- LOGIN
- MemberShip
- 2026-04-09 09:45:00
- Company
- Hanmi’s Rolontis post sales of KRW 4.8 bil in H1
- by Chon, Seung-Hyun Sep 05, 2023 05:40am
- Hanmi Pharm’s new drug ‘Rolontis’ has been slowly increasing its influence in the domestic market. In the first half of the year, 2 years into its release, the drug has posted sales of nearly KRW 5 billion. The drug has also been achieving fair results in the early stages of its release in the U.S. According to the pharmaceutical research institution IQVIA, Hanmi Pharm’s Rolontis posted sales of KRW 4.8 billion in 1H and rose over 10 times from the previous year. Rolontis is a new biodrug that Hanmi Pharmaceutical licensed out to Spectrum Pharmaceuticals in 2012. The drug is indicated for the treatment or prevention of neutropenia in cancer patients who receive myelosuppressive chemotherapy. As a granulocyte colony-stimulating factor (G-CSF) class that stimulates the granulocyte to increase neutrophil production, the drug has a similar mechanism of action with Amgen’s blockbuster drug ‘Neulasta (pegfilgrastim).’ In Korea, Rolontis was approved in March as the 33rd homegrown novel drug and listed for reimbursement in November 2021. Quarterly Sales of Rolontis(Unit: KRW ! million, Data: IQVIA) Rolontis exceeded KRW 1 billion in sales in Q4 last year. Sales continued to rise to KRW 2.3 billion and KRW 2.5 billion in Q1 and Q2 this year, respectively. At this trend, sales are expected to exceed KRW 10 billion this year, in only the second year of its release. Rolontis’s cumulative domestic sales have recorded KRW 8 billion. Rolontis is receiving much attention after successfully entering the U.S. market. Rolontis was approved by the U.S. FDA under the brand name Rolvedon in September 2021. The drug was successfully commercialized and released into the U.S. market 10 years after the licensing-out deal was made. With the approval, Rolontis became the first new drug to receive FDA marketing authorization among those being developed by Hanmi Pharm. It is the first new drug to be sold in the US market after being produced at a domestic plant (Pyeongtaek Bio Plant) that has received on-site inspections from the FDA. Rolontis was released in the U.S. market in earnest in October last year. The U.S. neutropenia treatment market is worth KRW 3 trillion a year. Since its launch, Rolontis has been showing smooth performance in the U.S. market. Rolvedon recorded sales of USD 15.6 million (about KRW 20 billion) in the Q1. In Q2, sales amounted to $21 million (about KRW 28 billion), up 34.6% from the previous quarter. Rolvedon initially received FDA approval after the technology was licensed out to Spectrum Pharmaceuticals, and in April, Spectrum was acquired by Assertio Holdings, a pharmaceutical company specializing in central nervous system, pain, and inflammation. In its Q2 performance earnings report, Assertio explained, “The acquisition of the Spectrum and Rolvedon asset has brought significant changes to the company. We plan to maintain a highly effective sales and marketing organization to expand the success of the new asset.”
- Policy
- Evaluating Tagrisso's primary benefit
- by Lee, Jeong-Hwan Sep 05, 2023 05:40am
- The Ministry of Health and Welfare announced that it is conducting a cost-effectiveness evaluation regarding the expansion of health insurance coverage for the first-line treatment of AstraZeneca's lung cancer drug Tagrisso. On the 4th, the Ministry of Health and Welfare responded as follows to a written question from People Power Party Rep. Choi Young-hee, a member of the National Assembly Health and Welfare Committee.
- Company
- HK Inno.N releases its GERD drug K-CAB in Singapore
- by Chon, Seung-Hyun Sep 05, 2023 05:40am
- Professor Prakash Gyawali (Department of Gastroenterology at Barnes-Jewish Hospital, Washington University Hospital) is giving a lecture at the K-CAB Launch Symposium in Singapore On the 4th, HK Inno.N announced that it had officially released its novel gastroesophageal reflux disease (GERD) treatment K-CAB in Singapore. HK Inno.N held a symposium to celebrate K-CAB’s launch at the Conrad Centennial Singapore Hotel on August 31st. K-CAB was approved in February in Singapore under the same brand name, K-CAB. HK Inno.N will export the finished product to its local partner, United Italian Trading Corporation (UITC), which will be in charge of local sales and marketing of K-CAB in Singapore. The symposium, which was held for gastroenterologists in Singapore, was hosted by UITC. At the symposium, Professor Prakash Gyawali (Department of Gastroenterology at Barnes-Jewish Hospital, Washington University Hospital) and Professor Hwoon-Yong Jung (Department of Gastroenterology at Asan Medical Center) shared the latest knowledge in using K-CAB. During his presentation, Professor Gyawali focused on the superiority and safety of K-CAB, emphasizing the drug’s rapid onset of action and safety in terms of hepatotoxicity over other P-CAB class drugs. Professor Jung shared his prescription experience with K-CAB in Korea. Professor Jung said, “K-CAB had provided a better treatment option for GERD patients in Korea.” K-CAB has been exported as a technology or finished product to 35 countries overseas. Among them, the drug has been launched locally in China, Mongolia, the Philippines, Mexico, Indonesia, and Singapore. Also, the company is preparing to launch K-CAB in Peru after receiving approval in July. Dal-won Kwak, CEO of HK Inno.N, said, “Singapore’s pharmaceutical market stands out among Southeast Asian countries, as it has been showing 11% YoY growth for the past 3 years. We will continue to work closely with our local partners to ensure the successful approval and launch of K-CAB overseas. K-CAB, which was released in March 2019, is a new drug for gastroesophageal reflux disease (GERD) in the P-CAB (potassium-competitive acid blocker) class. It has a new mechanism of action that inhibits gastric acid secretion by competitively binding to the proton pump and potassium ion located in the final stage of acid secretion. Its sales exceeded KRW 100 billion in prescriptions in its 3rd year of release in 2021 and recorded sales in the KRW 100 billion range for 2 consecutive years thereafter. Also, K-CAB posted prescriptions amounting to KRW 74.1 billion in the H1 this year, heralding a record that exceeds KRW 100 billion for three consecutive years.
- Policy
- Drug crime regulation,
- by Lee, Jeong-Hwan Sep 05, 2023 05:40am
- It is expected that a bill that would impose an obligation on doctors and pharmacists who prescribe and dispense drugs with a risk of misuse, such as narcotics, to check medication history through the Drug Safety Information System (DUR) will quickly pass the National Assembly. This is because a large number of drug-related crimes have occurred, such as the so-called 'Rolls Royce Man on Drug Suspicion' incident, and social consensus on the need for stronger regulations has grown, and the Yoon Seok-yeol government has also announced mandatory DUR confirmation of medication history as a measure to strengthen surveillance of medical drugs. On the 4th, Jeon Hye-sook, an official from the Democratic Party of Korea's office, explained, "We have secured a consensus not only on the government but also on the ruling and opposition parties on the need to make it mandatory to check the medication history of patients who prescribed and dispensed narcotics through DUR." The amendment to the Medical Service Act and the Pharmaceutical Affairs Act, proposed this time by Rep. Jeon Hye-sook, are a method of establishing new regulations on medicine and pharmacists in the 'confirmation of drug information' provision commonly stipulated in both laws. Specifically, the 'confirmation of drug information' clause stipulated in Article 18-2 of the Medical Service Act and Article 23-2 of the Pharmaceutical Affairs Act will be revised. Rep. Jeon Hye-sook's bill stipulates that in order to ensure the safe use of medicines, the Minister of Health and Welfare or the Minister of Food and Drug Safety must check whether the same ingredients have been administered in the past when prescribing, directly dispensing, or dispensing medicines that are recognized as having a risk of abuse, such as narcotics. In addition, DUR was proposed as a method for doctors, dentists, and pharmacists to check a patient's medication history for the same narcotic ingredient, and a fine of up to 1 million won could be imposed if the verification obligation was not followed. The Yoon Seok-yeol government declared war on drugs last April and announced comprehensive government-wide measures. At that time, as the Gangnam Academy District drug drink incident and famous celebrities' drug use crimes such as propofol and methamphetamine continued to occur, the Office for Government Policy Coordination announced that it would be mandatory to check prescription drug history using DUR, starting with drugs with a high risk of abuse such as fentanyl. With administration consistent with the purpose of the bill proposed by former lawmakers, an environment has been created in which the speed of processing can be accelerated when the bill is later reviewed by the National Assembly. There is a possibility that the medical community will oppose legislation mandating drug use history DUR. In the past, medical and hospital groups strongly opposed the amendments to the Medical Service and Pharmaceutical Affairs Act in the 20th National Assembly, which mandated the use of DUR when prescribing and dispensing medicines and imposed fines on violators. At the time, the medical and hospital communities considered the fact that punitive regulations were created without support measures such as fees or compensation for medical institutions, that doctors' judgments regarding drug prescriptions and dispensing could be excessively restricted, and that there were limits to clinical usefulness. rebelled against. The Ministry of Health and Welfare, the responsible ministry, and pharmacists' organizations supported the bill to strengthen drug safety by increasing DUR utilization. Rep. Jeon Hye-sook, who proposed the bill, plans to speed up the review of the bill by putting legislative feasibility first in order to prevent drug crimes from becoming increasingly rampant. She plans to push for legislation mandating the use of DUR when prescribing and dispensing non-reimbursed high-risk drugs and narcotic psychotropic drugs, following legislation mandating DUR confirmation of narcotic medication history.
- Policy
- Why many choline alfoscerates accepted price cuts
- by Lee, Tak-Sun Sep 05, 2023 05:39am
- Pic Chongkundang Gliatirin Soft Cap (left) and Gliatamin(right), leading choline alfoscerate drugs Companies are reluctant to self-manufacture their brain function enhancer choline alfoscerates despite price cuts. Only 20% of the companies decided to protect their drug price by switching to self-manufacture, and the prices of the others that opted to continue manufacturing through contract manufacture organizations (CMOs) were cut. This fact was evident in the insurance price ceiling reevaluation results announced by the Ministry of Health and Welfare on the 1st. Among the 51 choline alfoscerate 0.4g capsule formulations, 40 of them received price cuts of up to 15% of the highest price (KRW 445/capsule). 11 products have maintained the original drug price, and 10 of them have maintained their drug prices by conducting self-bioequivalence tests of their self-manufactured (imported) products. The products that maintained their price are ▲Chong Kun Dang Pharmaceutical’s ' Chongkundang Gliatirin Soft Cap.’▲Daewoong Bio’s 'Gliatamin Soft Cap. ' ▲Korea United Pharm 'Glicetil Soft Cap.' ▲GuJu Pharma ' Cereforin Soft Cap.' ▲Cosmax Pharma 'Choline Max Soft Cap. 400mg' ▲Mothers Pharm 'Memoem Soft Cap.' ▲Korea Prime Pharm 'Gria Soft Cap.' ▲Hanmi Pharm’s ' Cholinate Soft Cap. 400mg' ▲Su-Heung’s 'Alfogreen Soft Cap.' ▲Kukje Pharm ' Cholencina Soft Cap. ' A majority of products gave up protecting their drug prices with self-bioequivalence tests due to high investment risk. In 2020, the government made the decision to reimburse choline alfoscerate preparations only for dementia and apply selective reimbursement and cover only 80% of the cost for its main indication, mild cognitive impairment. Also, starting in 2021, clinical re-evaluation is underway to verify the substance’s efficacy for dementia and mild cognitive impairment. If the clinical trials show bad results, their indication may be reduced or deleted. This is why the analysis is that companies have been passive in maintaining their drug price by conducting self-bioequivalence tests. Even products with annual outpatient prescriptions exceeding KRW 10 billion did not defend their drug prices. Based on UBIST, the capsule formulations that posted sales of over KRW 10 billion, such as Daewon Pharmaceutical's Alfocholine (KRW 21 billion), Arlico Pharmaceutical's Choliatin (KRW 18 billion), Yuhan Corp’s Alfoatilin (KRW 17.5 billion), Jeil Pharmaceutical's Glitin (KRW 16 billion), and HLB Pharmaceutical's Glitia (KRW 12.9 billion) and Hutex’s Silvercerin Tab. (KRW 11.7 billion), maintained consignment production, and the insurance price ceiling of the drugs fell to KRW 445. Some have also pointed out that companies decided to not defend drug prices to pursue a low-price strategy as competition is intensifying. Dongkoo Bio Pharm’s Glifos Soft Cap. already lowered its price to KRW 445 in September last year. Nevertheless, UBIST showed Glifos’s sales grew 36% from the previous year to KRW 14.8 billion in outpatient prescriptions last year. An industry official said, “Choline alfoscerate has significant product risk due to clinical reevaluations. Also, we did not take any action to defend drug price because we are pursuing a low-price strategy."
- Company
- Humira market biosimilar share
- by Kim, Jin-Gu Sep 04, 2023 05:04am
- Two years have passed since the biosimilar of the autoimmune disease treatment Humira was launched in the domestic market, and its share in the adalimumab market was found to be around 14%. According to IQVIA, a pharmaceutical market research firm, on the 2nd, the market for 'Adalimumab' ingredients in the first half of this year was 50.1 billion won, a 9.9% increase from 45.6 billion won in the first half of last year. Adalimumab is a TNF-alpha inhibitor that treats autoimmune diseases such as rheumatoid arthritis and psoriasis. AbbVie's Humira is the original drug. It was well known as the product with the highest sales in the world until last year. In Korea, sales were 104 billion won in 2020, 92.4 billion won in 2021, and 93.8 billion won in 2022. In particular, the decline in sales in 2021 compared to 2020 is large because the drug price was reduced by 30% with the release of Humira biosimilar. Samsung Bioepis launched Adalloce as a Humira biosimilar in the third quarter of 2021. Then, in the third quarter of last year, Celltrion released Yuflyma. Although two years have passed since launch, the market share of the two biosimilars appears to be only around 14%. This is in contrast to the Avastin biosimilar, which increased its market share in the Bevacizumab market to more than 35% within two years of its launch. Samsung Bioepis Adalloce recorded sales of 5.8 billion won in the first half of last year, more than doubling from KRW 2.7 billion in the same period last year. Cumulative sales exceeded 10 billion won in the first quarter of this year and accumulated 14.5 billion won by the second quarter. Celltrion Yuflyma has been gradually expanding its influence, posting cumulative sales of 1.3 billion won since its launch in the third quarter of last year. Sales in the first half of this year were 800 million won. In addition, LG Chem has announced the release of a Humira biosimilar. LG Chem applied for product approval for Humira biosimilar ‘LBAL’ at the end of last year. LG Chem confirmed the equivalence and safety of LBAL and the original drug Humira in phase 3 clinical trials conducted in Korea and Japan with its Japanese partner Mochida Pharmaceutical, respectively. In the safety category, the incidence of adverse events (AEs) was similar in the LBAL group and the Humira group. In the case of the original Humira, quarterly sales are maintained at around 22 billion won, except for a 30% price cut following the release of biosimilars. In fact, Humira sales in the first half of last year amounted to 43.4 billion won, a 1.4% increase from 42.9 billion won in the same period last year. Analysis suggests that the company is successfully protecting sales overall despite the launch of biosimilars.
- Company
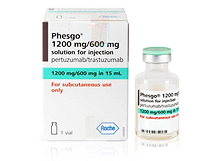
- Will Phesgo be listed with pricing premiums as a biobetter?
- by Eo, Yun-Ho Sep 04, 2023 05:04am
- Whether another biobetter after Nexviazyme will be receiving premium pricing in Korea is gaining attention. According to industry sources on the 30th, Roche Korea’s subcutaneous fixed-dose combination injection Phesgo (pertuzumab, trastuzumab) that combined ‘Perjeta’ and ‘Herceptin’ has passed the Health Insurance Review and Assessment Service’s Cancer Disease Deliberation committee review. Therefore, after undergoing the Drug Reimbursement Evaluation Committee review, Roche will sign agreements with the National Health Insurance Service regarding the supply and quality control obligations for Phesgo. If successfully listed, Phesgo will become the first anticancer drug and the second drug to benefit from the biobetter preferential treatment plan. In 2016, the government announced a plan to provide preferential pricing for biosimilars and biobetters, which are improved versions of already approved biopharmaceuticals, that have contributed to the improvement of Korea’s healthcare. In the case of Nexviazyme, In consideration of how biobetters are more difficult to develop compared to incrementally modified drugs (chemical drugs), the overall price of Nexviazyme was set at the 100-120% range of the original drug. However, since the implementation of the system, no drug has benefitted until now, and Nexviazyme became the first drug to benefit from the 1st. Phesgo was recognized for its innovation in improving patient convenience and reducing treatment time by changing the IV-injected Herceptin and Perjeta into a fixed-dose subcutaneous injection and was named the first biobetter approved for cancer in Korea. Metastatic HER2-positive breast cancer patients who had received maintenance therapy with IV Herceptin and Perjeta injections every three weeks may reduce their administration and monitoring time by 90% from 270 minutes (90min+180min) to 20 minutes (5min+15min) when switching to Phesgo. Also, as Phesgo is a subcutaneous formulation injected in the thigh rather than into the veins, it can reduce blood vessel and nerve damage that can be caused by repeated intravenous injections. The NCCN guidelines state that Phesgo can be used in the place of Perjeta and Herceptin, In fact, in the UK, 90% of patients treated with Herceptin and Perjeta switched to Phesgo within a year after its launch. Therefore. If listed, a significant number of patients receiving Herceptin-Perjeta treatment are expected to switch to Phesgo as well.
- Policy
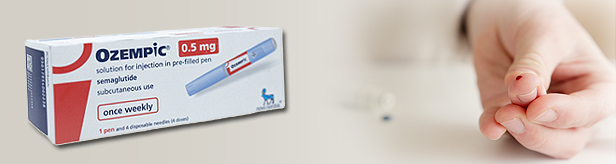
- New GLP-1 RA stops reimb discussions in KOR
- by Lee, Tak-Sun Sep 04, 2023 05:04am
- Novo Nordisk The debut of a new GLP-1 analog used as an adjuvant to dietary and exercise therapy in diabetes patients has been postponed in Korea. This comes as a disappointment as only one single-agent drug is currently reimbursed in Korea, and the high global demand for the drugs has rendered domestic supply short. According to the Health Insurance Review and Assessment Service and the industry on the 1st, discussions for the reimbursement of Novo Nordisk’s single agent GLP-1 receptor agonist ‘Ozempic Pre-Filled Pen' have come to a stop. This drug was recognized as appropriate for reimbursement by the Drug Reimbursement Evaluation Committee in February under the condition that the company accepts a price below the evaluated amount. Afterward, the pharmaceutical company accepted the evaluated amount and began drug pricing negotiations with the National Health Insurance Service. However, the company withdrew its The speculation is that the excess demand in the global market rendered it difficult for the company to supply the drug to Korea as well, for at least one year. Currently, the only single-agent GLP-1 receptor agonist available with reimbursement in Korea is Dulaglutide (Trulicity). Exenatide (Bydureon, AstraZeneca), which had received new reimbursement standards, had withdrawn its approval in September 2021. Another same-class drug, LyxumiaR had also withdrawn its approval in 2020. All of the companies gave up selling their drugs in the Korean market after losing to the long-acting once-weekly Trulicity. Since its release in May 2016, Trulicity has continued to its sole lead in the domestic market. Based on IQVIA, Trulicity recorded sales of KRW 59.4 billion last year. As another long-acting once-weekly treatment, Ozempic was expected to serve as a rival to Trulicity. In the global market, Ozempic’s sales have already surpassed that of Trulicity. However, its unstable supply due to global demand hindered its domestic launch. Ozempic is listed in the US, Japan, Italy, France, Switzerland, and the UK among the A7 countries. The Korean Diabetes Association and the Korean Endocrine Society had recommended that it would be appropriate to reimburse Ozempic as a long-acting GLP-1 receptor agonist same as Trulicity, as a comparative study between the two same-class drugs has also been conducted. GLP-1 is a hormone that regulates glucose and appetite and has various effects on the cardiovascular system. Its effect on glucose and appetite is achieved through GLP-1 receptors in the pancreas and brain, and GLP-1 analog drugs selectively bind and activate these GLP-1 receptors.
- Opinion
- [Reporter’s View] Disclose PVA results in advance as well
- by Lee, Tak-Sun Sep 04, 2023 05:04am
- The government announced the 7,000 drug items whose insurance price ceiling will be lowered according to the reevaluations that were conducted in advance. This preemptive measure was made out of concern over the large settlement of price differences and returns that may occur with the price adjustment. The product list and upper limit price were released on the 23rd of last month and were publicly notified on the 1st. The price adjustment will be applied in the field from the 5th. The public health authorities accepted the opinion of the Korea Pharmaceutical Association and others who requested sufficient time to prepare for returns and settlement of differences before the price adjustments. However, there remains some to be desired. In addition to those that were adjusted post-reevaluations, the insurance price ceiling of 134 other items had also been adjusted through the PVA (price-volume agreement) system. The adjusted price for the PVA price cuts will also become effective as of the 5th. Among the PVA price cut items, the prices of some have been further reduced due to the reassessment of the price ceiling, so the implementation of the PVA price adjustments was changed to match the price ceiling reevaluation schedule to prevent confusion in the field and reduce administrative costs. 18 items have undergone both PVA and price ceiling reevaluations. If the PVA price cuts were first implemented on the 1st of this month as scheduled, then the price ceiling reevaluation adjustments implemented on the 5th, these drugs would have had to change their price twice in one month. In this sense, setting the same implementation date for the two was reasonable and correct. However, it would have been better if the government had disclosed the PVA-adjusted drug items in advance as well. The price ceiling reevaluation results were released on the 23rd of last month, but the PVA list was released only on the 31st, after completing the Health Insurance Policy Deliberative Committee (HIPDC) review. Wholesalers and pharmacies have expressed the opinion that more preparations were needed for items on the PVA list, due to the high volume of returns necessary for some of the frequently used items. However, unlike the price ceiling reevaluations, the adjusted insurance prices were not announced in advance for the PVA items, increasing inconvenience in the field. Why the PVA list was not disclosed in advance, unlike the price ceiling reevaluation results, remains a question, as the effective date for the price ceiling adjustment for the two drugs was set at the same date, on the 5th. It is interpreted this may have been in line with the principle of non-disclosure before HIPDC review, but it is regrettable that the government was unable to show some flexibility, given that the price ceiling reevaluation results that were disclosed were also yet to receive HIPDC review at the time of disclosure. As a result, while 14 days were given to prepare for the return of items that underwent price ceiling reevaluations, only 6 days were given to prepare for the return of the PVA items. Another problem is that the prices of some items that are on the price ceiling reevaluation list will further be reduced due to PVA. If companies had prepared to settle their accounts based on the prices indicated in the price ceiling reevaluation list that was disclosed on the 23rd, they would have had to make re-readjustments to their accounts. In this sense, the imperfect data that was disclosed to prevent on-site confusion has burdened the site. This too could have been prevented if the PVA results had been transparently disclosed on the 23rd. The government's pre-release of the list of drug price cuts and postponement of the PVA implementation date are commendable in that they considered the confusion that will be caused by returns and balance settlements after the price adjustments. However, the measure should have been more well thought out. It would be best if the Ministry of Health and Welfare, which is in charge of the price ceiling reevaluations and PVA, put some more considerations into its measures.
- Company
- Can Koselugo pass the Pharmaceutical Evaluation Committee?
- by Eo, Yun-Ho Sep 04, 2023 05:04am
- Koselugo, a new drug for pediatric neurofibroma, is once again awaiting discussion for listing on insurance benefits. Attention is focused on whether AstraZeneca Korea's neurofibromatosis new drug Koselugo, which was decided for re-discussion at HIRA last month, will be presented to the committee on the 7th. Koselugo failed to reach an agreement at the committee last month even though the pharmaceutical company submitted supplementary data and a risk-sharing plan. This disease begins in childhood with milk-coffee spots measuring 1 to 3 cm. Afterward, they experience symptoms such as optic nerve glioma (brain tumor) around the age of 6 and scoliosis between the ages of 6 and 10. In adults, Lisch nodules, which are hamartomas that occur in the iris, are most commonly found. The possible part can be removed surgically or treated with chemotherapy or radiation. However, even after surgery, most cases recur, and most of them are major surgeries, putting a significant burden on both the medical staff and patients. In particular, recurrences are frequent in pediatric patients, so even after multiple surgeries, they have to take painkillers and often suffer from speech and motor difficulties. Koselugo is a treatment jointly developed by AstraZeneca and MSD. It inhibits the growth of cell lines by blocking MEK activity. In the SPRINT phase 2 clinical trial, which served as the basis for approval, Koselugo achieved ORR, the primary endpoint, by reducing tumor size by more than 20% in 68% of administered patients. Additionally, 82% of patients who showed a partial response maintained the response for over 12 months. Among patients who did not receive treatment, half experienced disease progression after 1.5 years, but only about 15% of patients who used Koselugo experienced disease progression even after 3 years.