- LOGIN
- MemberShip
- 2026-04-04 07:31:08
- Policy
- AZ’s Imjudo and Imfinzi both make reimbursement progress
- by Lee, Tak-Sun Nov 15, 2024 05:49am
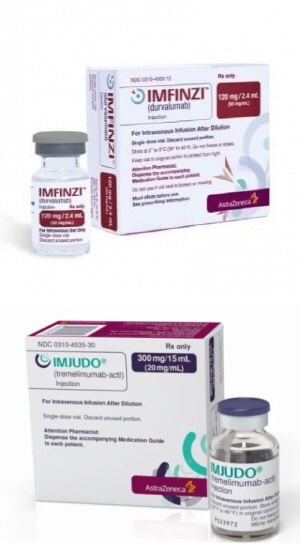
- AstraZeneca (AZ) Korea’s ‘Imjudo Inj.’ Has passed the first step to reimbursement listing in Korea. Also, reimbursement standards for ‘Imfinzi Inj,’ which is seeking reimbursement expansions, were set. However, these are only the first steps to reimbursement. On the 13th, the Health Insurance Review and Assessment Service held the 8th Cancer Disease Review Committee in 2024 to deliberate on the reimbursement standards for anticancer drugs. As a result of the deliberation, reimbursement standards were set for the new drug Imjudo Inj (tremelimumab) but not for Tecvayli Inj (teclistamab, Janssen). Imjudo is indicated for the first-line treatment of adult patients with advanced or unresectable HCC in combination with durvalumab. Here, durvalumab is AZ's immuno-oncology drug Imfinzi. Imfinzi is indicated for the treatment of patients with unresectable locally advanced non-small cell lung cancer (NSCLC) whose disease has not progressed after platinum-based concurrent chemoradiotherapy (CCRT). However, based on clinical results, the company has been seeking to expand its coverage to include liver and biliary tract cancers. One such example is the Imfinzi-Imjudo combination as a first-line treatment for liver cancer. Another is biliary tract cancer. Since February, Imfinzi+gemcitabine+cisplatin has been used for the first-line treatment of patients with locally advanced or metastatic biliary tract cancer. However, Imfinzi is currently paid fully out-of-pocket. As Imfinzi is an expensive drug, costing KRW 3,347,202 per bottle, healthcare professionals as well as patients have been requesting Imfinzi be covered by the government. The patients' voices were also discussed as an agenda at the last national audit. In response, HIRA had promised a proper review. On this day, their efforts bore fruit. Reimbursement standards were finally set for the drugs. With both drugs being set reimbursement standards, AZ can now look forward to the prompt reimbursement of both of its drugs. However, another AZ drug - Tagrisso (osimertinib mesylate), the company's flagship treatment for non-small cell lung cancer- failed to make the cut. The company sought to set reimbursement standards for Tagrisso in combination with pemetrexed plus platinum-based chemotherapy in the first-line treatment of patients with locally advanced or metastatic non-squamous NSCLC with an EGFR exon 19 deletion or exon 21 (L858R) substitution mutation, but the application was not accepted. On the same day, the CDDC deliberated on reimbursement standard improvements proposed by medical societies. As a result, requests to improve the phrase - “failed chemotherapy including docetaxel” - wording in the subjects for prostate cancer chemotherapy, and suggestions regarding the administration of palliative therapy in case of recurrence/metastasis during or after the administration of adjuvant therapy, were accepted.
- Company
- Leqvio with 'twice-yearly treatment' set for mkt
- by Whang, byung-woo Nov 15, 2024 05:49am
- Leqvio is set to challenge the market with its superior drug tolerance, administered twice yearly, compared to existing treatments. Product photo of Leqvio.According to the pharmaceutical industry on November 15, Novartis Korea launched the siRNA therapy Leqvio (inclisiran) on November 11. Lecvio is the first-in-class siRNA drug approved in South Korea. It is approved as an adjunct to dietary therapy for patients with primary hypercholesterolemia (heterozygous familial and non-familial) and mixed dyslipidemia. Leqvio uses naturally occurring siRNA to block PCSK9 protein production and lower LDL cholesterol levels. It has the advantage of its twice-yearly administration by doctors, reducing the challenges associated with self-injection. Novartis is reportedly working to establish prescription access for Leqvio in general hospitals. Industry sources said that Drug Committee (DC) approvals for Leqvio are proceeding across hospitals nationwide, with some hospitals already completing the process. Novartis' Leqvio was launched in South Korea after the product became available. Novartis is expected to start building its prescription sales as the DC reviews advance within general hospitals. With Leqvio prescriptions anticipated, there is growing interest in how Novartis’ domestic sales strategy will unfold. Although specific details have not yet been announced, it is anticipated that Novartis will consider either utilizing its own sales line or engaging in co-promotion with a Korean company. Leqvio's competing drug, Amgen’s Repatha, is co-marketed with Jeil Pharmaceutical. However, given Leqvio’s potential focus in general hospitals, Novartis may utilize its internal sales team. Will Leqvio lead the prescription trend? It will depend securing reimbursement Experts anticipate that Leqvio will have a market presence despite cost hurdles, as cholesterol management trends evolve to prioritize patient convenience along with clinical effectiveness. For hypercholesterolemia patients, maintaining LDL-cholesterol (LDL-C) at recommended levels consistently and early on is crucial in reducing the risk of atherosclerotic cardiovascular disease (ASCVD). Long-term strategies are anticipated to shift toward minimizing the frequency of medication doses for patients, with an increased focus on injection therapies that allow healthcare providers to monitor patient progress directly. "While statins require daily use and Repatha requires 26 injections annually, Leqvio is administered in twice-yearly injections by a doctor," Dr. Byeong-Keuk Kim, a cardiologist at Sinchon Severance Hospital, said. "Doctors face difficulty when patients who don’t respond well to statins. Now, we could have Leqvio as a treatment option." "Leqvio’s six-month dosing schedule could improve drug adherence, potentially resulting in a sustained decrease in LDL-C levels and lower cardiovascular risk in clinical practice," Dr. Kyung Woo Park, a cardiology professor at Seoul National University Hospital, said. However, with the competing PCSK9 inhibitor Repatha already reimbursed, Novartis' primary aim would be on obtaining reimbursement for Leqvio. Repatha’s reimbursed cost is approximately KRW 121,000 per injection, with recommended dosing every two weeks or once monthly at 420 mg (three dosages), bringing annual treatment costs to KRW 1.45 million. Novartis is working on Leqvio's reimbursement listing. The company aims to continue negotiations with the government to establish reimbursement for Leqvio at about KRW 3 million, aligning with Repatha’s annual price. "While Leqvio may be chosen by elderly patients facing adherence challenges or those with poor prognosis, many others already experience significant improvements by combining existing therapies with regular exercise. For some, even a once-monthly Repatha injection successfully maintains desired levels. In my opinion, balancing high costs against the administration convenience needs further discussion," a cardiology professor at a major hospital in Gyeonggi-do said.
- Opinion
- [Reporter’s View] Who’s to blame the new drug reimb delays
- by Eo, Yun-Ho Nov 15, 2024 05:49am
- Expedited approval of new drugs is one of the oldest issues in the pharmaceutical industry. Shortening the insurance reimbursement review period for drugs has been discussed almost every year, and in fact, the regulatory deadline is getting shorter and shorter. This is true for both the evaluation and negotiation stages of the Health Insurance Review and Assessment Service and the National Health Insurance Service. However, it is also true that the deadline is only a deadline set for the pharmaceutical company to apply and the authorities review the application, so it is not proving to be effective in expediting the reimbursement of new drugs. The responsibility lies on both sides. First of all, many pharmaceutical companies spend a considerable amount of time between the post-approval feedback process with their respective headquarters before actually applying for reimbursement - in other words, taking their time weighing up the gains and losses. During this process, the companies may delay the timing of reimbursement to receive a higher price or give up some indications due to competition from other products. Some companies deliberately delay drug price negotiations in anticipation of being included in the government's new coverage plan, while others cancel the introduction of a drug altogether because they believe it is not marketable in Korea. The “Korea-passing” decision, where the companies forego Korea and introduce the drug to other countries first, has become commonplace. In fact, at a recent press conference, HIRA said, “Regarding the time it takes to reimburse a new drug, although the evaluation is carried out within the statutory deadline, there is a difference in the actual time taken to the listing because the companies take a considerable amount of time to supplement their data, etc. In order to quickly register a new drug, the companies must first faithfully complete documents when applying for a decision.” However, the government's “let's complete discussions in the earlier stages and send the agenda to the Drug Reimbursement Committee” decision also plays a role. If you trace back the process of listing a drug that is long overdue for listing, there are certainly cases where the companies had voluntarily withdrawn their application after the Drug Reimbursement Standard Subcommittee decided to delay the review. However, there are many cases where such withdrawal is not “voluntary.” The deferral decision is very common during drug pricing negotiations between the NHIS and pharmaceutical companies. However, we need to remember that the 60-day deadline set for negotiations is a promise, and a deadline is a deadline. Also, the NHIS has referred to the negotiation deadline as a sort of "benefit" when announcing its plan to shorten the deadline for new drugs. The problem is that there is no transparency in the progress made in those 60 days. Nothing is disclosed on what happened to the drugs that exceeded the listing review deadlines. As a result, only the patients are left to suffer in endless await. No answer nor explanation on the direction of progress is provided to those who wait in dire need. This new year, all the stakeholders involved should make collaborative efforts to reduce the period to actual reimbursement listing.
- Company
- Hanmi's new bio drug 'Rolvedon' sales 88%↑ in the US mkt
- by Son, Hyung Min Nov 15, 2024 05:49am
- The U.S. sales of Rolvedon (Korean product name: Rolontis) have substantially increased. Hanmi Pharmaceutical's U.S. partnering company, Assertio, plans to expand market share by securing Rolvedon's indication for the same-day administration. According to Assertio on Novermber 14, Rolveron's sales in the U.S. market in Q3 were US$ 15 million (about KRW 21 billion), up 87.5% Year-over-Year (YoY). Rolvedon has recorded cumulative sales of US$110.30 million (about KRW 155 billion) since its launch in Q4 of 2022. Rolvedon is a treatment for neutropenia developed by Hanmi Pharmaceutical. It is Korea's 33rd new drug, approved in March 2021. After that, Hanmi Pharmaceutical and its U.S. partnering company Spectrum (now Assertio) obtained U.S. Food and Drug Administration (FDA) approval in September of the same year. Rolvedon was outlicensed to the U.S. Spectrum in 2012. After Assertio acquired Spectrum in April last year, it secured the licensing of sales and development of Rolvedon and lung cancer therapy Poziotinib. Rolvedon Since its release in the United States in October 2022, Rolvedon has recorded sales of $10 million within three months. After the product launch, 70 distributors purchased Rolvedon. It was then utilized by the top three community oncology networks, accounting for 22% of the clinic market share. It continued to show strong sales up to Q2 last year. Rolvedon generated sales of $15.6 million in Q1 last year, and in Q2, it recorded $21 million (approx. KRW 28 billion), an increase of 34.6% from the previous quarter. Rolvedon’s sales in Q3 last year slowed down since its launch. It recorded $8 million in Q3 last year, a decrease of 62% from the previous quarter. Regarding sales reduction, Assertio explained that the demand for Rolvedon after applying the reimbursement system was below expectations. Rolvedon successfully rebounded in Q4 last year, generating US$11 million in sales. Rolvedon's sales in Q1 amounted to US$14.50 million and maintained recovery in Q2, recording sales of US$15.10 million. Assertio has high hopes for Rolvedon's same-day administration clinical trial. Currently, Neulasta, jointly developed by Amgen and Kyowa Kirin, is recording over half of the market share in the U.S. market for neutropenia treatment. However, conventional treatments for neutropenia, such as Neulasta, can only be administered 24 hours after cancer therapy, thereby prolonging hospitalization. Assertio plans to gain a competitive edge with its strategy of Rolvedon's same-day administration method. Assertio has recently completed the Phase 1 clinical trial for Rolvedon's same-day administration. The company plans to present the clinical results at the 2024 San Antonio Breast Cancer Symposium (SABCS 2024), held for four days, starting December 10.
- Opinion
- [Reporter's View] The reality of drug shortage reports
- by Lee, Hye-Kyung Nov 14, 2024 05:52am
- Reports of shortages of oxytocin, an injectable drug used primarily as a labor inducer, have caused confusion in the obstetrics and gynecology field. Most obstetrics and gynecology centers that have a large number of expectant mother visits stock enough oxytocin to last 2-3 weeks, but JW Pharmaceuticals, which holds more than 70% of the prescription market, has announced a shortage of its oxytocin supply that will last until January next year. In the case of childbirth, there is no reason for a sudden surge in a drug’s demand like infectious diseases or colds, but oxytocin is designated as a national essential medicine that must ensure a stable supply as it is used to induce labor in mothers. In Korea, only two companies, JW Pharmaceutical and Yuhan Corp, manufacture oxytocin drugs. Since it is a national essential medicine with a small number of manufacturers, it seemed natural that supply and demand management would be in place, but out of the blue, the clinics and hospitals were suddenly just told that “there was no medicine.” A small hospital in a rural area with a low birth rate would have ordered the medicine on a case-by-case basis rather than keep two to three weeks' worth on hand, so the news that it would soon be out of stock must have been like a bolt from the blue. The question that first came to mind was, why is there a national essential medicine system in place if it cannot manage the supply of essential drugs? When looking closer into the situation, the cause was clear: the system was not well established enough to ensure a stable supply of the necessary drugs. The discontinuation of the manufacture, import, and supply of finished drugs must be reported to the Ministry of Food and Drug Safety 60 days before the discontinuation date. However, as the criteria for reporting shortages are set differently in each company's SOP, and there is no absolute threshold set for determining drug shortages. In the case of oxytocin, the MFDS was able to identify the shortage only after looking into Yuhan Corp’s shortage report, a company that only accounts for about 30% of the oxytocin market share. On October 28, the company reported a shortage of oxytocin on the market, stating, “There is also supply disruption for Choongwae Oxytocin Inj.. which is approved with the same ingredient. With no substitute drug available containing the same ingredient, a supply shortage is expected for a period of time, but we will be able to ensure supply from November 14, 2024.” Up until this point, JW Pharmaceutical had not notified the MFDS of its shortage. The problem was that the MFDS was not informed, but the letter sent to obstetrics and gynecology clinics and wholesalers indicated that the drug would be “out of stock until January.” Even if the drug is designated as a national essential medicine, the KFDA cannot know about the shortage without a report from the pharmaceutical company. The MFDS began to investigate the situation when it learned about JW Pharmaceutical’s oxytocin shortage via Yuhan Corp’s supply shortage report. JW Pharmaceutical, which has a higher market share, was unable to manufacture finished drugs due to issues with the API, and the MFDS reportedly supported the necessary measures and moved up the manufacturing date from January next year to December this year. This situation seems to have occurred because the threshold for shortages was not specified. Each company had a different threshold set for sending “out of stock” reports to the MFDS. Yuhan Corp reported a shortage when it crossed its threshold of shipments this year, while JW Pharmaceuticals did not report a shortage until it was likely to run out on site. It's not easy for the MFDS to keep track of the shortages of more than 500 national essential medicines every day. Unless the ministry receives a proper report, they cannot provide the necessary support, but if the product becomes out of stock even before the ministry can consider support, there is no opportunity for the authorities to take action. As a result, no medicine is available on site, with the government ending up taking countermeasures after the damage is made. Last year, the Ministry of Food and Drug Safety revised the Ordinance of the Prime Minister to pull forward the drug shortage report from 60 days to 180 days, with implementation scheduled for April next year. However, if the regulation is revised without a baseline for reporting not established, cases like oxytocin will only repeat itself. We need a system to address stockouts before there is “no medicine” on site.
- Company
- Lee Hyun-ju named as the representative of ZP Therapeutics
- by Eo, Yun-Ho Nov 14, 2024 05:52am
- Lee Hyun-ju, new representative of ZP Therapeutics Korea Lee Hyun-ju (48), ex-Daiichi Sankyo Korea's Oncology Business Franchise Head, was appointed as the new representative of ZP Therapeutics Korea. Industry sources said Zuellig Pharma has recruited Lee Hyun-ju as the new head of ZP Therapeutics Korea, Zuellig Pharma's commercial services corporation. Lee holds a degree from Sungkyunkwan University's College of Pharmacy, and she has years of experience in the Korean pharmaceutical market with expertise in the anticancer business. Lee started her career in 1999, undertook roles in Handok's marketing and Sanofi's marketing, and worked as Roche Korea's Oncology Cluster Lead and Novartis Korea's Hematology Cluster Lead. Lee moved to Daiichi Sankyo's Oncology Cluster last year and served her role until the new appointment. Meanwhile, ZP Therapeutics Korea is committed to providing a comprehensive solution, encompassing marketing, sales promotion, product launch medical e-detailing, registration & approval, market access, digitalization & data analysis-based sales excellence, adapting needs and changes of the pharmaceutical market. ZP Therapeutics Korea established itself as a commercial solution partner sought by pharmaceutical clients. The company is involved in in-licensing of many prescription drugs and over-the-counter (OTC) drug brands. ZP Therapeutics Korea also provides sales & marketing services, supporting major pharmaceutical companies.
- Company
- Celltrion anticipates Trump admin will bring positive shift
- by Whang, byung-woo Nov 14, 2024 05:51am
- Celltrion anticipates that President-elect Donald Trump's second administration in the United States will positively affect the company's biosimilars and Contract Development and Management Operations (CDMO) services. On November 12, Celltrion presented stockholders with the potential impact on the business under the title 'The Business Impact and Outlook upon President-elect Donald Trump's second administration in the United States launches.' Celltrion cited a report from the Korea Institute for Industrial Economics and Trade, 'The potential impacts of the U.S. presidential election on Korean industry and outlook,' and analyzed that the Trump administration will be friendly towards using generics and biosimilars. Currently, healthcare expenditures in the United States accounted for 17.6% of the country's GDP in 2023. As a solution, Trump's first administration implemented initiatives such as the 'Lowering Drug Prices by Putting America First' administrative orders and the 'American Patients First' plan to lower drug prices. These policies include details regarding biosimilars, including 'Improve Competition' and 'Lowering List Prices.' "When President-elect Trump's second administration launches, the administration is expected to take over the policy during the first administration and pursue healthcare policy," Celltrion said. "We expect the administration will favor expanding biosimilar prescriptions, which is Celltrion's main business." Trump's first administration pursued a policy of regulating drug pricing, proposing a bill to Congress to stop pharmaceutical companies from paying rebates to the top 3 pharmacy benefit managers (PBMs) in the United States. Such a move was said to be friendly to the biosimilar market. Additionally, as the administration pursues the PVM reform to alleviate financial loss, a by-product of economic stimulation, by reducing taxes, implementing a policy that expands the use of biosimilars is expected. Such a move is expected to be favorable to Celltrion. In particular, Celltrion anticipated these policies would positively impact its CDMO service, which will be Celltrion's growth momentum. The 'Biosecure Act' bill, the U.S. Congress initiative, 'prohibits entities that receive federal funds from using biotechnology from a biotechnology company of concern may not contract with any entities that do so.' The Biosecure Act is expected to support establishing a new supply network in US-friendly countries with business competitiveness, including South Korea, Japan, and India. "In line with the U.S. industry trend, we will complete establishing the CDMO corporate entity within this year to seize the opportunity to secure demands from Chinese companies," Celltrion added. "Celltrion will secure a new manufacturing plant, as Celltrion's 100% owned subsidiary, in South Korea or overseas to expand production capacity." Additionally, as Trump's second administration's policy priority is the 'America First' agenda, Celltrion anticipates US dollar strength will likely result in trade disputes and interest rate rises. During the process, Celltrion anticipates its products will remain unaffected by tariff increases, as tariffs on drugs are exempt under the WTO's Pharma Agreement. "Upon Trump's second administration launches, we expect the company will have an opportunity to focus mainly on business aspects, marketing expansion and sales growth, compared to other type of business," Celltrion said. "Celltrion will focus on changes to the U.S. biopharmaceutical industry and generate outcomes by maximizing business opportunity," Celltrion emphasized.
- Company
- ‘Access to bispecific antibody Columvi should be improved’
- by Son, Hyung Min Nov 14, 2024 05:51am
- Dr. Chris Fox, Professor of Haematology at the University of Nottingham, U.K. “Diffuse large B-cell lymphoma (DLBCL) is a disease in which one in four patients experience relapse even after treatment. The bispecific antibody Columvi has demonstrated efficacy in relapsed patients at up to 18 months of follow-up. The clinical performance of Columvi is not just an incremental improvement over existing therapies, but a paradigm shift in the DLBCL treatment environment.” At a recent meeting with Dailypharm, Dr. Chris Fox, Professor of Haematology at the University of Nottingham, U.K., recently described so about Columbo, a bispecific antibody approved for diffuse large B-cell lymphoma in Korea. DLBCL is a disease in which the body's protective “B cells” grow or multiply uncontrollably and is the most common form of non-Hodgkin's lymphoma that accounts for about 40% of all non-Hodgkin's lymphomas. The disease is characterized by aggressive, rapidly progressive staging. The number of DLBCL patients in Korea was 14,183 as of last year, a 36% increase from the 10,428 in 2018. Up to 15% of DLBCL patients fail first-line standard therapy, and 25% of patients experience relapse within 18 months despite achieving a complete response (CR). Patients with relapsed or refractory DLBCL show a characteristically rapidly worsening prognosis as the number of treatment cycles increases. Columvi, the first bispecific antibody targeting CD20XCD3 enters the market...offers the advantage of a fixed dosing period The good news is that a variety of new drugs have emerged for this disease. Roche's Polivy, a representative DLBCL drug, is said to be effective in about two-thirds of patients when used as a first-line treatment. However, this means that about one-third of patients who do not respond to first-line treatment remain in need of further options. Bispecific antibodies and chimeric antigen receptor T-cell (CAR-T) therapy, such as Columvi, are used in such cases of relapse. Columvi, the first bispecific antibody to target CD20xCD3 in DLBCL, was launched without reimbursement in Korea in May and is now on the formulary of more than 10 general hospitals. The drug has a 2:1 structure that binds to two CD20 regions on the surface of malignant B cells and one CD3 region on immune T cells, resulting in a stronger binding. Bispecific antibodies have two targets, each targeting a different cell: one that draws immune T cells closer to malignant B cells and the other that activates the T cells to kill the malignant B cells. Based on this mechanism of action, bispecific antibodies have been shown to be effective in patients who are resistant to conventional antibody therapies or chemotherapy. “Bispecific antibodies and CAR-T therapies have been explored as treatment options for DLBCL, but without head-to-head trials, it is difficult to say which is better. The choice of treatment should be based on the individual patient's state of disease progression. However, one of the side effects of CAR-T in elderly patients, immune effector cell-associated neurotoxicity syndrome (ICANS), is considered when selecting a treatment,” said Dr. Fox. He added, “Columvi has a fixed dosing period. It is designed to be administered for up to 12 cycles (8.3 months), so there is a clear end date for the treatment. It also has the advantage of being an off-the-shelf treatment that can be administered to patients immediately.” Columvi achieves 39% CR rate - still effective after 18 months...“justifies the need for its reimbursement” Columvi demonstrated efficacy in the multicenter, open-label Phase I/II NP30179 trial in patients with relapsed or refractory DLBCL after two or more prior systemic therapies. Trial results showed that Columvi achieved a complete response (CR) of 40% and an overall response rate (ORR) of 52%. Among patients who achieved CR, the median duration of response was 26.9 months, with 67% of patients maintaining CR at 18 months. The study also included about one-third of patients who had received prior CAR-T therapy. “Columvi demonstrated a 40% CR rate in the trial, even in patients who are difficult to treat,” said Dr. Fox. This data alone confirms the efficacy of Columvi, as such data cannot be expected with existing standard treatment options, and Columvi is showing similar results in the real world to the clinical trial,” said Dr. Fox. “In DLBCL, relapse typically occurs within 12 to 18 months, and staging progresses rapidly in relapsed patients. We already have data on Columvi’s use in these patients up to 18 months of follow-up. So we can be confident about Columvi’s efficacy data and maintenance of its effect.” However, Columvi’s reimbursement was rejected in July by the Cancer Disease Review Committee, the first gateway to reimbursement in Korea, due to the lack of long-term data. Roche Korea is aiming to reapply for Columvi’s CDDC review later this year. “Patient access to Columvi has been secured in the UK with reimbursement approval,” said Dr. Fox. “This is because the health authorities have recognized Columvi as an effective treatment in DLBCL.” “Columvi is not just an improvement over existing therapies, but a paradigm-shifting treatment for DLBCL. I want to emphasize that this is a treatment that could have an impact on prolonging the survival of patients with relapsed or refractory DLBCL.”
- InterView
- 'Early detection of RA can help prevent severe symptoms'
- by Whang, byung-woo Nov 14, 2024 05:51am
- "Rheumatoid arthritis not only induces permanent joint deformities and damages but also has a detrimental effect on quality of life due to many general symptoms. As effective disease management becomes possible following the recent introduction of various treatment options, early diagnosis and patient-customized treatment approach are crucial." New treatment options for rheumatoid arthritis have improved unmet needs in clinical practices and increased disease awareness. However, despite the rising diagnosis rate, some patients receive a diagnosis after the disease progresses to severe symptoms. Yunjung Choi, Professor in the Division of Rheumatology at Jeonbuk National University Hospital, has emphasized the importance of early diagnosis of rheumatoid arthritis, explaining the disease characteristics and the latest treatment advances. Yunjung Choi, Professor in the Division of Rheumatology at Jeonbuk National University HospitalRheumatoid arthritis is the most common autoimmune disease where abnormally activated immune cells invade joints, causing inflammation and pain. "Rheumatoid arthritis is mainly caused by inflammation in the thin tissue lining of joints. The disease symmetrically affects small joints in the hand and foot, damaging bones and cartilage surrounding the tissue lining of joints. It leads to joint deformities and loss of joint function." Choi added, "JAK inhibitors that can be orally administered and have almost similar effects now enable patients to manage arthritis effectively." The treatment options for rheumatoid arthritis broadened following the introduction of conventional disease-modifying antirheumatic drugs (cDMARDs), biological agents, and Janus Kinase (JAK) inhibitors. "Patients who have not reached treatment goals after being treated with cDMARDs in primary healthcare centers are often transferred to secondary healthcare centers or university hospitals," Choi said. "Many of them are moderate to higher patients who have poor prognosis factors, and they consider either biological agents or JAK inhibitors." "Customizing treatment to individual patient is necessary. For instance, adapting to patient conditions to prevent and manage side effects, ensure administration convenience, and evaluate drug compliance," Choi emphasized. The current clinical practices use cDMARDS, biological agents, and JAK inhibitors based on the 2021 American College of Rheumatology Guideline and the 2022 European Alliance of Associations for Rheumatology classification recommendations. With JAK inhibitors recently added to the reimbursement list, patients now have treatment options that offer the convenience of oral administration, less burden than injectables, and high efficacy comparable to biological agents. Choi said such a change has contributed to increased patient drug compliance and provided effective treatment options to medical practitioners. Regarding the benefits of JAK inhibitors, Choi said, "At first, there were concerns about JAK inhibitors for cardiovascular system-associated side effects, but follow-up research outcomes have shown that such risks are gradually alleviating." Choi added, "We hope more data in South Korea becomes available and anticipate safer drug use considering ages and existing health conditions." "There is a need for improvements in the rheumatoid arthritis system with blind spot" Furthermore, there is a need to improve a system regarding drug switching for rheumatoid arthritis treatment. For instance, switching to another JAK inhibitor is difficult when a patient does not respond to a JAK inhibitor. Some people have demanded systematic improvements. Positive changes are expected regarding this issue. The Health Insurance Review and Assessment Service (HIRA) has suggested a criterion for drug switching needs, establishing 'An assessment criterion for evaluating drug switching effects for rheumatoid arthritis.' In addition, Choi emphasizes the need to expand support for patients with serotype-negative rheumatoid arthritis. "About 80% of patients with rheumatoid arthritis are diagnosed with antibody positivity. But, the rest of the 20% are found to be antibody-negative, posing difficulty in receiving benefits," Choi said. "These patients require treatments their whole lives, experiencing joint damage and functional deficits. Because they are excluded from benefits, improvements to the policy may be necessary." Additionally, Choi pointed out that patients who use biological agents are recommended for immunization to prevent shingles, but many experience considerable cost burdens. "Shingles immunization is crucial for patient safety, but its high cost poses an additional burden to patients. Systematic support is required to lower the economical hurdle," Choi said. Lastly, Choi reiterates the importance of early diagnosis to seize the 'golden time' for treating rheumatoid arthritis. "Many patients endure symptoms thinking that they feel pain from using their hands frequently, but end up visiting hospitals once the disease has worsened. When an individual feels one's hand stiff and hard to grasp, and feels extensive pain in the body, one should not disregard it simply as fatigue," Choi advises. When morning stiffness lasts over 30 minutes on more than two occasions within two weeks, it may indicate early rheumatoid arthritis. Individuals must consult rheumatology specialists for an accurate diagnosis and a suitable treatment plan. "An early intervention makes a significant difference in preventing joint damages and preserving quality of life," Choi said. "Patients need to recognize disease early and proactively seek treatments."
- Company
- Global CDMOs compete to expand ADC capacities
- by Kim, Jin-Gu Nov 14, 2024 05:51am
- Global competition is heating up in the contract development manufacturing organization (CDMO) market for antibody-drug conjugates (ADCs). Major players include Switzerland's Lonza and Samsung Biologics, the world's top two CDMOs, which are competitively expanding their manufacturing facilities. Lonza recently announced the expansion of a 1,200-liter ADC manufacturing facility, while Samsung Biologics announced the start-up of a 500-liter ADC manufacturing facility within the year. According to KoreaBIO, Lonza announced on Dec. 13 (local time) that it plans to add 2 manufacturing facilities in Visp, Switzerland, to expand its 'bioconjugation' service. An additional 1,200-liter manufacturing facility will be built to produce commercial bioconjugates, including ADCs, in high volumes. At the same time, the company will expand the infrastructure of the existing facility. Construction is expected to be completed and the facility fully operational by 2028. The new manufacturing facility will provide comprehensive end-to-end lifecycle support. This includes drug manufacturing for early-stage clinical development, large-scale manufacturing for commercial supply, and finished product filling services. Lonza has been in the bioconjugate CDMO business since 2006. To date, it has produced more than 1,-00 cGMP batches for more than 70 programs. Christian Morello, Vice President, Head of Bioconjugates, Lonza, said, “We continue to see strong growth in the bioconjugates space as ADCs and other bioconjugated drugs increasingly progress towards commercialization. This investment in our multipurpose commercial bioconjugation capacity addresses the growing market demand, enables us to support the growth of our customers, and offers a flexible and integrated service for manufacturing bioconjugates.” The global CDMO market, including Lonza, has recently been intensely competing to expand capacities around ADC drugs. Samsung Biologics is building a dedicated 500-liter ADC manufacturing facility at its Songdo Biocampus in Incheon, South Korea. The company plans to finalize the construction this year and begin full-scale operation after receiving GMP approval. Lotte Biologics is expanding its ADC manufacturing facility at its Syracuse, USA plant. This is an investment of USD 80 million (approximately KRW 100 billion). The ADC manufacturing facility is currently being expanded and is targeting GMP approval in the first quarter of next year. The company is also in the process of building a related plant in Songdo, Incheon. In addition, Celltrion plans to establish a separate CDMO subsidiary while pursuing ADC drug development. Kyongbo Pharmaceutical is investing KRW 85.5 billion to build an ADC plant. The reason why domestic and foreign CDMOs are rushing to expand production capacity for ADC drugs is due to their marketability and high barriers to entry. ADC is a type of antibody conjugated with a cytotoxic drug (payload) as a linker. They have a high structural complexity compared to conventional antibody drugs, which makes the development and manufacturing process difficult, but they have emerged as the next generation of biopharmaceuticals due to their relatively high therapeutic efficacy and low side effects. Following the success of Daiichi Sankyo's breast cancer drug Enhertu (trastuzumab deruxtecan), research on ADC drugs has increased explosively worldwide. However, facilities for the development and mass manufacture of ADC drugs have not been able to keep pace. This is why an imbalance between ADC-related research and manufacturing is expected in the field. Unlike conventional antibody drug CDMOs, ADC-specific manufacturing facilities require more particular technologies. Unlike antibody drug production facilities, ADC production facilities must incorporate additional design principles because they handle cytotoxic drugs (payloads) and organic solvents. Additional design details include negative pressure design, differential pressure between cleanrooms, and airlocks to prevent the spread of cytotoxic drugs and protect operators.