- LOGIN
- MemberShip
- 2026-04-03 10:38:09
- Company
- Novartis Korea holds Cosentyx symposium at KCR 2025
- by Whang, byung-woo May 28, 2025 05:54am
- Novartis Korea Novartis Korea announced on the 27th that it held a luncheon symposium at the 45th Korean Congress of Radiology Annual Scientific Meeting (KCR 2025) to highlight the clinical value of Cosentyx (secukinumab) as a treatment for ankylosing spondylitis. The luncheon symposium was moderated by Professor Yong-Beom Park of the Department of Rheumatology at Severance Hospital, with Dr. Lianne S. Gensler, Professor of Clinical Medicine at the University of California San Francisco (UCSF), serving as the presenter. Dr. Gensler presented on the topic “Secukinumab in Ankylosing Spondylitis: Improving Patient Outcomes Through IL-17 Inhibition,” and shared key clinical data and treatment insights from real-world practice. First, Dr. Gensler explained, “Cosentyx is a representative interleukin-17A inhibitor that has demonstrated high treatment response compared with placebo in patients with ankylosing spondylitis who have no prior treatment experience with biological agents, establishing itself as an important early treatment option.” In the MEASURE 2 study, a representative clinical trial evaluating the efficacy and safety profile of Cosentyx in ankylosing spondylitis, patients with no prior experience with biologic agents demonstrated a significantly higher ASAS20 response rate (Assessment of SpondylArthritis international Society 20% response criteria) at week 16 compared to the placebo group. Additionally, the 5-year long-term follow-up study of the same trial confirmed sustained symptom improvement, demonstrating the drug's long-term efficacy. On the same day, Dr. Gensler presented the results of the SURPASS study, which targeted patients with ankylosing spondylitis who had high CRP levels (C-reactive protein levels) of 0.5 mg/dL or higher and at least one syndesmophyte (bone-like bony growth originating inside a ligament) at baseline, indicating a high risk of disease progression. The primary endpoint of the study was the proportion of patients without radiographic progression at week 104, and there was no significant difference between treatment groups. Dr. Gensler said, “In the SURPASS study, patients with ankylosing spondylitis who had no prior experience with biologic therapy received either Cosentyx (150 mg, 300 mg) or adalimumab biosimilar 40 mg, and both treatment groups demonstrated high levels of disease control.” Dr. Gensler also presented real-world data from the FORSYA study, which examined differences in treatment maintenance rates based on the timing and sequence of Cosentyx administration in ankylosing spondylitis, showing that using Cosentyx as the first biologic agent resulted in higher 1-year treatment maintenance rates. Dr. Gensler emphasized, “These results are significant as using Cosentyx as early as possible may lead to more sustained treatment effects and improved patient adherence.” Professor Yong-Beom Park, who attended as the moderator at the luncheon symposium, said, “Ankylosing spondylitis is a condition where early diagnosis and treatment are crucial for symptom control and prevention of joint damage. Fortunately, effective treatment options have been developed, allowing us to anticipate better treatment outcomes for patients compared to the past. Since Cosentyx has established itself as a first-line biologic therapy for ankylosing spondylitis in Korea, and we have been able to recognize its clinical value on-site thereafter, it was meaningful to share the latest treatment insights on Cosentyx at today's symposium.”
- Company
- Will JAK inhibitors for inflammation expand mkt presence?
- by Moon, sung-ho May 28, 2025 05:54am
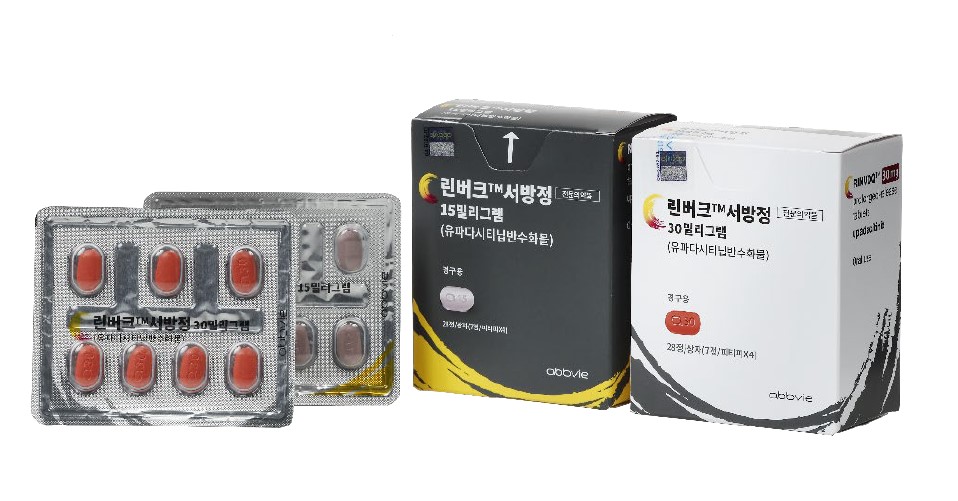
- It has been confirmed that Janus kinase (JAK) inhibitors are more effective at rapidly and powerfully controlling inflammatory responses in atopic dermatitis compared to biologics. Now that switching therapies between different drug classes is allowed, this finding is expected to serve as a key basis for drug selection in clinical practice. According to the pharmaceutical industry, on May 26, the Ministry of Health and Welfare (MOHW) revised reimbursement criteria as of March, allowing for the switching of therapies between JAK inhibitors and biologics for the treatment of atopic dermatitis. Subsequently, clinical settings will have to consider treatment strategies following reimbursement approval for switching between drug classes. Recently, the results of sub-analysis studies, Heads Up and Level Up clinical trials, were reported. The study involved a comparison between the JAK inhibitor Rinvoq (upadacitinib, AbbVie) and the biologic dupilumab. This research not only showed that Rinvoq rapidly and strongly suppresses Type 2 inflammatory responses, a core pathogenesis of atopic dermatitis, but also effectively controls other significant inflammatory responses related to atopic dermatitis, such as Type 1 and Type 17/22 responses. Specifically, in the sub-analysis of the Heads Up study, at week 2 of treatment, the gene expression patterns (transcriptomes) in the skin of the Rinvoq group were approximately 66.5% similar to those of normal skin. In contrast, dupilumab's transcriptome normalization was only 2.0% (P < 0.001). At week 16 of treatment, the level of transcriptome normalization was 104.4% for the Rinvoq group and 62.9% for the dupilumab group, with the Rinvoq group showing significantly higher efficacy (P
- Policy
- Expanded reimb for Jardiance's CKD indication imminent
- by Lee, Tak-Sun May 27, 2025 06:19am
- Jardiance Tab It is to be watched whether the SGLT-2 inhibitor Jardiance (empagliflozin, Boehringer Ingelheim) will be approved for expanded reimbursement to include chronic kidney disease (CKD) indication, in addition to diabetes and chronic heart failure indications. The evaluation by the Health Insurance Review & Assessment Service (HIRA) is expected to be nearing end following the reimbursement expansion filed in the first half of last year. According to industry sources on May 26, HIRA is reportedly reviewing expanded usage scope and pre-drug price reduction system for Jardiance's CKD indication. The pre-drug price reduction system for expanded usage scope drugs is designed to quickly enhance patient access to treatment by omitting the cost-effectiveness evaluation and applying a pre-reduction rate table, with a maximum 5% reduction in the ceiling cap, considering the estimated additional claim amounts due to the expanded reimbursement criteria. Once the pharmaceutical company submits financial impact analysis data and HIRA determines the pre-reduction rate through practical review, the Drug Reimbursement Evaluation Committee (DREC) will deliberate. If the pharmaceutical company accepts the deliberation results, the revised reimbursement criteria notification is completed after negotiation with the National Health Insurance Service (NHIS). The company applied to HIRA for reimbursement expansion for Jardiance's CKD indication in the first half of last year. Jardiance was the first SGLT-2 inhibitor to file. The approved indications for Jardiance 10mg tablets are: 1. Type 2 diabetes mellitus, 2. chronic heart failure, and 3. chronic kidney disease. Jardiance Tab, which were listed for reimbursement as a diabetes treatment in 2017, have also been reimbursed for chronic heart failure since February 2024. Since January, the reimbursement criteria have been expanded, allowing patients with heart failure with preserved ejection fraction (HFpEF) who have symptoms and signs of heart failure and a left ventricular ejection fraction exceeding 40% to receive national health insurance benefits. Currently, the only SGLT-2 drugs covered for diabetes and chronic heart failure patients, besides Jardiance, are Forxiga (dapagliflozin) and HK inno.N's DapaN Tab, which transferred Forxiga's indications. However, there is currently no drug reimbursable for CKD. If the reimbursement expansion procedure for Jardiance is completed, it is expected to be the only SGLT-2 drug with CKD reimbursement coverage. The efficacy of Jardiance has been demonstrated through clinical trials, showing a statistically significant 28% relative risk reduction in the progression of kidney disease or cardiovascular death compared to placebo. The competition in the market for SGLT-2 has been intensified due to the expiration of dapagliflozin patent in 2023 and the launch of generic drugs, Jardiance's expanded reimbursement scope to include CKD will give Jardiance a competitive advantage. Generic drugs are expected to launch following Jardiance's substance patent expiration in October. However, Jardiance's heart failure and kidney disease indications are expected to remain protected, so expanded reimbursement is anticipated to minimize the impact of generic entry. The pharmaceutical industry anticipates that the reimbursement expansion for Jardiance's CKD indication will be approved after July or by the end of the year.
- Company
- Will Imfinzi finally be reimbursed for biliary tract cancer?
- by Eo, Yun-Ho May 27, 2025 06:18am
- With the advent of an era in which a single drug is used for multiple indications, awareness is growing on the need to address the issue of non-reimbursed indications. In particular, in order to improve Korea’s rigid reimbursement evaluation system, which is regarded as the main cause of reimbursement delays, not only using the flexible application of ICER but also the weighted average price (blended pricing) method for each indication is being specifically discussed. The recent “Policy Debate on Addressing Inequality in Access to Innovative Drugs and Improving Regulatory Frameworks” also focused on the need for system reforms to enhance patient access and discussed the necessity of introducing the blended pricing method in depth. The blended pricing method calculates the average drug price by reflecting the value of each indication for multi-indication drugs and is considered an effective way to enhance patient access while efficiently managing health insurance finances. Italy, France, and Australia are already using this method to secure flexibility in reimbursing innovative drugs. In particular, IBP applies to risk-sharing agreements (RSAs) and is emerging as a realistic alternative due to its high feasibility and lower administrative costs. One example is the PD-L1 inhibitor Imfinzi (durvalumab). This drug was first listed in 2020 for the treatment of non-small cell lung cancer and is currently undergoing the reimbursement process for biliary tract cancer, a disease with limited treatment options. In the poor prognosis setting of biliary tract cancer, where the average survival period was just over 7 months, the emergence of the innovative new drug Imfinzi has brought about a shift in the treatment landscape. Compared to the standard chemotherapy regimen, Imfinzi improved overall survival by more than twofold at the 3-year mark, and in a subgroup analysis of Korean patients, the drug demonstrated superior survival benefits over the overall patient population. However, in Korea, patients' access to treatment is still limited due to the high reimbursement barrier. It has been almost three years since Imfinzi was approved by the Ministry of Food and Drug Safety as a first-line treatment for metastatic biliary tract cancer, but there has been no concrete progress on reimbursement since it was approved by the Cancer Disease Review Committee in November 2024. Jung Yong Hong, Professor of Hematology and Oncology at Samsung Medical Center, said, “The ultimate goal of the government, pharmaceutical companies, and healthcare professionals is to provide the verified treatment benefits of Imfinzi as standard therapy to patients with biliary tract cancer as quickly as possible. We must explore ways to strengthen institutional flexibility to enhance treatment access for patients with bile duct cancer.” Korea applies a relatively strict ICER criteria in the pharmacoeconomic evaluation process for innovative new drugs. The lower the cost of existing treatments and the longer the extended survival period, the more unfavorably the ICER value is set. In other words, when compared to chemotherapy approved 20 years ago, the cost-effectiveness of Imfinzi is difficult to fully reflect under the current evaluation system. It is encouraging that there is a growing movement in Korea to flexibly apply ICER thresholds. In February, the Health Insurance Review and Assessment Service applied more flexible ICER standards than before in the process of evaluating the appropriateness of reimbursement for Trodelvy (sacituzumab), a targeted therapy for triple-negative breast cancer. The government is also gradually promoting institutional improvements to increase patient access to new drugs. At a recent policy debate, Jung-kyu Lee, Director of the Bureau of Health Insurance Policy at MOHW, said, “We agree on the need to introduce blended pricing and will comprehensively review the matter to ensure that innovative new drugs are supplied at the right time,” raising expectations for future system improvements. Given that the government has directly mentioned the possibility of institutional improvements, attention is focused on whether discussions regarding the flexible application of ICER and the introduction of blended pricing will lead to actual cases, enabling prompter access to innovative drugs such as Imfinzi to patients with biliary tract cancer. Meanwhile, countries such as Canada, the United Kingdom, Australia, Japan, and Taiwan have acknowledged the clinical innovativeness of Imfinzi and moved quickly to provide reimbursement. In the case of the UK, considering the dire treatment landscape for biliary tract cancer and the fact that Imfinzi is the first first-line treatment for this indication, an exception was made during pharmacoeconomic evaluations by applying a weighted adjustment to Quality-Adjusted Life Years (QALY), thereby allowing for a more flexible application of the ICER threshold.
- Company
- K-Bios head to ASCO…anticancer drugs to AI predictions
- by Kim, Jin-Gu May 27, 2025 06:18am
- Korean pharmaceutical and biotech companies set out to participate in the 2025 American Society of Clinical Oncology (ASCO) Annual Meeting, which is just 5 days away. At ASCO 2025, LG Chem's U.S. subsidiary Aveo Oncology, along with Tium Bio, Onconic Therapeutics, and ImmuneOncia, will each present clinical trial results about their anticancer drugs. Lunit plans to introduce a large number of results on the accuracy of AI-derived treatment response predictions for anticancer drugs. ASCO 2025 will be held from the 30th of this month to the 3rd of next month in Chicago, U.S. It is recognized as one of the world's three major cancer academic conferences, along with the American Association for Cancer Research (AACR) and the European Society for Medical Oncology (ESMO). Every year, over 400 companies from 120 countries around the world participate to present the latest cancer data. LG Chem subsidiary Aveo Oncology to announce Phase III trial results for kidney cancer drug Fotivda According to industry sources on the 26th, LG Chem, Tium Bio, Onconic Therapeutics, ImmuneOncia, and Lunit are among the domestic pharmaceutical and biotech companies that will present clinical results at this year's event. LG Chem will present the latest data on its independently developed kidney cancer treatment ‘Fotivda (tivozanib)’ through its US subsidiary Aveo Oncology (AVEO). Aveo Oncology received approval for Fotivda from the European Medicines Agency (EMA) in 2017 and the U.S. Food and Drug Administration (FDA) in 2021. LG Chem acquired Aveo Oncology in 2022 for USD 571 million (approximately KRW 700 billion). The study being presented this time is the global Phase III TiNivo-2 trial. It evaluates the efficacy of Fotivda in combination with Opdivo (nivolumab) or as monotherapy as a second-line treatment for patients with metastatic renal cell carcinoma who have previously received treatment with Opdivo (nivolumab)+Yervoy (ipilimumab) or VEGF TKI +immunotherapy. Given that the previous Phase III clinical trial on the same Fotivda+Opdivo combination failed to meet the primary endpoint, attention is focused on whether the reattempt made by the company with a different clinical strategy succeeded. Aveo Oncology stated that the results of the control group receiving Fotivda monotherapy in the clinical trial confirmed the drug’s potential as a second-line treatment. The company explained that the PFS endpoint demonstrated clinical significance with Fotivda monotherapy. Aveo Oncology will also announce the results of a Phase III trial for its head and neck cancer treatment candidate, ficlatuzumab. Ficlatuzumab is a monoclonal antibody-based targeted anticancer drug that inhibits the action of hepatocyte growth factor (HGF), which promotes tumor growth. LG Chem will present the results of a Phase III trial comparing the combination therapy of ficlatuzumab and Erbitux (cetuximab) with Erbitux monotherapy as a control group for the treatment of head and neck cancer. In addition, the company will present a poster on the Phase Ib dose-escalation trial of AV-380, an anti-GDF15 antibody for the treatment of cancer cachexia. Tium Bio, Onconic Therapeutics, and ImmuneOncia to present interim clinical results Tium Bio will present the interim results from a Phase II clinical trial of its candidate drug 'TU2218' that targets biliary tract cancer and head and neck cancer, in combination with the immunotherapy drug 'Keytruda (pembrolizumab)’ for the first time. TU2218 is an oral dual inhibitor that simultaneously blocks the signaling pathways of 'transforming growth factor (TGF-β)' and 'vascular endothelial growth factor (VEGF),' which are involved in cancer cell growth and metastasis, thereby maximizing the response rate of immunotherapy agents like Keytruda. The company explained that the dual-target mechanism that targets TGF-β and VEGF improves the tumor microenvironment (TME), thereby enhancing the sensitivity. Tium Bio is conducting a Phase II clinical trial on TU2218 to enter the market as a first- and second-line treatment for head and neck cancer and biliary tract cancer. Existing treatments for head and neck cancer and biliary tract cancer have a short overall survival (OS) of 6 months to 1 year. The company explained, “TU2218 has secured significant OS extension data in an with high unmet need.” Onconic Therapeutics will present two clinical data updates related to its next-generation dual-targeted anticancer drug candidate, nesuparib. The first presentation will be about the Phase Ib/II and Phase Ib trials in progress for metastatic pancreatic cancer. Pancreatic cancer is a representative intractable cancer with limited treatment options, and the company explained that the presentation is significant in that it explores the potential of nesuparib as a treatment option for this disease. The second presentation will be about the PENELOPE study, a Phase 2 investigator-initiated clinical trial in progress for endometrial cancer patients. This trial is exploring the combination of Nesuparib and the immune checkpoint inhibitor Keytruda as a new treatment option for endometrial cancer. An Onconic Therapeutics representative said, “The presentations show that nesuparib is receiving attention as a new option in the fields of pancreatic cancer and endometrial cancer, where treatment options are limited. We will accelerate development to benefit patients in need and demonstrate the value of nesuparib through the global oncology community.” ImmuneOncia has also announced plans to present clinical data at ASCO 2025. The presentation is expected to highlight promising results from the Phase Ib clinical trial of IMC-002, a monoclonal antibody targeting the immune checkpoint protein CD47. This drug works by blocking the CD47 and SIRPα signals, thereby enabling macrophages to eliminate cancer cells. Lunit announces AI-derived “anticancer drug response prediction technology” results Lunit will showcase a range of AI-derived technologies for predicting the response to anticancer drugs. Lunit announced that it will present 12 research findings utilizing its AI biomarker platform 'Lunit Scope' at ASCO 2025. The most notable data is the results of a study predicting the efficacy of Enhertu (trastuzumab deruxtecan) in patients with HER2-positive biliary tract cancer. Conducted in collaboration with Japan’s National Cancer Center East (NCCE), the study analyzed 288 immune histochemistry (IHC) slide images of HER2-positive bile duct cancer patients using Lunit Scope's 'uIHC' technology to quantitatively evaluate the intensity of HER2 expression and its distribution within cells (cell membrane, cytoplasm, etc.). The results demonstrated that Lunit AI not only accurately assessed the intensity of HER2 expression but also that the cell membrane specificity of HER2 expression was a better predictor of treatment response in patients. Among 29 patients treated with Enhertu, those with high HER2 cell membrane specificity had a median progression-free survival (mPFS) of 11.0 months, compared to 4.2 months in patients with low cell membrane specificity, indicating improved treatment outcomes. Among the patients identified by AI, additional patients who were not detected by conventional HER2 expression intensity measurement methods were included, suggesting that the AI-derived cell membrane specificity analysis method can identify more patients responsive to Enhertu treatment compared to the conventional method. Additionally, Lunit is presenting research results on AI-based prediction of claudin 18.2 (CLDN18.2) expression and immune phenotype in gastric cancer patients. According to Lunit, claudin 18.2-targeted therapy has emerged as a new alternative for gastric cancer treatment, but practical limitations have arisen due to sample shortages and the additional costs and time required. To address this, Lunit developed an AI model that predicts Claudin18.2 expression using only basic H&E slides. The model demonstrated a high AUROC value of 0.751, indicating its ability to predict Claudin18.2-positive patients in a gastric cancer patient population. Claudin 18.2 expression is also associated with the response to immune checkpoint inhibitors, and it has been confirmed that it significantly extends progression-free survival (PFS) and overall survival (OS) compared to chemotherapy alone. Generally, early clinical or preclinical results are presented at AACR, and late-stage clinical results at ASCO, rendering more active technology transfer and partnership discussions at the ASCO event. Given the commercial value of late-stage clinical data, the achievements of domestic pharmaceutical and biotech companies at the event are expected to serve as a stepping stone for their future global market entry.
- Policy
- Rinvoq reimbursed for active progressive psoriatic arthritis
- by Whang, byung-woo May 27, 2025 06:18am
- Pic of Rinvoq AbbVie Korea's Rinvoq has become the first oral JAK inhibitor to be covered by insurance for psoriatic arthritis in Korea. On the 26th, AbbVie Korea announced that Rinvoq (upadacitinib), a once-daily oral treatment and selective JAK inhibitor, will be reimbursed for the treatment of active and progressive psoriatic arthritis in adults starting June 1, in accordance with the Ministry of Health and Welfare’s official notification. With the reimbursement decision, adult patients with active and progressive psoriatic arthritis who have been treated with two or more types of disease-modifying antirheumatic drugs (DMARDs) for a total of six months or more (at least three months each) but have not responded adequately to treatment or have discontinued treatment due to side effects will now be eligible for Rinvoq’s use with insurance reimbursement. An initial evaluation will be conducted three months after administration of Rinvoq, and if the number of active joints is reduced by 30% or more, insurance coverage will continue, with evaluations conducted every 6 months thereafter. In addition, if treatment with tumor necrosis factor inhibitors, interleukin inhibitors, or phosphodiesterase-4 inhibitors is ineffective or cannot be continued due to side effects, or if medication compliance needs to be improved, insurance reimbursement will be granted even if the patient has switched to Rinvoq. In such cases, a treatment recommendation form for the switch must be attached, and the patient is recommended to maintain the use of the new treatment for at least 6 months after the switch. Seung-Jae Hong, Professor of Rheumatology at Kyung Hee University Hospital said, “Psoriatic arthritis greatly affects the quality of life of patients, but many patients still struggle to find treatment options to reduce disease activity. Rinvoq, which has been approved for insurance reimbursement, has been shown in clinical studies to improve joint symptoms and significantly improve the quality of life of patients by restoring physical function and reducing fatigue.” Professor Hong also noted, “With the convenience of once-daily oral administration, we anticipate that this treatment to become a practical and useful option in practice.”, This insurance reimbursement was approved based on Rinvoq’s efficacy and safety confirmed in SELECT-PsA 1 and SELECT-PsA 2, which are phase III, multicenter, randomized, double-blind, placebo-controlled clinical studies in patients with moderate-to-severe adult active and progressive psoriatic arthritis. SELECT-PsA 1 included patients who had an inadequate response to or were unable to tolerate one or more non-biologic disease-modifying antirheumatic drugs (DMARDs), while SELECT-PsA 2 included patients who had an inadequate response to or were unable to tolerate one or more biologic disease-modifying antirheumatic drugs.
- Company
- 'Wegovy' dominating the South Korean obesity drug market
- by Chon, Seung-Hyun May 27, 2025 06:17am
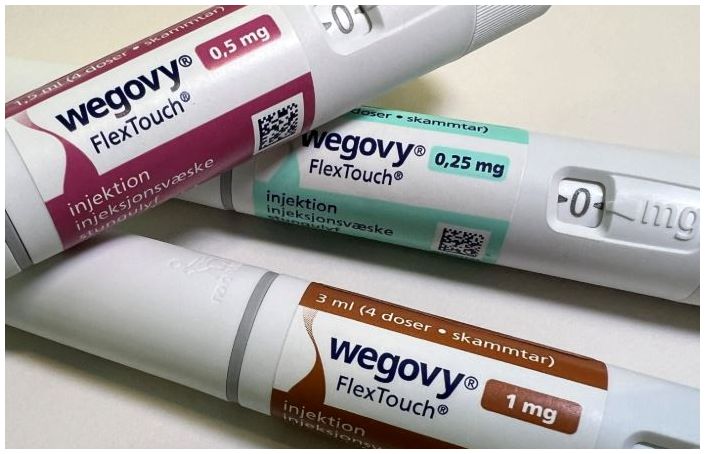
- Novo Nordisk's Wegovy has dominated the South Korean obesity treatment market, establishing a monopolistic competition with over 70% market share. In just six months since its launch in Korea, Wegovy generated a sensation, surpassing KRW 100 billion in cumulative sales. Wegovy's success has expanded the obesity drug market to its largest size ever, while sales of Saxenda, which previously led the market, sharply declined. According to pharmaceutical market research firm IQVIA, on May 26, the obesity drug market reached KRW 108.6 billion in the first quarter of this year, a 162.3% increase compared to KRW 41.4 billion in the same period last year. This is the first time the quarterly obesity drug market size has exceeded KRW 100 billion. Quarterly Obesity Treatment Market Size and Key Product Sales. Legend: Bars-obesity market, Black-Wegovy, Purple-Qsymia, Green-Saxenda (Unit: KRW 100 million, Source: IQVIA) Novo Nordisk's Wegovy clearly stood out. In the first quarter, Wegovy's sales recorded KRW 79.4 billion, accounting for a dominant 73.2% of the entire obesity drug market. Wegovy, which was approved by the Ministry of Food and Drug Administration (MFDS) in April 2023, is a GLP-1 analogue containing semaglutide, known to reduce HbA1c. Novo Nordisk developed Wegovy as a once-weekly obesity treatment using semaglutide after observing weight loss effects in patients during clinical trials of GLP-1 class diabetes drug candidates. Wegovy gained immense popularity immediately after its domestic launch in October last year. Despite its high price, prescription demand surged due to its significant weight loss efficacy. Wegovy's sales reached KRW 60.3 billion in the fourth quarter of last year, propelling it to the top of the obesity drug market. The obesity drug market size was KRW 47.4 billion in the third quarter of last year, but it soared by 97.9% to KRW 93.8 billion in just one quarter following Wegovy's launch. Wegovy held a 63.4% market share in the obesity drug market in the fourth quarter of last year, and its share has continued to rise this year. Under six months since its domestic release, Wegovy's cumulative sales reached KRW 139.8 billion, exceeding KRW 100 billion. Wegovy is thriving globally due to its groundbreaking weight loss effects. Wegovy's sales last year reached DKK 58.26 billion (approximately KRW 11.7 trillion), an 85.7% increase from DKK 31.343 billion in 2023. Demand for Wegovy surged to the point of shortages after its launch in the U.S. market. Even before its domestic launch, Wegovy gained global fame for shortages, having been rumored as the weight loss secret of international celebrities like Tesla CEO Elon Musk. Despite its high price of around KRW 500,000, Wegovy gained explosive interest immediately after its domestic release, leading to supply shortages. Even with the suspension of non-face-to-face prescriptions, demand for Wegovy continued to rise. Initially, Wegovy was actively prescribed through non-face-to-face medical consultations. When concerns were raised that Wegovy was being indiscriminately prescribed via non-face-to-face consultations regardless of a person's weight or obesity status, health authorities suspended non-face-to-face prescriptions for obesity treatments from December 16 of last year. The introduction of Wegovy has led to a reduction in sales of Saxenda and Qsymia, which previously dominated the obesity drug market. The presence of Novo Nordisk's Saxenda has significantly declined in the obesity drug market. Saxenda's first-quarter sales were KRW 4.2 billion, down 72.3% from KRW 15.1 billion in the same period last year. Compared to its KRW 24.2 billion sales in the second quarter of last year, its sales have sharply declined to less than 20%. Saxenda, launched in Korea in 2018, was the world's first obesity drug approved as a GLP-1 analog. Saxenda's active ingredient, liraglutide, is identical to Victoza's, prescribed for type 2 diabetes patients, differing only in dosage and administration. The analysis suggests that Wegovy, a GLP-1 class drug similar to Saxenda, has further taken Saxenda's market. With reduced domestic supply since Wegovy's launch, there are rumors of Saxenda's production being discontinued. After becoming the obesity treatment market leader with sales of KRW 42.6 billion immediately after its launch in 2019, Saxenda maintained its lead for five consecutive years until 2023. Saxenda's sales reached KRW 66.8 billion in 2023, accounting for 37.5% of the obesity treatment market that year. However, following the introduction of Wegovy, Saxenda's sales sharply declined, and its market share in the first quarter of this year was only 3.8%. The first-quarter sales of Alvogen Korea's Qsymia decreased by 3.9% year-on-year to KRW 8.6 billion. Launched in late 2019, Qsymia is a combination drug containing 'phentermine' and 'topiramate'. Alvogen Korea secured domestic marketing rights from U.S.-based Vivus in 2017. Alvogen Korea entered a co-promotion agreement with Chong Kun Dang in late 2019 and began full-scale sales in Korea. Qsymia recorded KRW 10.2 billion in sales in the third quarter of last year but fell to 9.3 billion KRW in the fourth quarter, when Wegovy was launched, and has further decreased this year.
- Company
- Re-evaluation possibility of 'Bylvay' gathers attention
- by Eo, Yun-Ho May 26, 2025 05:57am
- Product photo of Ipsen KoreaAttention has been drawn to when 'Bylvay Cap,' the first medicine chosen for the 'Pilot Project for Integration of Product Approvals, Reimbursement Coverage Reviews, and Drug Price Negotiations,' will be re-evaluated. Bylvay (odevixibat), Ipsen Korea's treatment option for progressive familial intrahepatic cholestasis (PFIC) in patients aged 3 months or older, received a decision of reevaluation at the Health Insurance Review and Assessment Service (HIRA)'s Drug Reimbursement Evaluation Committee (DREC) meeting held in April. After that, the drug had not been considered for the DREC review in May so it will likely be considered for the upcoming review. As part of implementing the first concurrent approval-evaluation-negotiation pilot project since October, the government selected two medicines, including 'Qarziba (dinutuximab)' for treating rare disease in children and Bylvay, as the first drugs for the pilot project. The concurrent approval-evaluation-negotiation pilot project conducts the Ministry of Food and Drug Safety (MFDS)'s approval, HIRA's drug evaluation, and drug pricing simultaneously, expediting the insurance listing process, including approval, drug evaluation, and the Ministry of Health and Welfare (MOHW) reporting. However, Bylvay not being approved for reimbursement has raised questions about the validity of the expedited listing of selected drugs. Furthermore, Bylvay was challenged at the stage of setting the reimbursement criteria. It has been reported that the company poorly took the expert advice while setting the reimbursement criteria because the expert advice gathering process was reduced to merely a 'formality.' In response, the HIRA stated, "To facilitate DREC's efficient evaluation, HIRA operates a small committee for setting reimbursement criteria before a review. At the small committee meeting, HIRA was reviewed in depth by gathering advice from experts and academics regarding clinical usefulness and cost-effectiveness. It was not indeed a thorough process rather than merely a formality." It is to be watched whether Bylvay, which was selected for the concurrent approval-reimbrusement-drug price pilot project, is to be included in the reimbursement list. Meanwhile, the efficacy of Bylvay was demonstrated through the Phase 3 ASSERT study involving children and adolescent patients aged 17 years and below. The study results demonstrated that Bylvay reduced itchiness statistically significantly compared to a placebo, meeting the primary endpoint. Furthermore, Bylvay statistically improved the average serum bile acid concentration at the primary endpoint target time-points, at week 20 and week 24, than the placebo. This effect of Bylvay continued through 24 weeks of treatment.
- Policy
- Moderate-risk trial granted for 'Amtagvi' for melanoma
- by Lee, Jeong-Hwan May 26, 2025 05:56am
- The government has approved a moderate-risk clinical study to treat refractory melanoma patients using the T-cell therapy, Amtagvi. The government also approved a high-risk clinical study that administer multi-virus antigen-specific immune T-cells to pediatric and adolescent patients with resistant·refractory multi-virus infections who underwent allogeneic hematopoietic stem cell transplantation. On May 23, the Ministry of Health and Welfare (MOHW) announced these decisions as part of the resolution results of the 5th Advanced Regenerative Medical and Advanced Biopharmaceutical Review Committee. The Committee reviewed a total of four clinical study plans (two high-risk, two moderate-risk) from institutions, including Catholic University of Korea Seoul St. Mary's Hospital and Samsung Medical Center. Of these, two were approved, and two were deemed unsuitable. Approval of 'Amtagvi' clinical study for melanoma patients The approved project is a moderate-risk clinical study to evaluate the safety and efficacy of tumor-infiltrating lymphocytes (TIL) derived from the patient's own body, in refractory (intractable) melanoma patients who have failed immune checkpoint inhibitor therapy. Melanoma is a malignant tumor originating from melanin cells in the skin. Although it accounts for 1-4% of skin cancers, it has the highest mortality rate. Tumor-infiltrating lymphocytes (TIL) are lymphocytes present in the tumor microenvironment that recognize and destroy tumor cells. They have a high potential to overcome tumor heterogeneity and tumor cell immune evasion, leading to tumor cell death. The TIL therapy 'Amtagvi' is the world's first approved T-cell therapy for solid tumors. Clinical trials of TIL therapy are currently underway for various solid tumors both domestically and internationally. This study aims to evaluate safety by confirming adverse reactions and to assess efficacy by checking objective response rates and progression-free survival, following the administration of TILs manufactured using a domestically developed method. This is to provide a new treatment option using TIL for domestic melanoma patients who have failed most existing treatments. Approved for T-cell therapy in multi-virus infected patients The study was a high-risk clinical study that involved administering multi-virus antigen-specific immune T-cells (VST) to pediatric and adolescent patients who have undergone allogeneic hematopoietic stem cell transplantation and show resistance· refractoriness to standard treatment for multi-virus infections or related infectious diseases. Graft-versus-host disease (GVHD), which primarily occurs during allogeneic hematopoietic stem cell transplantation, is a major severe complication where donor immune cells attack the patient's tissues. To manage this, strong immunosuppressants are used, and as a side effect, the patient's overall immunity is weakened, making them susceptible to infections. This leads to the reactivation of latent viruses within the patient's body, causing infections. Existing antiviral drugs find it difficult to suppress multiple viruses simultaneously, can lead to resistance with long-term use, and have high kidney·liver toxicity. This study aims to simultaneously suppress multiple viruses using VSTs and prevent long-term recurrence through immune memory. The director of the Minister of Food and Drug Safety (MFDS) informed the committee that the research data submitted by the researchers were valid through a rapid and combined review of the high-risk clinical study. Following the procedure, regenerative clinics will conduct the clinical study after receiving approval notification from the MFDS. Kim Woo-ki, Secretary-General of the Advanced Regenerative Medical and Advanced Biopharmaceutical Review Committee, explained, "Based on a re-deliberation decision regarding clinical study plans that required adjustments, the committee granted final approval so researchers can submit supplements."
- Policy
- Amgen’s SCLC drug tarlatamab soon to be approved in KOR
- by Lee, Hye-Kyung May 26, 2025 05:55am
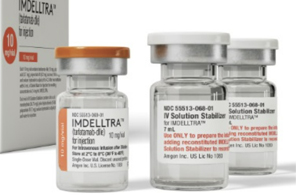
- The approval of Amgen's new drug for small cell lung cancer, tarlatamab (U.S. brand name Imdelltra), is imminent in Korea. According to industry sources on the 23rd, the Ministry of Food and Drug Safety has completed its safety and efficacy review for tarlatamab. The MFDS's completion of the review means a new drug approval will follow soon. Tarlatamab was designated as a “GIFT” item by the MFDS in January last year and underwent a fast-track review upon the submission of the new drug application. In the United States, the FDA designated tarlatamab as breakthrough therapy in October 2023 and granted accelerated approval on May 16, 2024, for the treatment of adult patients with extensive-stage small cell lung cancer (ES-SCLC) whose disease has progressed during or after platinum-based chemotherapy. Tarlatamab is a bispecific antibody that recognizes antigens in both tumor cells and T cells (immune cells). This allows for the drug to induce T cells to attack tumor cells even when the tumor cells try to avoid them. This drug demonstrated efficacy in the Phase II DeLLphi-301 trial. The trial evaluated the efficacy of tarlatamab in patients with SCLC who had failed two or more prior lines of treatment. The patients that enrolled in the trial received tarlatamab 10 mg every two weeks. The team recruited and randomized 220 patients who had failed first-line treatment for small cell lung cancer at 56 centers in 17 countries around the world, to find a new treatment strategy that would maximize the effectiveness of tarlatamab, which is currently under development while maintaining patient safety. Results showed that the group of subjects who received tarlatamab 100 mg every 2 weeks achieved an objective response rate of 40%, with a median response duration of 9.7 months. The median overall survival was 14.3 months. Currently, available treatments for small cell lung cancer in Korea include the immunotherapy drug 'Imfinzi (durvalumab)' and the chemotherapy drug ‘Zepzelca (lurbinectedin).'