- LOGIN
- MemberShip
- 2026-04-10 17:06:14
- Company
- Possibility of passing the drug price reduction Act
- by Kim, Jin-Gu Mar 20, 2023 05:51am
- A sense of crisis in the biopharmaceutical industry is rising as the possibility of passing the 'drug price reduction/refund bill' in the plenary session of the National Assembly is increasing. The pharmaceutical industry is concerned that the amendment will infringe on the right to request a trial as stipulated in the Constitution, and furthermore, it will damage the domestic pharmaceutical and bio-industry as a whole. According to the pharmaceutical industry on the 16th, the revision of the National Health Insurance Act, the so-called Drug Price Reduction and Refund Act, proposed by Rep. Kim Won-i and Nam In-soon, respectively, will be decided at the National Assembly plenary session this month at the earliest. According to this amendment, if a pharmaceutical company loses a lawsuit on drug price cuts, it must discharge the health insurance finances invested during the drug price cut suspension period. In the opposite case, the amended bill also contains content that allows the NHIS to refund the damages incurred by the pharmaceutical company during the course of the lawsuit if the pharmaceutical company wins the primary case. However, in the pharmaceutical industry, the position is that in the case of 'refund', it does not fall under the requirements for citation for suspension of execution. In the current legal system, suspension of execution is cited when there is a 'concern about serious and irreparable damage'. However, in the case of a refund, it is argued that these requirements are not met. As a result, concerns are raised that the enforcement of the law will be biased toward the recovery among refunds and refunds, which will violate the right to request a trial specified in the Constitution and worsen the remedy of rights. There are concerns that companies' attempts to suspend the execution of the government's drug price cuts will significantly shrink. In the pharmaceutical industry, it is the position that the economic gains and losses caused by the difference between the decision to suspend execution and the judgment on the merits should be remedied according to the existing procedures, such as claims for damages between companies or parties. It is also criticized that it is not right in the legal system for the state to consider unfair gains and return them after the fact, and that excessive infringement of property rights is unconstitutional. Furthermore, the pharmaceutical industry is concerned that if this amendment is passed, it will deal a blow to the domestic pharmaceutical bio-industry as a whole. In fact, in past cases of suspension of execution citations, three-fourths of the total number of citations are for domestic pharmaceutical companies. The expected surcharge upon redemption of these is estimated at 490 billion won. This is eight times higher than multinational pharmaceutical companies' 59 billion won. In particular, the pharmaceutical industry is criticizing that legal disputes over drug price reduction, which is a legitimate right of companies, will shrink in a situation where government re-evaluation mechanisms such as re-evaluation of already-listed drugs, re-evaluation of benefit adequacy, and re-evaluation of overseas drug prices are expected to continue in the future. It is expected that the Drug Price Reduction Act will discourage domestic pharmaceutical companies from challenging patents and thereby worsen the positive function of reducing health insurance finances. This is because if the original company finally wins the lawsuit and the NHIS refunds the pharmaceutical company the loss caused by the drug price cut, the NHIS can claim the right of indemnity from the generic company that participated in the patent lawsuit. The pharmaceutical industry was concerned that the amendment would undermine generic companies' willingness to challenge patents and hinder active patent challenges. As a result, there are concerns that the opportunity for financial savings due to the release of generics will be lost.
- Company
- Generics for Visanne grew significantly in Bayer's opening
- by Whang, byung-woo Mar 17, 2023 05:46am
- As the generic market for Visanne, Bayer's endometriosis treatment, is growing rapidly, the status of the original drug is being threatened. According to the pharmaceutical industry, as the number of patients with endometriosis increased significantly, the treatment market was also found to be growing significantly. Looking at the health insurance treatment status of 'endometriosis (N80)' from 2016 to 2020 announced by the NHIS, the number of endometriosis patients increased by 48.2% from 104,689 in 2016 to 155,183 in 2020. Due to this influence, medical expenses also increased by 79.6% from 56.6 billion won in 2016 to 101.6 billion won in 2020, and outpatient medical expenses surged 147.7% from 16.4 billion won to 40.6 billion won. Visanne's sales continued to rise during the same period as the number of patients increased. According to UBIST, a drug research institute, Visanne's sales recorded a growth of ▲8.6 billion won in 2017 and ▲10.5 billion won in 2018. Afterward, sales decreased to 7.6 billion won in 2019 when insurance drug prices decreased (53,980 won → 37,786 won), but sales increased again to 7.8 billion won in 2020, 9.5 billion won in 2021, and 9.9 billion won in 2022. Considering the fact that there was another drug price cut to 28,906 won in 2021, the actual amount of prescriptions compared to sales is expected to increase further. It is analyzed that Visanne's growth was largely driven by two factors. The first factor is that since December 2018, even patients diagnosed radiologically using ultrasound or MRI can use Bizan, which has improved the patient discovery and prescription environment. Experts believe that the fact that ultrasound of the female genital organs, including the uterus, was covered in February 2020 as part of strengthening insurance coverage, may have had an impact on increasing patient accessibility. In fact, according to the NHIS data, the number of patients with endometriosis in 2019-2020 stood out more than in other years. It increased by 12% from 136,144 in 2019 to 155,183 in 2020. Compared to the annual increase of 7-9%, the rate of increase is greater. As the number of endometriosis patients increases, the growth rate of generic products in addition to the original Bizan is also increasing significantly. According to Ubist, the sales growth of the Bizan generic product line was minimal, with sales of ▲900 million won in 2019 and ▲1.2 billion won in 2021. This is a figure that has grown by about 8.4% from 16.6% in 2021 to 25% in 2022 in terms of sales compared to the total market size. Bayer has no choice but to think about various strategies to continue Bizan's growth. Basically, in this situation, the first thing multinational pharmaceutical companies emphasize is the long-term effect and safety of the original. Bayer announced that Bizan reduced EAPP and improved HRQoL in the long term through the final analysis results of 'ENVISIOeN', a real-world study that evaluated the long-term efficacy and safety of Bizan in 6 Asian countries for 24 months in March last year. did. Along with this, Bayer's more fundamental response strategy is to expand its treatment of endometriosis rather than playing a game of chicken with generics in the market. In December 2018, it was possible to diagnose endometriosis with ultrasound, but the proportion of clinicians is still relatively low when examining the usage performance by a nursing institution with Visanne and Dienogest. Bayer's strategy also starts from this situation. Until now, endometriosis was recognized as a disease that was treated in general hospitals, but the plan is to focus on publicizing it as the paradigm is changing. A Bayer official said, “The biggest task is to publicize endometriosis as a disease that can be treated in clinics. Now, we are focusing on publicizing it based on a lot of evidence.” As we are at the stage of treatment, we are considering practical measures through a paradigm shift in treatment and RWE."
- Company
- Sales in the Dutasteride market are strong
- by Kim, Jin-Gu Mar 17, 2023 05:46am
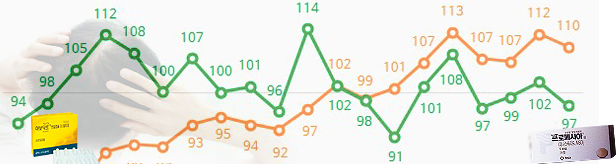
- Avodart and Propecia quarterly sales (units, data IQVIA) The original drug, GSK Avodart, was the first in 2021 to go beyond Propecia (Finasteride), leading to the market for two consecutive years until last year. In the case of generic, Dutasteride grows steeply and pursues the Finesteride quickly. In the pharmaceutical industry, the new formulation product is cited as a variable in the market. Boryeong's newly -made FINASTERIDE ingredient has been released, and Chong Kun Dang is developing a product of an injection formulation. ◆ Avodart's sales last year sales of 43.6 billion won VS Propecia's sales of 39.6 billion won According to IQVIA, a pharmaceutical market research firm on the 15th, GSK Avodart's sales last year were 43.6 billion won. In 2021, the company increased by 4% from 41.9 billion won, changing the highest sales record. If the scope is expanded to the last four years, sales growth will be even worse. Avodart's sales, which amounted to 31.1 billion won in 2018, increased by 40% in four years. In particular, in 2021, the company surpassed the existing market in Korea. Propecia, the origin of hair loss treatment, has been steadily declining since 2019. Propecia's sales amounted to 39.6 billion won last year. In 2019, sales of 41.6 billion won were lowered to less than 40 billion won in 2021, and last year, it decreased even more. In the pharmaceutical industry, price competitiveness is cited as Avodart's rapid growth. AVODART is currently being supplied to 700 won per 1,700 won per 0.5mg product. Avodart has lowered the price from 1300 won to 920 won as the patent expired in 2016. In 2017, additional cuts to 700 won were lowered to half compared to Propecia. ◆ Dutasteride generic sales rising Dutasteride products also increased significantly. Hyundai Pharm's Damodad's sales, which amounted to 5.9 billion won in 2021, increased 26% to 7.5 billion won last year. Until 2019, annual sales amounted to only 900 million won, but more than eight times in three years. Hanall Biopharma Pharma ADAMO also increased sales by 62% from 1.8 billion won to 3.1 billion won in a year. In addition, sales increased by more than 10% in one year, including Huttex Pharmaceuticals Korea, Daewoong Bio DAEWOONG BIO DUTASTERIDE, DUTALID, and Dutaride Soft Cap. In the case of Finasteride, the market size is still greater than Dutasteride, but the growth trend has slowed. Momopecia increased 13% from 5.7 billion won in 2021 to 6.5 billion last year. On the other hand, Genu One Science MYPECIA decreased by 16% from 5 billion won to 4.1 billion won during the same period, while JW SHINYAK MONAD decreased by 25% from 5.3 billion won to 4 billion won. The sales of three of the six products, which recorded more than 3 billion won last year, fell compared to the previous year.
- Policy
- Marketing authorization imminent for Obizur in Korea
- by Lee, Hye-Kyung Mar 17, 2023 05:46am
- Marketing authorization for Takeda Pharmaceuticals Korea’s ‘Obizur Inj (susoctocog alfa)’ is imminent in Korea. Obizur Inj is a treatment for bleeding episodes in adults with acquired hemophilia A. The drug has been used as a treatment for hemophilia A in Korea after receiving an orphan drug designation in July 2021. According to the industry on the 16th, the Ministry of Food and Drug Safety recently completed the safety and efficacy review for Obizur. If the MFDS completed the safety and efficacy review without issues, the drug’s marketing authorization is expected to be underway soon. Hemophilia is a congenital bleeding disorder caused by a congenital deficiency of a blood clotting factor and is estimated to have an incidence of 1 per 10,000 births. Depending on the deficient blood clotting factor, hemophilia is divided into two types – hemophilia A and hemophilia B – and hemophilia A accounts for 80% of all hemophilia and hemophilia B for the other 20%. Unlike general hemophilia, acquired hemophilia A is a very rare condition caused by the development of autoantibodies directed against factor VIII, which leads to bleeding episodes like those experienced by hemophilia patients. According to domestic research, 55 patients are reported to have acquired hemophilia in Korea, and the prevalence rate is 0.2-1.48 per 1,000,000 people. Unlike congenital hemophilia, which almost always occurs in boys, acquired hemophilia mostly affects men and women over the age of 65. Orphan drugs are treatments used for diseases that affect 20,000 or fewer patients (prevalence population) in Korea, and are used for diseases for which no appropriate treatment method or drug has been developed, or drugs whose safety or efficacy have been significantly improved compared to existing alternatives.
- Company
- Enhertu's petition subcommittee is announced
- by Eo, Yun-Ho Mar 17, 2023 05:46am
- The 'answer' to the national petition urging insurance coverage for the next-generation ADC anti-cancer drug Enhertu is expected to come out soon. According to the related industry, Daiichi Sankyo Korea and AstraZeneca Korea's HER2-positive breast cancer treatment, Antibody-drug conjugate (ADC) Enhertu, will be submitted to the Petition Review Subcommittee next week. As a result, attention is paid to how it will affect the Enhertu benefit listing process. The drug was referred to the Health and Welfare Committee of the National Assembly last month after a petition urging health insurance approval at the beginning of this year gained the consent of 50,000 people. Enhertu, based on the DESTINY-Breast01 and DESTINY-Gastric01 clinical studies from the Ministry of Food and Drug Safety in September of last year, Enhertu is ▲unresectable or metastatic HER2-positive breast cancer who have previously received two or more anti-HER2-based therapies and ▲previously anti-HER2 anti-HER2 approved for the treatment of locally advanced or metastatic HER2-positive gastric or gastroesophageal junction adenocarcinoma who have received two or more therapies, including treatment. Also, in December, based on the DESTINY-Breast03 clinical trial, it received approval for an expanded indication for the treatment of patients with unresectable or metastatic HER2-positive breast cancer who had previously received one or more anti-HER2-based therapies. Enhertu is an antibody-drug conjugate. The antibody-drug conjugate uses the selectivity for the target and the killing activity of the drug to selectively act only on cancer cells, thereby increasing the therapeutic effect and minimizing side effects. Ra Seon-young, a professor of oncology at Yonsei Cancer Hospital, said, "Enhertu is the first and only HER2-targeted therapy that has demonstrated a survival period of more than one year as a treatment for advanced gastric cancer after treatment with Trastuzumab. "Considering the small number of patients, we hope that the reimbursement will be applied as soon as possible," she said. In the Enhertu DESTINY-Breast03 study, a head-to-head treatment with T-DM1 showed a significant improvement in PFS in patients with unresectable or metastatic HER2-positive breast cancer who had previously received one or more anti-HER2 therapies. In the interim analysis updated in 2022, mPFS was 28.8 months in the Enhertu group, 22 months longer than 6.8 months in the T-DM1 group, and overall survival (OS), a major secondary endpoint, was higher in the Enhertu group than in the T-DM1 group It showed a statistically significant result that reduced the risk of death by 36% compared to Enhertu's DESTINY-Breast01 trial confirmed sustained antitumor effects in patients with unresectable or metastatic HER2-positive breast cancer who had previously received two or more anti-HER2 therapies including T-DM1, Trastuzumab, and Pertuzumab. As a result of the study, Enhertu showed a confirmed ORR of 60.9%) and mPFS of 16.4 months. The mDOR was 14.8 months, showing a sustained antitumor effect even in severely ill patients with a median number of previous anticancer drugs reaching 6 (range 2-27).
- Company
- MSD ‘Januvia’s NTTP impurity level is at low risk’
- by Jung, Sae-Im Mar 17, 2023 05:45am
- On the 16th, Regarding the issue of excess nitrosamine impurities detected in some Januvia 50mg products, MSD Korea said, “The company has detected impurities that exceed the acceptable limit in two 50mg packaged batches among all Januvia products that were imported to Korea until October 2022. As a precautionary measure, the company has decided to voluntarily recall these products, and the level of impurity detected in the batches poses a negligible risk to patient safety." According to MSD Korea, the company has been updating the Ministry of Food and Drug Safety on the company’s measures and plans for control since August last year when the company first became aware of possible detection of the nitrosamine carcinogen, 'Nitroso-STG-19 (NTTP),' in Januvia. Upon MFDS request, the company has recently conducted a full inspection of impurities on all distributable Januvia products among those imported to Korea by October last year. Results showed that Januvia 50mg products with batch numbers ▲U010253 ▲U012914 were detected to have excess nitrosamine impurities. MSD Korea explained, “The detected level of impurities slightly exceeds the temporary accepted interim limit (maximum 246.7 ng/day).” The company had decided to make voluntary recalls for the batches detected with excess impurities on the 15th. The detected batches were last supplied to the Korean market on November 1, 2021, and have a use-by date that expires in February 2024. MSD Korea added, “The number of products that were detected to have excess impurities account for 0.35% of all formulations of Januvia products that were distributed in the same period.” MSD Korea also estimated that most stock of drugs with the corresponding lot numbers would have been exhausted by now at pharmacies when considering the prescription rate, frequency of orders, and order volume of Januvia in Korea. NTTP was first found as an impurity last year. As a nitrosamine compound, it is naturally found in low levels in drinking water, pickled/grilled meats and fish, vegetables, and dairy products. It is also produced in the drug manufacturing process. In June last year, the European Medicines Agency (EMA) raised the possibility of NTTP detections and requested inspections for the substances ▲sitagliptin, ▲varenicline, ▲methylphenidate, ▲ rifampicin, ▲rasagiline, ▲amitriptyline, ▲nortriptyline, and ▲dabigatran. At the time, the impurity test on Januvia showed that detected levels of NTTP did not exceed the accepted level. Since then, MSD Korea has been additionally conducting NTTP tests on all samples of drugs that contain sitagliptin manufactured from July last year. In other words, drugs that were manufactured after July last year are only allowed to be released to the market if they pass testing for NTTP impurities, and therefore have no impurity issues. The company said, “We have been conducting additional quality control measures and supplying drugs that meet the temporarily accepted release standards, and are making rapid efforts to strengthen process control to further minimize the NTTP level so that we can meet the long-term intake standards.”
- Product
- It is difficult to solve the problem of expensive generics
- by Mar 16, 2023 05:46am
- The Pharmaceutical Association for a Healthy Society (CEO Hyung-geun Shin) submitted an opinion against the 'Partial Amendment to the National Health Insurance Act' proposed by Representative Kim Min-seok, saying that the problem of expensive generics cannot be solved with penalty-type rebates. On the 14th, the pharmaceutical association said, "The proposed amendment contains the contents of replacing existing drug price cuts and reimbursement suspension administrative measures with penalty surcharges, and applying the changed statute when the standard for pharmaceutical disposition is lighter. "It is a law to make fools of pharmaceutical companies that do not provide rebates, and it is self-evident that it will continue to increase the price of Korean generics, which are famous for being the most expensive among OECD countries," he said. They pointed out that practical measures have not been prepared for the rebate issue. In 2014, the National Assembly and civil society joined forces to enact the 'rebate two-out system' to punish illegal kickbacks. It is that they continue to claim that access is restricted. They said, "Although this claim threatens the basic principle of 'same ingredients can be substituted for preparation', which has been maintained by the NHIS for a long time, the NHIS accepts the pharmaceutical company's argument and imposes a penalty of 30-50% of the drugs subject to suspension of reimbursement. "Even in this situation, citing the patient's right to access medicines as a reason is no different from simply arguing for the rebate itself to be allowed," he pointed out. The Pharmaceutical Association said, "Korea is known to be the most expensive country for generic drugs among OECD countries through various studies, and accordingly, pharmaceutical companies provide various rebates to healthcare institutions to promote sales, and healthcare institutions pay more than to purchase cheaper drugs. In order to receive more money and valuables, prescriptions for more expensive drugs are induced, and the structure in which the proportion of Korean pharmaceutical expenditures continues to rise is repeating itself,” he emphasized. “Pharmaceutical rebates are not just punishments for unfair trade, but an act that threatens health insurance finances, patients’ wallets, and patients’ health,” he said. “The current drug pricing method, which guarantees high generic prices, must also be improved as soon as possible,” he urged. He also ordered the National Assembly to "strengthen the rebate punishment and eliminate rebates from medical sites, and this will protect the health of patients and the finances of the NHIS."
- Company
- Exclusive domestic sales of JW Shinyak, Galderma hair loss
- by Mar 16, 2023 05:45am
- Kim Yong-gwan, CEO of JW Shinyak (right), and Kim Yeon-hee, CEO of GaldermaJW Shinyak announced on the 15th that it has signed a domestic exclusive sales contract with Galderma for hair loss treatment Ell-cranell and nail athlete's foot treatment Loceryl nail lacquer. According to the contract, JW Shinyak will be in charge of domestic sales and marketing of the two products. Ell-cranell is an androgenetic alopecia treatment that can be used by both men and women. It minimizes hair loss by suppressing the production of dihydrotestosterone, which is the cause of hair loss, threefold. It is easy to apply to the scalp with an applicator once a day, increasing convenience. As a result of clinical trials on 51 female patients with androgenetic alopecia in Korea, the number of hair increased by 9.8% and the thickness of hair by 13.2% after 8 months of Ell-cranell application. Also, more than 80% of the clinical participants rated it as 'easy to apply and not sticky to the scalp and hair'. Loceryl nail lacquer is the first product of Galderma launched in Korea in 1999 and is the most-sold topical treatment for toenail fungus (onychomycosis) in the world. It is a manicure-type external application that is applied directly to the nails, and the antifungal effect is maintained for 7 to 14 days just by using it once or twice a week. It is quickly absorbed into the nail, is not easily erased by water or sweat, and forms a protective film on the surface to prevent infection. With this contract as an opportunity, JW Shinyak plans to further enhance its competitiveness in the domestic skin disease treatment market. Kim Yong-gwan, CEO of JW New Drug, said, "The introduction of Galderma products, which have proven their excellence in the global market, has allowed us to build a more diverse lineup along with existing self-produced drugs." will go," he said.
- InterView
- ‘Reimbursing Revlimid as maintenance therapy beneficial’
- by Eo, Yun-Ho Mar 16, 2023 05:45am
- Professor Hyeon-Seok Eom The multiple myeloma treatment ‘Revlimid’ has finally been listed for reimbursement after 4 long years of await as maintenance therapy, starting from the new year of 2023. Reimbursement of Revlimid as maintenance therapy had undergone various twists and turns in Korea. Since 2019, BMS Korea had actively sought to list the drug for reimbursement, but was unable to make progress. The agenda has been deliberated by the Cancer Disease Drug Committee during meetings that were held in September 2019, June 2020, then again in September last year. The last meeting gained attention due to its deliberation of the CAR-T therapy ‘Kymriah (tisagenlecleucel),’ but to no avail for Revlimid. After passing CDDC deliberations in June last year, Revlimid’s reimbursement was finally extended to cover its use as maintenance therapy after 4 years. That a drug can prevent or delay the recurrence of cancer is an extraordinary concept that all cancer survivors would opt for. Revlimid has presented such an option for the first time in the field of multiple myeloma, a type of blood cancer that has a recurrence rate of 70-80%. Dailpharm met with Hyeon-Seok Eom, Professor of Hemato-Oncology at the National Cancer Center to seek insight into the significance and value brought by Revlimid's reimbursement as maintenance therapy. -It took a long time for Revlimid to receive the reimbursement extensions. How do you believe the reimbursement extension will affect the field? When considering how research on Revlimid’s use as maintenance therapy started in the mid-2000s, quite some time had been taken for its reimbursement approval. After the 5-year, and 10-year study data were published, I remember demand started to rise for the reimbursement of the drug as maintenance therapy around 2015. Even patients recognized the need and filed petitions to the National Assembly. Despite such efforts, it took quite some time for Revlimid to receive reimbursement as maintenance therapy. Patients were unable to use the drug as maintenance therapy or had to pay the full non-insured price for such use. In fact, from the late 2000s to early 2010s, this difference in treatment options led to a difference in the 5-year survival rate of multiple myeloma patients in Korea and the U.S. This is an example of how access to drugs directly affected the survival rate of patients. In the same context, patients in Korea will enjoy an improvement in their survival rate with the reimbursement extension. Improvement in the patient's quality of life and survival rate is of the greatest significance in terms of treatment as well. -The reimbursement approval of RVd (lenalidomide+bortezomib+ dexamethasone) therapy last year has greatly changed the prescription pattern of HCPs in Korea. The reimbursement of the maintenance therapy will also bring much change in the prescription environment. I believe the reimbursement of Revlimid as maintenance therapy will change how HCPs progress with treatment in the first line as well as the second line for multiple myeloma. For example, a patient’s overall survival may improve further if he or she uses Revlimid as maintenance therapy after VRd (bortezomib+lenalidomide+dexamethasone) therapy. This is why many studies abroad investigated the use of Revlimid as maintenance therapy following VRd therapy. In this aspect, the reimbursement approval of Revlimid has great significance. -Ultimately, how well the disease can be cared for in the front line (as first-line therapy) seems to be key in managing multiple myeloma as well. That’s true. Despite the increasing diversity of treatment options available in the field, it is still most important to see a good prognosis in the earlier stages. Considering how about 30% of patients die while transitioning from first-line treatment to second-line treatment and the prognosis of patients generally worsens with later lines of treatment, it is very important to increase the time to recurrence and survival rate of patients by treating patients well in the earlier stages. Therefore, it is most important to improve the prevention of recurrence, PFS, and OS with first-line treatment after considering various treatment options. Many HCPs abroad use many drugs in the first line to prolong the treatment period as much as possible. -What improvements do you wish for in treating multiple myeloma? The reimbursement of Revlimid as maintenance therapy has improved the front-line treatment environment, therefore, we now need to focus on improving the second-line treatment environment. We need to use more diverse options to treat multiple myeloma in the second line as well. The survival period of the patients is greatly reduced when patients go through further lines of treatment. The PFS is only a few months, and even the OS does not exceed 1 year in later lines of treatment, so it is important to use drugs well in the earlier stages. Also, good drugs remain unreimbursed in Korea. It is a pity that these effective drugs cannot be used earlier due to environmental issues like lack of reimbursement and are therefore used in the later stages of treatment. As in the United States, we should allow the use of effective drugs in earlier lines of treatment, and discretion should be given to the doctors for the combined use of drugs with reimbursement. - Are there any drugs you are looking forward to in the field of multiple myeloma in the future? With treatments continuing to evolve, I expect new treatment methods like CAR-T therapies would also eventually be introduced to the field. Development of such treatments will significantly improve the OS and quality of life of patients in the earlier lines of treatment, in the first- or second-line. Currently, patients with multiple myeloma generally recieve chemotherapy and autologous hematopoietic stem cell transplantation. However, some patients may experience side effects such as hair loss due to strong drugs and the process itself is also cumbersome as it requires weekly hospitalization. I hope that positive changes would come to foster a better treatment environment for patients in the future.
- Company
- SPC Korea to exclusively distribute 2 new COPD drugs in KOR
- by Eo, Yun-Ho Mar 16, 2023 05:45am
- SPC Korea will now be in charge of the domestic supply of two new COPD drugs in Korea. The company announced it had signed an exclusive agreement for the sales and distribution of two Chronic Obstructive Pulmonary Disease (COPD) treatments with the multinational pharmaceutical company, Covis Pharma GmbH. Under the agreement, SPC Pharm has been exclusively selling and distributing Eklira (Aclidinium bromide)’ and ' Duaklir (aclidinium bromide/formoterol fumarate dihydrate) in Korea from March 1. Covis Pharma had previously acquired the global rights for Eklira and Duaklir from AstraZeneca. Upon signing the agreement, the exclusive distribution and sales rights for the drugs in Korea will be transferred to SPC Korea, and their license transfer process is currently underway. The two drugs are delivered via the Genuair device and used as maintenance treatment for patients with COPD. SPC Pharm plans to strengthen marketing for the products to increase the market share of these products in Korea's COPD treatment market. A company official said, “Through the agreement, we plan to strengthen the company's existing respiratory treatment portfolio and continuously introduce global new drugs to provide new treatment options in Korea ."