- LOGIN
- MemberShip
- 2026-04-18 02:23:25
- Product
- Lixiana joins NOAC market race late but takes the lead
- by Byun Kyung A Oct 31, 2019 09:59am
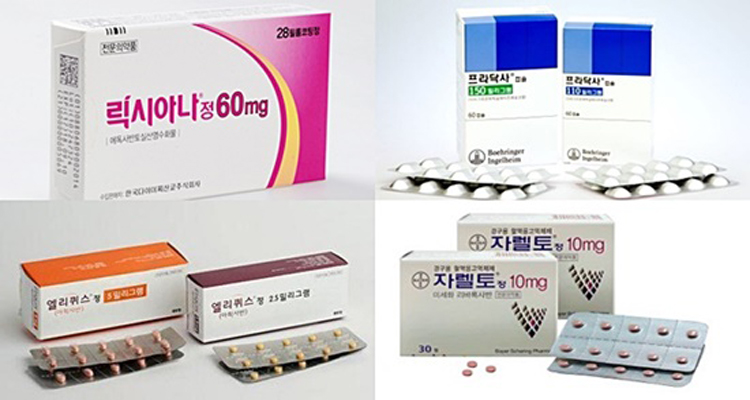
- (Clockwise from upper left) Images of Lixiana, Pradaxa, Xarelto, and Eliquis A follow-on drug in the non-vitamin K antagonist oral anticoagulant (NOAC) market, Lixiana, continues to lead the market. The treatment took the lead from Xarelto in last January for the first time, and it has been the most prescribed drug in the market for nine consecutive months. Pfizer and Bristol-Myers Squibb’s Eliquis had to face a Korean-made generic as a competitor, but its sales performance was unaffected with its original price maintained. On Oct. 28, UBIST, a pharmaceutical market data research firm, reproted Lixiana (edoxaban) marked an accumulated prescription of KRW 40.1 billion in the third quarter. The figure skyrocketed by 68.5 percent from last year same period. Lixiana recorded prescription sale of 14.9 billion won in the third quarter only and marked its record-breaking quarterly performance. The treatment reached outpatient prescription sale of 4 billion won in last January and beat Xarelto’s (rivaroxaban) prescription sale of 3.8 billion won, for the first time. The top spot in the NOAC prescription market has been solidified for nine months straight. The total sale gap between Lixiana and Xarelto’s prescription marked 6.6 billion won and was widened in the third quarter, due Xarelto’s sale dropping 0.2 percent in the third quarter than the year before. The treatment was ranked on second place in the market with 33.5 billion won accumulated prescription sale. Outpatient prescription sales trend of four NOAC items by month (Unit: KRW1 million) Source: UBIST Both internal and external factors played a part in shuffling the NOAC market rank. Bayer’s German production plant issue prolonged the unstable supply management in Korean market, and also the revised pharmaceutical product labeling regulation required all dosage containers to be reprocessed and slowed down Xarelto’s come back. In the meantime, Daiichi Sankyo and Daewoong’s co-promotion revved up the prescription sales of a follow-on drug, Lixiana. Insider from Daiichi Sankyo evaluated, “The healthcare providers and patients were positive about Lixiana’s better drug compliance with once-daily regimen, and improved safety for patients backed by Phase 3. The long-lasting co-promotion partnership with Daewoong, started from Sevika HCT deal, also created a great synergy effect boosting the sales performance”. Monthly prescription sales trend for Eliquis and apixaban generics (Unit: KRW) Source: UBIST Eliquis cumulated 31.3 billion won prescription sales this year, showing 32.1 percent surge than the year before. As of the third quarter, difference in accumulated prescription sales between Xarelto and Eliquis is only about 2.1 billion won. Eliquis was the first NOAC original to compete against generics, but its sales were not influenced as it maintained its original price. After the Korean Supreme Court in last June invalidated drug patent protecting Eliquis, the drug now has Korean-made generics competitors from Chong Kun Dang, Yoo Young, Yuhan, Huons, and Hanmi. But as Ministry of Health and Welfare has decided to defer Eliquis’ price reduction until the final decision on the treatment’s substance patent case is to be made on coming Dec. 31. Currently, the drug still maintains its initial price of 1,185 won per tablet. On the other hand, Chong Kun Dang’s competing generic with the highest content apixaban is about half the price of Eliquis. Boehringer Ingel Heim’s Pradaxa (dabigatran) marked accumulated prescription sales of 12.4 billion won in the quarter. The company sought for a significant increase in market share with a co-promotion deal with Boryung, but the sales performance did not show much increase than last year with 12.3 billion won.
- Policy
- Weighted pricing benefit abused as permanent price booster
- by Byun Kyung A Oct 31, 2019 09:58am
- The government evaluated the current weighted drug pricing system has been digressed as a permanent pricing benefit. Apparently, 96 percent of items have maintained the benefitted pricing for more than three years, and the authority sees that such practice has distanced itself from the initial objective to secure stable supply. Ministry of Health and Welfare (MOHW) submitted a statement answering the National Assembly Health and Welfare Committee Audit addressing the issue. Previously, Liberty Korea Party Lawmaker Kim Soon-Rye questioned the ministry about revising drug pricing system and strengthening competitiveness of Korean companies. In summer, MOHW presented revised 'Decision-making and Modification Standard for Drug Item' and unveiled weighted pricing system revision plan as a part of generic pricing system revision. The system was revised to set one year period of weighted pricing for synthetics and biopharmaceuticals, but provides maximum two years in case number of companies supplying the equivalent generics is less than three. The revision also established generic drug pricing standard and pricing for multi and single-use eye drops. On the revised weighted pricing system, MOHW explained “The initial objective of the system was to stabilize drug supply (weighted pricing for generics with less than three suppliers) and to induce soft landing for a generic entering the market where the original is lowering its price, from 100 percent to 70, and then to 50 percent.” “The revision was planned to keep the regulation faithful to its original objective maintaining stable drug distribution”, the ministry added. And the government emphasized its justification of drug pricing system revision as “244 out of 254 items, or 95 percent of the benefited items have been maintaining its increased price for more than three years, abusing the system as a permanent price boosting tool”. The ministry also ensured it would thoroughly review individual cases that need special support to stabilize drug supply. The statement added MOHW’s commitment to contribute strengthening Korean pharmaceutical company’s global competitiveness by executing the Biohealth Industry Innovation Strategy and Pharmaceutical Industry Fostering and Support Master Plan.
- Product
- Maviret takes up 83% of HCV treatment market share
- by Byun Kyung A Oct 31, 2019 09:41am
- Maviret product image Abbvie broke through the hepatitis C virus (HCV) treatment market and dominated 83 percent of oral outpatient prescription market only with its pan-genotype HCV treatment, Maviret, launched last year. Gilead once dominated the market with two items, but their prescription ratio shriveled down to 12 percent. On Oct. 30, a pharmaceutical market research agency, UBIST reported this year’s third quarter outpatient prescription sales of eight direct-acting antiviral (DAA) regimen HCV treatments recorded 13.2 billion won, soaring 41.4 percent from last year’s third quarter at 9.3 billion won. Abbvie’s Maviret prescription skyrocketed from the launch in last year September, and brought back up then descending total volume of HCV outpatient prescription market. The market had plummeted to 9.3 billion won in September last year, but turned around with Maviret’s launch. Outpatient prescription sales trend of major hepatitis C virus treatments (Unit: KRW 1 million) Source: UBIST This year’s third quarter outpatient prescription sales of Maviret reached 10.9 billion won. The sales easily doubled since last year’s fourth quarter with 4.2 billion won. As its accumulated prescription sales this year marked 31.1 billion won, Maviret is projected to make over 40 billion won by the end of the year. Taking up 82.9 percent of the eight DAA regimen treatments’ outpatient prescription sales, Maviret affirmed its unmatched position in the market. Maviret is the first treatment approved in Korea for chronic HCV infection in adults across all major genotypes. It is a pan-genotype ribavirin-free treatment that combines glecaprevir (100mg), an NS3/4A protease inhibitor, and pibrentasvir (40mg), an NS5A inhibitor, dosed once-daily as three oral tablets. Industry insiders view Maviret rapidly took over the market as it shortened drug treatment period by a month, compared to other DAA regimen. The treatment also mainly targets for patients without cirrhosis and who are new to treatment, the condition most of hepatitis C patients have. Recently, Maviret was able to improve consumption convenience as FDA approved of the drug shortening treatment period of chronic hepatitis C patients with cirrhosis and who are new to treatment, from 12 weeks to eight weeks. Sources also report Ministry of Food and Drug Safety’s approval on the expanded indication is imminent as related application has been submitted. However, due to the fact number of HCV patients is limited and the virus has fairly high full recovery rate, it is unclear if Maviret’s golden days would last long. In fact, Maviret’s prescription sales growth has turned from the third quarter. The total prescription soared every quarter since its launch and peaked in the second quarter, but it’s the figure dropped 9.1 percent in just about three months. Meanwhile, a former HCV treatment market leader, Gilead Sciences seems to have lost a big cut from its own market share. Sovaldi marked 18.1 billion won in last year’s first quarter, but its third quarter prescription sales in this year plunged to 4.68 billion won. Two top selling products of Gilead, Sovaldi and Harvoni, made total prescription of 1.5 billion won. The two drugs combined accumulated prescription sales of 5 billion won, merely taking up 11.7 percent of the whole hepatitis C treatment market. BMS’ Daklinza and Sunvepra combined marked outpatient prescription sales of 4.5 billion won in the third quarter, which is about one-tenth of what they had made last year same quarter. Launched around same season in the second quarter of 2017, MSD’s Zepatier and Abbvie’s Viekira and Exviera watched their sales continue dropping after the launch of Maviret and had short period of sales peak. In the third quarter, Zepatier marked prescription sales of 700 million won, whereas prescription sales for Viekira and Exviera were not even counted from last July. Abbvie insider commented, “Demand for Viekira and Exviera has decreased after Maviret was launched. There isn’t any issue with supply from the company”.
- Product
- Government likely to list Zejula in December
- by Byun Kyung A Oct 31, 2019 09:36am
- Sources predict Zejula, an ovarian cancer treatment, would get listed for healthcare reimbursement in coming December. According to an industry insider on Oct. 16, Takeda Pharmaceuticals Korea is waiting for Health Insurance Policy Deliberation Committee’s (HIPDC) deliberation, after recently reaching an agreement with National Health Insurance Service (NHIS) on drug pricing of Zejula (niraparib), a poly (ADP-ribose) polymerase (PARP) inhibitor. The niraparib treatment has been passed by Drug Reimbursement Evaluation Committee of Health Insurance Review and Assessment Service (HIRA) only after four months it was approved in last July. Zejula can be prescribed as a maintenance treatment for adult patients with recurrent epithelial ovarian cancer, including fallopian tube or primary peritoneal cancer, who are in a complete or partial response to platinum-based chemotherapy. However, the National Health Insurance (NHI) reimbursement would be first available for BRCA mutation patients only. Zejula was approved based on results of Phase 3 trials (ENGOT-OV16/NOVA). Progression-free survival (PFS) of patients taking Zejula, with or without BRCA mutation, showed a meaningful extension than the the control group. Moreover, the treatment proved its efficacy through PRIMA trial testing as a first-line treatment for ovarian cancer, regardless of BRCA mutation. In Korea, AstraZeneca’s Lynparza was listed for NHI reimbursement as a first PARP inhibitor. Lynparza was exempted from pharmacoeconomic analysis and was listed as reimbursed drug with expenditure cap risk sharing agreement (RSA) in October, 2017. However, the reimbursement benefit was suspended for some patients from last January as it was initially listed as post-chemotherapy maintenance therapy up to 15 months. From then on, AstraZeneca underwent reimbursement expansion talks with Korean government and lifted limitation on the fixed period of 15-month since last May.
- Policy
- For reimbursed drug, efficacy and cost-efficiency come first
- by Byun Kyung A Oct 31, 2019 09:34am
- On the last day of the 20th National Assembly Annual Audit for the Health Insurance Review and Assessment Service (HIRA), half the questions were dedicated to pharmaceutical affairs. The lawmakers of the NA Health and Welfare Committee questioned HIRA about NHI reimbursement reevaluation on dementia treatment choline alfoscerate, reimbursement expansion on NOAC Xarelto, and reimbursement expansion on the anticancer treatment reflecting its frequent non-reimbursed off-label use as ophthalmic solution. Some lawmakers claimed the General Principle of Healthcare Reimbursement on liquid solutions, like syrup and suspensions, should be revised and expand utilization cap eligible for reimbursement. As always, however, HIRA had a strictly basic answer for the said topics and stated, “The issues addressed would be sufficiently reviewed when clinical efficacy and cost-efficiency are proven”. Below is Daily Pharm’s summary of HIRA’s written answer submitted to the NA on Oct. 28. ◆Reimbursement reevaluation on choline alfoscerate: The current system does not stipulate a reevaluation for NHI reimbursement based on clinical efficacy, except for special cases of Ministry of Food and Drug Safety (MFDS) revoking an approval. The government's National Health Insurance Comprehensive Plan is to establish a pharmaceutical reevaluation system considering clinical efficacy of listed drug, financial impact and healthcare coverage listing status in foreign countries. HIRA, then, plans to have Drug Post-evaluation Subcommittee under Drug Reimbursement Evaluation Committee (DREC) to conduct NHI reimbursement feasibility reevaluation with the new system. Particularly, HIRA official stressed uncertainty of choline alfoscerate “has been questioned constantly” and that the agency would “establish reevaluation system promptly for it”. The dementia treatment is usually sold as a health functional food in other countries. ◆Expanded reimbursement benefit on Xarelto: Medical industry urges the health authority to grant NHI benefit on new oral anticoagulant (NOAC) Xarelto (rivaroxaban) to high-risk patients with coronary artery disease (CAD), specifically for cases of atrial fibrillation (AF) before and after catheter ablation and electrical cardiodiversion, nonvalvular AF with hypertrophic cardiomyopathy, and nonvalvular AF with CHA₂DS₂-VASc score 1. At the moment, Brilinta (ticagrelor) and Xarelto are listed for reimbursement as antiplatelets, and the benefit for Xarelto only covers high-risk patients with nonvalvular AF. HIRA answered, “As medical academic society has requested expanding reimbursement benefit on Xarelto, the agency plans to promptly review additional clinical evidences, such as revised guideline in foreign countries”, and the treatment’s “reimbursement would be expanded depending on clinically proven efficacy”. ◆Revising General Principle for syrup and suspensions: The current General Principle on Healthcare Reimbursement Criteria and Method stipulates granting NHI reimbursement benefit on pharmaceutical syrup and suspensions, also available in types of table or capsule with equivalent ingredient, in following cases; prescribed to patients younger than 13; patients with old age, dementia or other dysfunctional esophagus unable to swallow; prescribed with antacid, sucralfate, and sodium alginate under approved indication. The National Assembly pointed out the General Principle regarding pharmaceutical liquid solution should be amended and provide healthcare benefit for all Koreans to consume drug more conveniently. But HIRA official explained, “Liquid solution tends to be more expensive than tablet or capsule drugs”, therefore, “the General Principle, on Oct. 1, 2011, stipulated providing benefit to subject drugs meeting cost-efficiency standard under certain medical state and patient condition”. Since 2011, some syrup and suspension with proven cost-efficiency have received reimbursement as an exception to the General Principle. HIRA official added, “The agency would accordingly review the need to amend general reimbursement criteria based on cost-efficiency standard”. ◆Listing Avastin for reimbursement: This year’s National Assembly Audit addressed promptly providing reimbursement for non-reimbursed off-label treatment approved to be used. The issue refers to the use of anticancer treatment Avastin in ophthalmology as a non-reimbursed off-label treatment for macular generation. After consulting with Ministry of Food and Drug Safety (MFDS), HIRA allowed request for use of non-reimbursed treatment at clinics without an institutional review board (IRB) by revising ‘Standard and Procedure of Requesting Usage Approval of Non-reimbursed Off-label Drug’ this month. HIRA stated it would consider providing healthcare reimbursement benefit in the future, when the legitimately used off-label drugs meet clinical efficacy and cost-efficiency standards. ◆Expanding RSA for follow-on drugs: As the RSA subject regulation for severe disease has been revised in last July, HIRA plans to positively review feasibility of expanding RSA subject for follow-on drugs after collecting public opinions. ◆Preventing illegal drug distribution: HIRA has decided to upgrade monitoring system to better manage all drug distribution information and to utilize the collected information properly through the serialization system. HIRA currently requires a serial number to be labeled on minimal drug distribution unit container for the health authority to track individual unit in all phase of distribution, from manufacturing to import, distribution, and consumption. In last May, HIRA cooperated with Seoul city community police to investigate illegal distribution of a weight-loss medicine Saxenda injection. ◆Drug pricing standard for the revised Generic Pricing Policy: The latest revision in the Generic Drug Pricing Policy stipulates drug pricing differentiated with compensation for cost, time and investment spent on generic development, and revised weighted pricing system. Nonetheless, the pricing standard for incrementally modified new drug is same as before. As the new weighted pricing policy could bring down prices of some incrementally modified drugs (IMD), HIRA plans to adequately amend the standard with Ministry of Health and Welfare. HIRA official said, “IMDs are mostly developed by Korean pharmaceutical companies, so drug pricing benefit without limitation on IMD could cause international trade discrepancy as unfairly favorable benefit for Korean companies only”, but “the agency would continue to talk to other related ministries and industry about other means to promote development of IMD with better clinical efficacy”. ◆Revising PE analysis review process: In Australia and Canada, a company is responsible for submitting pharmaco-economic analysis and a public agency is responsible for reviewing the submitted material. But in Korea, pharmaceutical companies have difficulties editing submitted PE analysis report. Lawmakers claimed Korea should adopt ‘Application Registration System’ to prevent such inconvenience. HIRA official answered, “it would be reviewed in detail, surveying overseas cases and current conditions in Korea”.
- Policy
- Jext, only distributed to KOEDC for profits
- by Lee, Jeong-Hwan
- The company that exclusively deals with one of urgent drugs, Jext used for allergic reaction Shock (Anaphylaxis) was criticized for distributing drugs only through KOEDC( Korea orphan & Essential Drug Centers ) for profit. Even though Jext was listed insurance registration last July and it is possible for the company to make direct distribution, The price between general reimbursement and KOEDC reimbursement has big difference. So, Jext distributed only to KOEDC. According to the patients and KOEDC on the 11th, Jext has been distributed and sold patients only through KOEDC since domestic reimbursement listed. It is in patients and KOEDC view that KOEDC reimbursement is much higher than general reimbursement, and it makes economic burden to patients. The company says it is not for profit at all. The headquarters regulates the distribution of general reimbursement items, so the company is inevitably unable to distribute the supply. In fact, KOEDC reimbursement price of Jext is ₩134,933 more than double the general reimbursement price is ₩56,670. The company distributes Jext only through KOEDC until insurance registration listed. But it is still on sale only through KOEDC, even though Jext got general reimbursement listed and can be distributed at clinics or retail pharmacies. The reimbursement price of KOEDC is calculated based on the import cost, whereas the general reimbursement price is meticulously formulated through registraion procedure of Health Insurance Review & Assessment Services. It is the majority opinion of reimbursement specialists that it is much more profitable to sell at KOEDC than to distribute Jext at the general imbursement. Furthermore, the distribution of Jext through KOEDC significantly reduces additional marketing and management tasks such as account management costs required for direct distribution. That's one of the reasons why the direct distribution is delayed. However, if the distributor don't handle the medicine reimbursement listed directly for 6 months, the regulatory action is removed. It even raises doubts that the company deliberately distributes Jext only to KOEDC. Regardless of the company's intentions, as a result, patients need to get Jext ony by paying more expensive money through KOEDC because thiere is no distribution volume, even though there is a way to purchase Jext at significantly lower reimbursement. KOEDC official said, the prodcut is not in shortage of distribution, but the the company distributes medicines only to KOEDC and dose not supply them directly. It's reluctant. In the end, patients have to go and buy through KOEDC with higher price for almost 6 months even after reimbursement listed, there has never been a company using this trick so far. The deliberate coordination disregards the purpose of establishing KOEDC and the policy of expanding access to ER medicines for patients. In response to such criticism, the company said that it is not a distribution control for profitability, and will start direct distribution as soon as possible. The company official said, It was true that Jext was distributed only to KOEDC after July when reimbursement listed, but it was not intended. It was a supply disruption at the headquarters in preparation for improved Korean insert, etc. The official added, "The company will import Jext products within this month and supply them directly from next January after our own quality inspection".
- Company
- 'Uplizna' to bring a shift to the NMOSD treatment strategy
- by Son, Hyung Min
- Tanabe Pharma Korea recently held the UPSTREAM Symposium at Voco Seoul Gangnam to celebrate the launch of NMOSD treatment Uplizna in South Korea.New treatment strategies are emerging for neuromyelitis optica spectrum disorder (NMOSD), a condition where a single relapse can lead to lifelong disability. This shift has been brought about by the introduction of 'Uplizna', a new drug targeting CD19 B cells, for NMOSD treatment in South Korea. Uplizna has been shown to significantly reduce the risk of relapse in AQP4 antibody-positive patients, and medical professionals anticipate that this treatment option will provide patients with a better choice in terms of mechanism and efficacy.Tanabe Pharma Korea recently held the UPSTREAM Symposium at Voco Seoul Gangnam to celebrate the launch of Uplizna (inebilizumab)in South Korea.Professor Ho Jin Kim of the Department of Neurology at the National Cancer Center served as the chairperson. Professor Ki Hoon Kim of the Department of Neurology at Severance Hospital and Professor Jeeyoung Oh of the Department of Neurology at Konkuk University Medical Center delivered lectures titled ▲Optimizing the treatment with inebilizumab after rituximab and ▲inebilizumab in practice: identifying appropriate patients, respectively.Uplizna is a targeted therapy for adult patients with AQP4 antibody-positive NMOSD. It works by targeting and depleting CD19+ B-cells, thereby reducing attacks (relapses) caused by the immune system targeting the optic nerve and spinal cord.The treatment received U.S. FDA approval in 2020 and was authorized in South Korea in 2021. Tanabe Pharma Korea is currently proceeding with the reimbursement listing process for the drug.During the symposium, Professor Ki Hoon Kim began by highlighting B-cells and the AQP4-IgG production pathway as core elements of NMOSD pathophysiology.The professor explained, "Plasma cells are directly linked to the clinical deterioration of NMOSD. Unlike rituximab, which targets only CD20, Uplizna depletes cells up to the pre-CD19 stage, allowing for an approach closer to the underlying cause of the disease."NMOSD is a rare autoimmune disease characterized by unpredictable, repeated relapses of optic neuritis and myelitis, leading to severe disabilities such as eye pain, blindness, and paraplegia. Approximately seven out of ten NMOSD patients are AQP4 antibody-positive; the formation of these antibodies activates the complement system, which can cause necrosis in the optic nerve and spinal cord.Notably, 80–90% of patients experience recurrent relapses, thus even a single event can result in fatal outcomes. These symptoms are often irreversible and difficult to recover from, necessitating rapid acute-phase treatment fully.Previously, NMOSD relapse relied on high-dose steroids or immunosuppressants to suppress symptoms or used rituximab or 'tocilizumab (product name: Actemra)' to prevent relapses. However, as the relapse suppression effects of these treatments were limited, there was a high demand for new options.Rituximab' clinical limitations have been pointed out. These include non-unified administration protocols, varying B-cell depletion and relapse risks based on FCGR3A genotypes, and high rates of infusion-related reactions (IRR) during the first administration. In contrast, evidence was presented that Uplizna is easy to manage with twice-yearly dosing, reduces the risk of relapse by more than 70% in clinical trials, and cuts the rate of worsening on the Expanded Disability Status Scale (EDSS) by more than half. Professor Kim summarized, "Uplizna is an option that can supplement the structural limitations for patients who do not respond to rituximab."In the second session, Professor Oh focused on the timing of switching therapies, which is a challenge in NMOSD treatment.Professor Oh emphasized, "Defining treatment failure based solely on clear relapses may cause us to miss patients." She presented various clinical patterns, including partial responses, incomplete recovery after severe relapses, and switching due to side effects or infections.Professor Oh also pointed out that due to strict domestic reimbursement criteria, some patients with "disability creep," where disability accumulates slowly without clear relapses, may miss the window for adjusting their treatment strategy.Based on actual patient cases, Professor Oh identified characteristics of patient groups requiring a switch from rituximab to Uplizna.The characteristics include ▲rapid repopulation of CD19+ B-cells, ▲incomplete response due to genotype influence, and ▲difficulty maintaining treatment due to infection burdens such as pneumonia.Professor Oh also highlighted data showing the sustained efficacy of Uplizna.The N-MOmentum study, which served as the basis for approval, was a 28-week randomized, placebo-controlled trial that faithfully reflected the NMOSD patient population in real-world clinical settings by including diverse racial and ethnic groups.In the trial, 89% of the Uplizna group remained relapse-free for 28 weeks, compared to only 58% of the placebo group.Long-term data also showed sustained efficacy, with an annualized relapse rate (ARR) of 0.03 for patients treated with Uplizna for at least 2.5 years, significantly lower than the approximately 1.0 ARR in the placebo group.However, because the open-label period (OLP) was non-blinded and uncontrolled, the results might appear more positive due to patient dropout among those with poor prognoses.Professor Oh assessed that "Uplizna is an option that is not merely as a substitute, but the one that ensures both efficacy and safety when a mechanistic switch is required."Professor Kim concluded, "Because NMOSD is a disease where a single minor relapse can lead to lifelong disability, establishing an initial strategy and determining the appropriate timing for a switch is paramount," adding, "This symposium was meaningful for refining our understanding of mechanism-based treatment and discussing customized decisions for each patient. The introduction of Uplizna will serve as an opportunity to advance NMOSD treatment strategies to the next level."
- Company
- '팬데믹 반짝 수혜' 한국화이자, 2년 배당금 1600억
- by Chon, Seung-Hyun
- [데일리팜=천승현 기자] 한국화이자제약이 2년 연속 대규모 배당을 결정했다. 한국화이자제약은 매년 1248만원 배당 정책을 고수했지만 지난 2년간 1600억원을 모기업에 배당했다. 코로나19 팬데믹 반짝 수혜로 대규모 이익이 발생하면서 고배당을 실시했다.15일 금융감독원에 따르면 한국화이자는 지난해 지급한 배당금은 600억1248만원으로 집계됐다. 중간배당 600억원에 연차배당 1248만원이 추가됐다.한국화이자의 지난해 중간배당은 주식 액면 배당률 6501%가 적용됐다. 주식 1주당 액면금액 5000원보다 60배 이상의 배당이 책정됐다는 의미다. 보통주 17만2104와 우선주 1만2480주를 대상으로 각각 559억원 41억원의 중간배당이 결정됐다.한국화이자는 지난 2023년에 이어 2년 연속 대규모 배당이 실시됐다. 한국화이자는 2023년 중간배당 1000억원과 연차배당 1248만원을 결정한 바 있다. 2023년 중간배당은 액면배당률 1만835%가 적용됐다. 한국화이자의 최대주주는 화이자의 네덜란드 자회사 'PF OFG South Korea 1 B.V.'로 지분 99.99%를 보유하고 있다. 한국화이자가 코로나19 팬데믹 기간 동안 실적이 크게 향상되면서 고배당이 실시된 것으로 분석된다.지난 2020년 한국화이자는 매출 3919억원을 기록했는데 2021년 1조6940억원으로 4배 이상 확대됐고 2022년에는 3조2254억원으로 치솟으며 2년 간 매출이 8배 이상 확대됐다. 지난 2023년 매출은 1조6018억원으로 전년대비 절반 수준으로 줄었지만 2020년과 비교하면 4배 이상 증가한 수치다.한국화이자는 2020년 영업손실 72억원과 순손실 212억원을 기록했지만 2022년에는 영업이익과 순이익이 각각 1201억원과 1195억에 달했다. 2023년 영업이익 592억원과 순이익 849억원을 기록했다.화이자는 코로나19가 전세계로 확산되기 시작한 2020년 3월 독일 바이오앤테크와 손잡고 메신저리보핵산(mRNA) 백신 개발에 나섰다. mRNA 기술을 지닌 바이오앤테크와 대규모 글로벌 임상 경력이 많은 화이자가 만나 시너지를 냈다.화이자는 코로나가 확산된지 1년도 채 되지 않아 95% 예방 효과를 지닌 백신 코미나티 개발에 성공했다. 2020년 12월 미국 식품의약국(FDA) 긴급사용승인을 받았고, 한국에서도 이듬해 3월 긴급사용승인 되며 본격적으로 한국지사를 통해 공급됐다. 이후 화이자는 코로나19 치료제 팍스로비드 개발에도 성공했으며 한국 정부도 이를 구매해 치료제로 활용했다.한국화이자는 매년 배당금을 1248만원으로 유지하는 독특한 배당정책을 지속했다. 한국화이자는 우선주 자본금에 배당률 20%를 적용해 배당금을 산출했다. 한국화이자의 자본금은 총 9억2292만원이다. 이중 보통주(17만2104주) 자본금은 8억6052만원, 우선주(1만2480주) 자본금은 6240만원이다. 우선주 자본금 6240만원의 20%인 1248만원의 배당금이 책정됐다.한국화이자는 지난 2005년부터 20년 동안 4번을 제외하고 모두 '우선주 20%'의 동일한 기준으로 배당금 1248만원이 지급됐다.지난 2017년 배당금이 순이익보다 많은 797억9400만원으로 책정된 바 있다. 당시 보통주(245만5520주)와 우선주(1만2480주) 모두 액면금액 5000원의 660%를 배당률로 결정하면서 배당금 규모가 확대됐다. 2008년에는 1900억원의 배당금이 책정됐다. 당시 6억원 적자를 기록했는데도 액면가 대비 3045%의 배당률을 결정하면서 높은 배당금이 확정됐다.다만 한국화이자의 고배당이 지속될지는 미지수다. 한국화이자는 지난해 매출 7837억원으로 51.1% 감소했다. 같은 기간 영업이익은 638억원에서 272억원으로 57.4% 줄었다. 엔데믹 여파로 인해 실적 부진이 불가피했다. 한국화이자의 작년 매출과 영업이익은 2022년과 비교하면 각각 75.7%, 77.4% 축소됐다.