korea. The briefing will address the impact of the overall new drug pricing reform, including fast-track listing.”Critics also argue that the reform of the new drug pricing system, like the proposed price cuts for generics, lacked sufficient prior discussion.A pharmaceutical industry official said, “As with the generic drug pricing reform, this situation arose because sufficient discussion was not conducted before the reform plan was announced. If there had been even a process to coordinate the implementation measures, the current backlash would not have occurred.”
- Policy
- ‘Active INN prescribing needed for drugs with supply shortages’
- by Jung, Heung-Jun Mar 12, 2026 08:35am
- Han-sook Kim, Director of Health Insurance Policy Division, MOHWThe government said it is reviewing various measures while expressing support for introducing INN (international nonproprietary name) prescribing for drugs with unstable supply.It also stated that it will continue consultations to minimize the impact of the drug pricing reform plan on the field and will further refine the system even after implementation.On the 11th, Han-sook Kim, Director of the Health Insurance Policy Division at MOHW, stated at the National Assembly's drug pricing system discussion forum, " There are many concerns surrounding INN prescribing due to conflicting stakeholder interests. From the perspective of preventing supply instability, it is necessary to actively utilize INN prescribing. We are reviewing various aspects, including the criteria for supply instability and the safety, efficacy, and effectiveness of INN prescribing.”When asked about the direction of the drug pricing reform, Kim said the government would consider the policy’s impact on the field and remain open to consultations and improvements.Director Kim explained, ”The government is also paying close attention to the sustainability of the National Health Insurance finances. We are making multifaceted efforts. Improving unreasonable structures is crucial, and advancing the drug pricing system reforms is part of that effort.“Kim added, “This is an agenda with diverse perspectives. The government cannot clearly predict the impact the reform will have on the field once implemented. The government cannot clearly predict the impact on the field when drug pricing system reforms are implemented. Even after the reform is implemented, we will strengthen monitoring and make improvements if problems arise.”Kim dismissed concerns that the drug pricing reform plan concentrates insurance spending on multinational pharmaceutical companies, and said that it was a misunderstanding.Kim said, “The drug pricing reform could be misunderstood as a policy favorable to the global pharmaceutical industry. But promising companies and technologies must receive investment. If cost savings are generated through the reform, it will be used to properly reward companies investing in R&D.”
- Policy
- Doctors "If INN prescribing is enforced, will boycott the SPD"
- by Kang, Shin-Kook Mar 12, 2026 08:34am
- Doctors who took to the National Assembly to protest the promotion of International Nonproprietary Name (INN) prescribing legislation have said they will go as far as a total boycott of the Separation of Prescribing and Dispensing (SPD) system if the bill is enforced.On the 11th at 4:00 PM, the Korean Medical Association (KMA) Special Committee for public health promotion held a rally in front of the National Assembly Main Building in Yeouido to block the INN prescribing legislation.The doctors gathered at the National Assembly held pickets reading "Will Declare SPD System Annulment if INN Prescribing is Enforced" and demanded an immediate halt to the legislative process.At the scene, Kim Taek-woo, KMA president, emphasized, "INN prescribing is not merely about selecting a chemical component. It is a highly sophisticated professional medical act performed after considering the patient's comprehensive condition. This irrational bill, which prioritizes pharmacy inventory over patient needs when dispensing medication, must be scrapped immediately."The Korean Medical Association (KMA) Special Committee for public health promotion held a rally in front of the National Assembly Main Building in YeouidoKim warned the government and the National Assembly, saying, "Do not trade the public's health for economic logic. While pharmacist groups mislead public opinion by citing ambiguous budget savings, no budget can be more precious than the lives of our citizens."Kim further stressed, "If INN prescribing is enforced, we will regard it as a unilateral breach of the Medical-Pharmaceutical-Government Agreement and declare the total nullification of the SPD system. If our right to prescribe is violated and patient safety is threatened, we will stake everything, including my presidency, on this struggle."Following him, Kim Kyo-woong, Chairman of the KMA representative council, pointed out, "INN prescribing is not simply a systemic change. It is an act that denies the medical judgment of physicians who have precisely diagnosed a patient's condition. Furthermore, it is a highly irresponsible idea that breaks the continuity of treatment and puts patients at risk."Lee Ju-byung, Chairman of the Special Committee to Oppose INN Prescribing, asked, "The new bill states that failure to comply with mandatory INN prescribing will result in up to one year in prison or a fine of up to 10 million KRW. Is this such a serious crime? Who proposed that a doctor should face imprisonment for not prescribing by ingredient name?Lee raised his voice, saying, "Some say doctors prescribe by brand name to receive rebates," adding, "Then, are you advocating for INN prescribing just to receive rebates yourselves?"Lee added, "If the government insists on mandating INN prescribing for the sake of the public, we doctors will, in accordance with the government's will, launch a movement to prescribe only original drugs solely for the benefit of the people."Park Jong-hwan, President of the Medical Association Council for 25 clinics in Seoul, also noted, "On one hand, they say we must implement INN prescribing for public convenience, but on the other hand, they want to forcibly close large-scale pharmacies that the public can use late at night and which offer a wide range of drug choices," adding, "Isn't this an act of inconsistency?"Park stated, "The legislation proposed by Rep. Jang Jong-tae is a self-contradiction," adding, "Both bills contain the words public and patient, but the actual public and patients are nowhere to be found. They only look toward the interests and votes of specific professional interest groups."Park concluded, "I do not know whether it is a National Assembly member's job to pass bills that give all dispensing authority to pharmacists through INN prescribing and protect the interests of small pharmacy owners by regulating large pharmacies, or if this is simply for the benefit of a specific group."
- Policy
- ‘Pricing reform should not be finalized without reporting to NA’
- by Lee, Jeong-Hwan Mar 11, 2026 08:29am
- Rep. Sunmin Kim of the Rebuilding Korea Party criticized the Ministry of Health and Welfare, saying it should not move forward with approving and implementing a drug pricing reform plan— which primarily involves lowering generic drug prices— by having it approved by the Health Insurance Policy Review Committee without reporting to the National Assembly.Kim effectively put the brakes on the ministry after it attempted to proceed with the March schedule for subcommittee and full meetings of the Health Insurance Policy Deliberation Committee (HIPDC) without including any mention of the drug pricing reform plan in its 2026 annual policy briefing to the National Assembly, despite the issue being of the utmost concern to the pharmaceutical industry.National Assembly Health and Welfare Committee Joomin Park of the Democratic Party of Korea also agreed with Kim on the need for a separate briefing on the reform plan. Addressing Health and Welfare Minister Eun Kyeong Jeong, Park said, “Because this is a very important issue, it would be appropriate to provide an additional briefing at the committee’s plenary meeting after concluding your discussions on the reform plan.”At the full committee meeting on the 10th, Minister Jeong responded affirmatively to Rep. Kim's procedural remarks and Chairman Park's request for an additional briefing on the drug pricing system reform plan, saying the ministry would comply.Consequently, it is highly likely that the MOHW will provide a separate briefing on the direction of the drug pricing system reform plan at the full committee meeting of the National Assembly's Welfare Committee this month (March), after subcommittee discussions and before the full committee vote.Currently, the ministry plans to hold a one-point HIPDC subcommittee meeting on March 11, followed by further discussion at another subcommittee meeting on March 18, before bringing the reform plan to the HIPDC plenary meeting on March 26 for approval. This plan includes lowering the pricing calculation rate for already listed generic drugs from the current 53.55% to the 40% range.The pharmaceutical industry has criticized the proposal as a mechanical, across-the-board “lawnmower-style” price cut, presenting 48% as their absolute bottom line for the generic drug calculation rate.With the gap between the MOHW and the pharmaceutical industry over the reform plan showing no signs of narrowing, Rep. Kim raised the issue through a procedural remark as the MOHW attempted to pass the plan without reporting it to the National Assembly.Rep. Kim stated, “After reviewing the MOHW's briefing materials, I question what the most pressing issue in current healthcare policy actually is. From what I understand, the drug pricing system reform is the topic most intensely discussed in the media and policy circles recently.”Kim continued, “I hear that tomorrow and next week, the HIPDC subcommittee will finalize the generic drug price reduction ratio. Following HIPDC deliberations at the end of March, discussions are proceeding with the goal of implementation next January. Yet, such an important policy report was not included among today’s key briefing items.”Kim added, “At this rate, there are concerns that the government could proceed with the drug pricing reform without reporting it to the relevant standing committee of the National Assembly. Therefore, I ask the Chairman to ensure that the MOHW clearly reports on the drug pricing system reform currently being pursued during today's briefing.”When Chair Park asked Minister Jeong whether she could provide an immediate briefing on the reform plan, Jeong replied, “We plan to hold about two more discussions in the HIPDC subcommittee to further coordinate opinions and gather more diverse input from the industry. As the proposal has not yet been finalized, we will review the progress and provide either a written report or a separate briefing.”In response, Park demanded that the MOHW prepare to provide an additional briefing at the committee’s plenary session, given the critical nature of the drug pricing system reform plan being pursued by the MOHW.Park stated, “Since additional processes and procedures remain (regarding the reform plan), individual briefings are fine, but because this is an extremely important issue, it would be better to provide an additional report at the committee’s plenary meeting once the discussions are complete.
- Policy
- MOHW agrees to relax convenience store medicine policy
- by Lee, Jeong-Hwan Mar 11, 2026 08:28am
- The Ministry of Health and Welfare (MOHW) has cast a vote in favor of an amendment to the Pharmaceutical Affairs Act that legislates the '20-item limit' on the number of safe household medicine items, currently prescribed by the Pharmaceutical Affairs Act, to a Presidential Decree (Enforcement Decree) to allow for lower-level legislation.The Ministry also expressed support for a provision that eases the '24-hour operation' requirement, which is a mandatory registration criterion for sales outlets, in eup, myeon, and dong where there are no pharmacies or safe household medicine sales outlets.In addition, the Ministry presented a specific proposal to delay enforcement by one year from implementation date to prepare for various matters related to institutional improvement, such as the establishment of subordinate statutes.The bill currently under discussion is facing significant backlash from the pharmacist community, as it could lead to the complete removal of regulations on the number of safe household medicine items in convenience stores and to the expansion of the sale of general medicines outside pharmacies. However, with the competent MOHW expressing support, the likelihood of its passage has increased.In addition to the MOHW, the Korean Society of Oriental Pharmacy, the Korea Alliance of Patients Organizations, the Consumers Union of Korea, and the Korea Association of Convenience Store Industry also supported the legislation. The Korean Pharmaceutical Association was the only organization to oppose the bill.On the 10th, the amendment to the Pharmaceutical Affairs Act, proposed by Representative Han Ji-ah of the People Power Party, is planned to be tabled at the plenary session of the National Assembly's Health and Welfare Committee.Rep. Han Ji-ah's stands that fixing the number of safe household medicine items in the Pharmaceutical Affairs Act is hindering the ability to respond flexibly and administratively to changes in the pharmaceutical market and environment, as well as to public demand.This is the reason for introducing a bill that provides a delegation provision, allowing the number of safe household medicine items to be determined by Presidential Decree.Rep. Han's proposal also includes a provision to establish the basis for the installation and operation of a Pharmaceutical Policy Deliberation Committee under the Minister of Health and Welfare.Easing the 20-item upper limit on safe household medicine items... Ministry supports, Pharmaceutical Association opposesThe Ministry supported the provision delegating the regulation of the 20-item limit for convenience store medicines, which is currently fixed in the Pharmaceutical Affairs Act, to a Presidential Decree.The MOHW also submitted a supportive opinion on relaxing the 24-hour operation requirement and the registration criterion for sales outlets on a limited basis in eup, myeon, and dong areas where there are no pharmacies or safe household medicine sales outlets, to improve accessibility to safe household medicines.However, the MOHW stated that the enforcement date should be adjusted to 1 year after promulgation to prepare for various matters related to institutional improvement, such as the establishment of subordinate statutes.The Korean Society of Oriental Pharmacy also agreed with the amendment to reorganize the safe household medicine system.The Korea Alliance of Patients Organizations and the Consumers Union also supported it. The Consumers Union also expressed the view that it is appropriate to determine the regulation on the number of items through an Enforcement Rule, an Ordinance of the Ministry of Health and Welfare, rather than a Presidential Decree.The Korea Association of Convenience Store Industry supported the bill while suggesting a modification that would require the MOHW to designate the number of household medicine items after receiving advice from a committee.The Korean Pharmaceutical Association strongly opposed. They pointed out that although various systems to supplement medically underserved areas, such as public late-night pharmacies, health clinics, and the designation of special locations, are already in place, the management and operation of safe household medicine sales outlets and special locations remain insufficient.The Korean Pharmaceutical Association argues that, rather than indiscriminately expanding the convenience store medicine system, the priority should be to evaluate whether the management systems of existing programs are functioning properly and to reorganize the system to ensure safe use.The Korean Pharmaceutical Association stated, "To resolve the pharmacy accessibility of residents in medically underserved areas such as farming and fishing villages, special locations can already be designated according to the Pharmaceutical Affairs Act, and a system is in place to allow the purchase of medicines through designated special locations. Currently, medicine is also accessible through 1,895 health clinics nationwide," and emphasized, "In particular, considering the increase in cases of acetaminophen poisoning, the lack of management of sales outlets and the increase in cases of non-compliance with requirements, and the trend of strengthening regulations abroad, we actively oppose the expansion of safe household medicine items at this point as it is a policy that directly contradicts national health."Establishment of Pharmaceutical Policy Deliberation Committee...Ministry of Health and Welfare, Ministry of the Interior and Safety, etc., all opposedThe MOHW and the Ministry of the Interior and Safety opposed the provision establishing a Pharmaceutical Policy Deliberation Committee, arguing that it would create an environment in which pharmaceutical-related matters, such as medicines, could be discussed regularly.The logic is that, since the Central Pharmaceutical Affairs Council exists and is established, installed, and operated by the MFDS, the establishment of an additional body is unnecessary.The Ministry of the Interior and Safety stated, "The Pharmaceutical Policy Deliberation Committee is an advisory committee under the MOHW, but considering the purpose of the Act on the Establishment and Operation of Committees Under Administrative Agencies, it is necessary to consider plans to expand the functions of the Central Pharmaceutical Affairs Council or utilize the policy advisory committees within the MOHW rather than establishing a separate committee."The Korean Pharmaceutical Association and the Korean Medical Association also submitted opposing views.The Korean Pharmaceutical Association opposed it, stating, "The role of the Pharmaceutical Policy Deliberation Committee in the bill is managed by the Pharmaceutical Policy Division of the MOHW," adding, "The policy planning and drafting are performed by the Ministry's Division of Pharmaceutical Policy, while the Pharmaceutical Policy Deliberation Committee performs policy deliberation and advice. In practice, this would lead to discussing the same matter twice, causing inefficiency and making the responsibility and subject of policy decisions unclear."The Korea Medical Association said, "Since the Central Pharmaceutical Affairs Council (CPAC) is already running, establishing a separate Pharmaceutical Policy Deliberation Committee would be a redundant installation of a committee performing similar functions, which is a waste of administrative power," adding, "There are concerns that it could lead to role conflicts between committees and inefficiency in the policy-making process."
- Policy
- Contaminated COVID vaccines, national petition for special investigation
- by Lee, Jeong-Hwan Mar 10, 2026 08:55am
- Minister of Health and Welfare Jeong Eun KyeongFollowing confirmation by disease control authorities of negligence in the management of foreign substances in COVID-19 vaccines, a national petition has been filed requesting the appointment of a Special Prosecutor to investigate the allegations.With multiple opposition lawmakers raising accountability issues against Minister of Health and Welfare Jeong Eun Kyeong, attention has been drawn to the progress of the petition.On the 6th, a petition was field on the National Assembly's e-People service stating, "We request the introduction of a Special Prosecuter to clearly investigate the foreign substance issues reported during the COVID-19 vaccine management process and the appropriateness of the administrative response."The petitioner demanded a Special Prosecutor investigation into the entire process of reporting and responding to foreign substances in COVID-19 vaccines. The request includes verifying the legality of reporting, recall, and quality control procedures; determining accountability; and conducting a full-scale investigation into potential external pressure or conflict-of-interest involvement.Furthermore, the petitioner urged the National Assembly to disclose the full results of the investigation, improve systems to prevent recurrence, and restore the public's right to know and trust in public health.According to the 'Diagnostics and Analysis of COVID-19 Response Status' report released by the Board of Audit and Inspection of Korea (BAI) on the 23rd of last month, the Korea Disease Control and Prevention Agency (KDCA) failed to notify the Ministry of Food and Drug Safety (MFDS) of foreign substance reports. Instead, they handled the issue by informing only the manufacturers and did not suspend vaccination with the same batch numbers despite the risk.Specifically, between March 2021 and October 2024, the KDCA received 1,285 reports of foreign substances in COVID-19 vaccines from medical institutions but bypassed the MFDS, opting to receive investigation results directly from manufacturers.While the majority of these cases (835, 65%) involved rubber stopper fragments due to usage errors, 127 cases (9.9%) involved hazardous foreign substances, including mold, hair, and silicon dioxide.Notably, because no suspension of administration was ordered for the vaccines containing hazardous substances, approximately 14.2 million doses from those specific batch numbers continued to be administered even after the reports were made.Based on the BAI announcement, the petitioner argued, "There is a need for an independent verification of potential deficiencies in the management and reporting systems, and whether the actions of the KDCA and MFDS complied with relevant laws and manuals," adding, "An objective investigation is also required regarding whether external pressure or conflict-on-interest interests influenced policy decisions during the reporting and management process."The petitioner further asserted, "It must be clarified whether the administrative agency's judgments were made based on public health principles or influenced by specific organizations or companies. Given that this matter directly affects national health, it is difficult to restore trust solely through internal executive branch investigations. The facts and accountability must be clarified through an investigation independent of political interests."Separate from the national petition, the opposition party is holding the Minister of Health and Welfare accountable for the contaminated COVID-19 vaccines.The People Power Party (PPP), citing the BAI report that contaminated vaccines were administered due to management failure during the pandemic, requested that Rep. Choo Mi-ae (Democratic Party), Chairperson of the Legislation and Judiciary Committee, cooperate in holding an emergency inquiry.Shin Dong-wook, Senior Supreme Council Member of the PPP, pointed out during a Supreme Council meeting on the 5th, "We requested the Democratic Party to hold an emergency inquiry into the BAI at the Legislation and Judiciary Committee, but Chairperson Choo is refusing, stating without reason that the committee cannot be convened."Rep. Na Kyung-won, the designated opposition lead for the Legislation and Judiciary Committee, also posted on Facebook yesterday, "According to KDCA data, there were 485,576 reports of adverse reactions, 2,802 deaths, and 1,285 reports of foreign substances. However, vaccinations were not stopped." Rep. Na added, "I will demand an emergency meeting of the Legislation and Judiciary Committee, the immediate withdrawal of government appeals [in vaccine lawsuits], the resignation of former Commissioner Jeong, and a parliamentary investigation."Rep. Kim Mi-ae, the PPP executive secretary of the Health and Welfare Committee, also stated at a PP meeting, "The status of COVID-19 vaccine management is a total failure that seriously threatens national health. It is a clinical experiment conducted by the state on innocent citizens." Rep. Kim urged Minister Jeong, who was the KDCA Commissioner at the time, to "take immediate responsibility, resign, and fully cooperate with the investigation."
- Policy
- Will Briviact become the next Vimpat? Generics near early listing
- by Jung, Heung-Jun Mar 10, 2026 08:55am
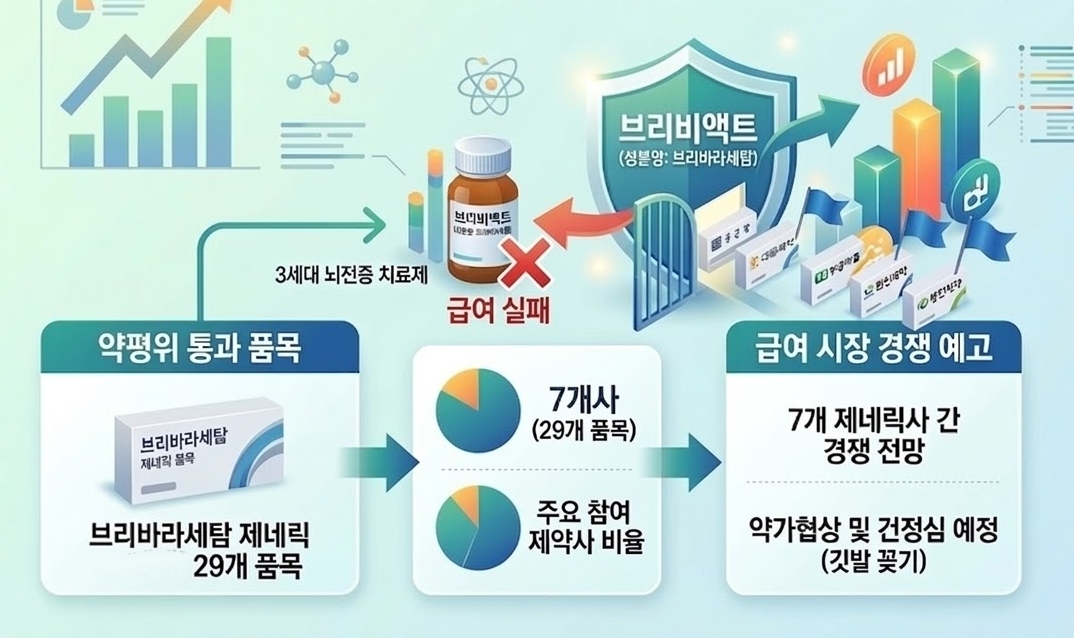
- Attention is focusing on whether generics will be listed first in the reimbursement market, in which the third-generation epilepsy treatment Briviact (brivaracetam) failed to enter.If 7 generic manufacturers, including Chong Kun Dang, Daewoong Pharmaceutical, and Samjin Pharmaceutical, secure reimbursement listing, competition among generic companies is expected in the reimbursed market without the original drug.Generic companies targeting Briviact’s vacancy are on the verge of securing reimbursement listing. AI-generated image.On the 5th, the Drug Reimbursement Evaluation Committee recognized the reimbursement adequacy of 29 epilepsy treatment products containing brivaracetam from 7 domestic pharmaceutical companies. Chong Kun Dang (Briveta Tab), Daewoong Pharmaceutical (Brivatop Tab), Bukwang Pharmaceutical (Bukwang Brifil Tab), Whanin Pharm (Briva Tab), Samjin Pharmaceutical (Bricetam Tab), Myung In Pharmaceutical (Buripam Tab), and Hyundai Pharmaceutical (Brilact Tab) are expected to proceed with listing procedures after price negotiations and review by the Health Insurance Policy Deliberation Committee. The original product is UCB Korea's Brivact, which received domestic approval in 2019. However, it failed to secure reimbursement listing when attempting to enter the insurance market and reportedly did not submit post-marketing surveillance (PMS) data last year. With its patent expiring last February, a series of generic approvals followed. Having passed the DREC hurdle, the generic versions are now on the verge of entering the reimbursement system.If price negotiations are finalized, a unique scenario could unfold where generics secure reimbursement listing before the original drug.Should generics gain early listing, it would mirror the case of UCB Pharma's other epilepsy treatment, ‘Vimpat (lacosamide)’.Vimpat, which was approved in Korea in 2010, ultimately failed to obtain reimbursement listing due to pricing issues, while generic versions of companies such as SK Chemicals’ Vimsk entered the reimbursement market first.According to the market research institution UBIST, Vimsk recorded sales of KRW 4.5 billion last year, marking 32% growth from KRW 3.4 billion the previous year. Its prescription performance has steadily increased over 4 years, from KRW 2.3 billion in 2021.The 7 companies preparing to list brivaracetam generics are also expected to attempt market entry using the same formula.The ultimate question is whether they can clear the drug price hurdle that the original failed to overcome.
- Policy
- Entering into RSA contracts is the key to high-cost drugs
- by Jung, Heung-Jun Mar 10, 2026 08:55am
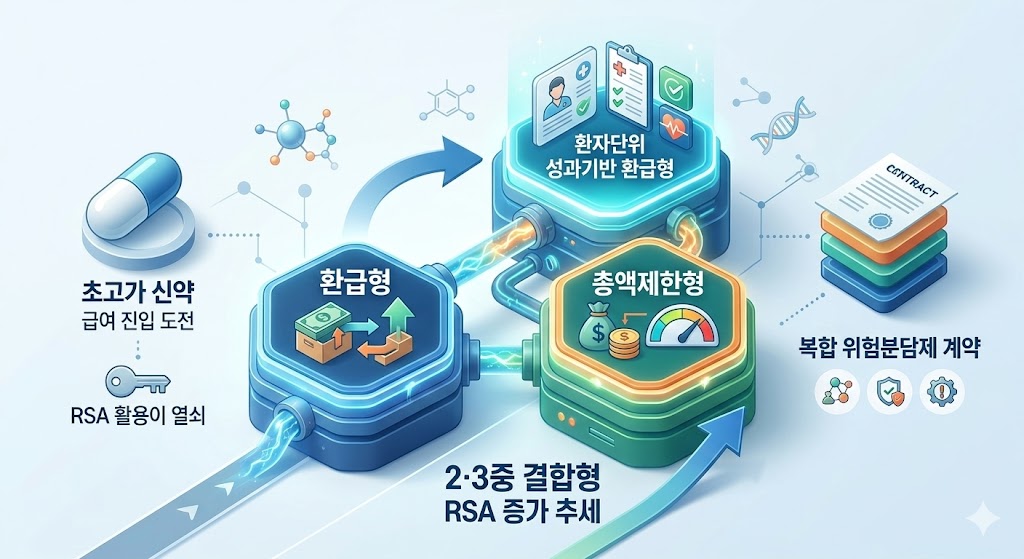
- As the number of ultra-high-cost new drugs seeking insurance coverage grows, more medications are entering double or triple Risk-Sharing Agreement (RSA) contracts.There is a growing trend of triple RSA contracts that combine the standard RSA Refund model with Expenditure Caps and Patient-Level Outcome-Based Refunds.AI-generated imageAccording to industry sources on the 5th, ultra-high-cost drugs recently listed are entering the reimbursement bracket through contracts that combine existing Refund and Expenditure Cap models with Outcome-Based Refunds.The government is strengthening these safety measures to manage financial risks while ensuring access to new drugs; in effect, these hybrid models have become an essential option for crossing the reimbursement threshold.A majority of the new drugs listed or granted expanded coverage this month involved hybrid contracts. Antengene's Xpovio (selinexor) and AstraZeneca Korea's Imjudo and Imfinzi were all subject to both Refund and Expenditure Cap models.For Xpovio, the additional financial requirement due to expanded coverage was estimated at KRW 11.6 billion. However, the government determined that the actual financial impact would be lower when applying two types of RSA.GC Biopharma's Livmarli (maralixibat), a treatment for pruritus in Alagille syndrome, was subject to a triple contract: a Refund, an Expenditure Cap, and a Patient-Level Outcome-Based Refund.The Patient-Level Outcome-Based Refund model tracks treatment results; if pre-agreed targets are not met, the pharmaceutical company must refund a certain amount. It is reported that Livmarli passed the Drug Benefit Evaluation Committee and the Health Insurance Policy Deliberation Committee because GC Biopharma submitted a risk-sharing plan that included this outcome-based refund.Ipsen Korea's Bylvay (odevixibat), a treatment for pruritus in patients with cholestatic liver disease listed last October, is another case of a triple contract.During its cost-effectiveness evaluation, Bylvay was found to have higher annual costs than alternative treatments. However, it was able to clear the listing threshold through the risk-sharing types proposed by the pharmaceutical company. At the time, the estimated annual claim amount was KRW 118.4 billion, but the financial burden was deemed lower through the RSA.As the listing and expansion of reimbursement for immuno-oncology drugs and high-cost new drugs continue to increase, pharmaceutical companies are actively using combinations of Refund, Expenditure Cap, and Outcome-Based Refund models to obtain National Health Insurance coverage.