- LOGIN
- MemberShip
- 2026-04-07 09:51:40
- Company
- ‘Long-term treatment for osteoporosis is now possible'
- by Son, Hyung-Min Jun 20, 2024 05:48am
- Dr. Byung Ho Lee, professor of Orthopedic Surgery at Gangnam Severance Hospital The improved reimbursement standards for osteoporosis drugs have created a treatment environment that promotes fracture prevention. Healthcare professionals have pointed out that the treatment continuation rate of osteoporosis patients has been low stressing the importance of continuous treatment to minimize the risk of fracture. On Sept. 19, Amgen Korea held a media session at the Lotte Hotel in Jung-gu, Seoul, to introduce its treatment strategies in response to the changing osteoporosis treatment environment in Korea. The Ministry of Health and Welfare expanded the duration of reimbursement for major osteoporosis treatments last month. Previously, only patients with a T-score of -2.5 or lower using dual-energy x-ray absorptiometry (DXA) were eligible for reimbursement, but those with a T-score of -2.5 or higher and -2.0 or lower can now receive reimbursement for their treatments for up to 2 years. Experts such as the Korean Society of Osteoporosis and the Korean Society for Bone and Mineral Research have consistently raised the need to expand the reimbursement standards. The number of osteoporotic fractures in Korea is increasing every year, but only 36% of patients receive medication for their osteoporosis within a year after suffering a fracture. Patients with osteoporosis gradually lose bone mass, and experience fractures in the spine, femur, wrist, etc. at the slightest impact. However, because osteoporosis has no symptoms, it is often not actively treated. In particular, the percentage of patients who continue treatment is low due to limited reimbursement standards. Dr. Byung Ho Lee, professor of Orthopedic Surgery at Gangnam Severance Hospital, said, "Studies have shown that osteoporosis increases the risk of new fractures fivefold within 1-2 years after a fracture. The mortality rate within 1 year of hip and spine fracture is 30% and 20%, respectively. It is imperative that ultra-high-risk patients that are at high risk of fracture receive the drug treatment." The changed reimbursement standards are expected to increase the utilization of osteoporosis medications such as Prolia (denosumab), Evenity (romosozumab), and bisphosphonates. Osteoporosis drugs are divided into bone stimulators (such as Evenity), which build the bone, and bone resorption inhibitors (such as Prolia and bisphosphonates), which inhibit the differentiation and action of osteoclasts. Dr.Lee said, "Sequential treatment with a bone stimulator inhibitor followed by a bone resorption inhibitor is more effective than vice versa. Therefore, It is important to continue the use of bone resorption inhibitors after bone stimulators in high-fracture-risk patients.” Dr. Bum Joon Kim, professor of Endocrinology at Seoul Asan Medical Center, said, "The longer the treatment is administered, the better the effectiveness is for osteoporosis and the lower the risk of fracture. The treatment goal should be a T-Score of -2.0 or higher, not -2.0, which is the current reimbursement standard. For Prolia, there is no clinical limit set on the treatment duration. The extended reimbursement has fostered the environment for long-term treatment, so it is important now for us to continue administering the drug.” Dr. Bum Joon Kim, professor of Endocrinology at Seoul Asan Medical Center
- Policy
- 'Approvals-Reimbursement Reviews-Price Negotiations' pilot
- by Lee, Hye-Kyung Jun 20, 2024 05:48am
- The government is preparing to commence “The 2nd Pilot Project for Integration of Product Approvals, Reimbursement Coverage Reviews, and Drug Price Negotiations” The pilot system is intended to concurrently process applications to the Ministry of Food and Drug Safety (MFDS), reimbursement assessment, and drug price negotiations. Following the first pilot program last year, the government initiated a demand survey to commence the second pilot program in the second half of the year. According to the industry sources on June 19th, the Ministry of Health and Welfare (MOHW)’s Pharmaceutical Benefits is conducting a demand survey for drugs to participate in the second approval-assessment-negotiations pilot program. This program aims to improve patient access to treatments for severe diseases and strengthen reimbursement management. “The 2nd Pilot Project for Integration of Product Approvals, Reimbursement Coverage Reviews, and Drug Price Negotiations” in preparation. The 'approval-assessment package system' is now in effect to strengthen patient access to reimbursable treatments. This system has been designed to handle the marketing approval from the MFDS and reimbursement appropriateness assessment of HIRA at the same time. By expediting the drug price negotiations stage, the goal is to shorten the time it takes for the entire process, ensuring prompt drug reimbursement. The drug can be applied to HIRA’s insurance listing after receiving marketing approval by passing the safety and efficacy review from the MFDS. The course of the process is that once a reimbursement appropriateness decision is made and selected as a drug price negotiation or reimbursable drug, the drug can be reimbursable. The approval-assessment-negotiation packages will handle all three tracks simultaneously. Drugs that are eligible for approval-assessment-negotiation packages must meet the following conditions. For a drug to be considered for the second pilot program, ▲The drug must be eligible for approval and decision application by the end of June next year. ▲It should be a drug intended for treating life-threatening diseases (with a life expectancy of less than 1 year) or rare diseases with sufficient efficacy. ▲The drug must demonstrate clinically significant improvements in efficacy compared to existing treatments or be for conditions without current treatments. ▲It must meet the prerequisites for designation under the MFDS's Expedited Review and Approval (GIFT) program or be eligible for application. Required documents must include the planned date of application for approval, product name, ingredients, classification, indication, approval alignment (domestic/foreign), drug pricing application system, life expectancy, 5-year survival rate, clinical stage, presence of placebo, reimbursement status in South Korea for placebo, evaluation criteria, substitute drug, current treatment, degree of improvement, and number of subjects. Additionally, the document must include the estimated per capita and overall estimated financial requirements, excluded country reimbursement evaluation results, number of countries where pricing is listed, names of countries where pricing is listed, and company name. This document will be used as a reference for selecting drugs for the pilot program. The registration deadline is August 12th, and the documents can be submitted to the Korea Pharmaceutical and Bio-Pharma Manufacturers Association (KPBMA). Meanwhile, two items of treatments for pediatric rare diseases have been designated for the first pilot system and are under assessment for approval, reimbursement assessment, and drug pricing negotiations simultaneously.
- Company
- HK inno.N and others license out jointly developed candidate
- by Kim, Jin-Gu Jun 20, 2024 05:48am
- 'IMB-101(OXTIMA),' a dual-antibody candidate jointly developed by HK inno. N, IMBiologics, and Y-Biologics, was licensed out to a U.S. biotech company specializing in new drug development. The contract amounts to US$940 million (approximately KRW 1.3 trillion), including an up-front payment of US$20 million (KRW 27.6 billion). HK inno. N announced on June 17th that it has entered into a technology transfer agreement with Navigator Medicines, a U.S. new drug development company. The contract covers global countries except for Asia (Japan included). According to the contract, HK inno. N will receive a proportional share of the total contract. The company will also receive a royalty payment from sales after the launch. 'IMB-101,' under joint development of three companies, is a dual-antibody candidate that targets both OX40L antibody and TNF-α. It regulates both inflammatory cytokines and T-cells, targeting autoimmune diseases. This candidate was secured through joint research of HK inno. N and Y-Biologics commenced in 2016. Subsequently, it was transferred to IMBiologics in August 2020. IMBiologics is a company established by people who worked at HK inno.N. IMBiologics obtained the U.S. Food and Drug Administration (FDA) approval to conduct Phase 1 trials for 'IMB-101' in August of last year and accomplished license out before the completion of clinical trials. IMBiologics was responsible for heading the license out. An official from HK inno. N said, "It is meaningful that a jointly developed pipeline by three domestic pharmaceutical and biotech companies has shown potential for entry into the U.S. market by leveraging synergy in their respective areas." They added, "This achievement holds substantial significance. We will continue to strive for accelerated and visible outcomes through active open innovation across various aspects." An official from Y-Biologics said, "We commend the accomplishments of our joint development partners." They added, "We will continue to demonstrate the excellence of our antibody discovery platform and strive to become a global leader in novel antibody drug development."
- Company
- K-pharma speeds up Keytruda biosimilar development...
- by Kim, Jin-Gu Jun 19, 2024 05:46am
- Product photo of Keytruda. Biopharmaceutical companies in South Korea are fast-developing biosimilars referencing 'Keytruda (pembrolizumab),' which has ranked no.1 in global sales. Samsung Bioepis and Celltrion have initiated global phase 3 trials. Due to Keytruda’s leading position in global sales, competition is expected among the companies mentioned above, as well as U.S.-based Amgen and Swiss Sandoz, to develop biosimilars. Pharmaceutical companies in Korea and overseas are initiating global phase 3 trials for 'Keytruda biosimilar' According to industry sources on June 17th, Celltrion recently submitted an IND to the U.S. Food and Drug Administration (FDA) for its 'CT-P51,' which is being developed as a biosimilar referencing Keytruda. Celltrion will conduct a comparative effectiveness study to demonstrate equivalence between Keytruda, the original pharmaceutical, and CT-P51 in 606 patients with non-small cell lung cancer (NSCLC). Previously, Samsung Bioepis initiated a global Phase 3 trial for Keytruda biosimilar, 'SB27,' in April. Samsung Bioepis plans to conduct a phase 3 trial comparing the effectiveness and safety of SB27 to Keytruda, enrolling 616 patients with metastatic NSCLC across 14 countries. Samsung Bioepis (left), Celltrion. The analysis shows that competition to develop Keytruda biosimilars among companies, including biopharmaceutical companies in South Korea, globally is on the rise. Currently, U.S.-based Amgen and Swiss-based Sandoz have commenced phase 3 global clinical trials to develop Keytruda biosimilars. Amgen commenced a phase 3 global clinical trial for ABP234 in April of last year, and Sandoz initiated a phase 3 clinical trial for GME751 the same month. Keytruda’s substance patent expires after 2029…biosimilar companies aim for 'agreement' with the original company Global companies are expected to complete their biosimilar development between 2025 and 2026. Keytruda’s substance patent will expire in November 2029 in the United States and in January 2031 in Europe. Other patents, such as the use patent, formulation patent, therapeutic method-related patent, and process-related patent, tied to indications are still valid. Since Keytruda has over 30 approved indications, more than tens of patents are tied to these. The original company, with an 'evergreening' strategy, has secured the patent validity of Keytruda until after 2040 through numerous patents. Since there are more than tens of patents to overcome, companies developing biosimilars aim to reach an 'agreement' with the original company rather than launching products after patent challenges. Previously, in the cases of global pharmaceuticals, such as Humira and Enbrel, companies developing biosimilars launched their products through agreements with the original company, either by paying royalties or adjusting release dates. For these reasons, pharmaceutical industry experts anticipate that the timing of completing clinical trials will be a crucial variable for biosimilar developers. Completing biosimilar development quickly can provide an advantageous position over competing firms in negotiations over royalty payments to original companies or adjustments to launch dates. Top 10 pharmaceuticals in global sales prospects for 2024 (source: Evaluate) According to the pharmaceutical market research firm Evaluate, Keytruda generated US$25 billion (approximately KRW 33 trillion) in global sales last year, becoming the top-selling pharmaceutical globally. Previously, the top-selling pharmaceuticals were Humira from AbbVie from 2019 to 2020, and Pfizer's COVID-19 vaccine Comirnaty from 2021 to 2022. Keytruda is rapidly expanding sales through actively adding indications. After reaching US$10 billion (approximately KRW 13.3 trillion) in 2019, it showed steady growth topping US$20 billion (approximately KRW 26.7 trillion) in 2022. To date, Keytruda has secured more than 40 indications. In the Korean market, Keytruda is also a leading pharmaceutical with the highest sales. According to the pharmaceutical market research firm IQVIA, Keytruda generated sales of KRW 398.7 billion last year, up 66% from KRW 239.6 billion in 2022.
- Company
- Suhee Shin appointed new General Manager of Amgen Korea
- by Eo, Yun-Ho Jun 19, 2024 05:46am
- Suhee Shin, new General Manager of Amgen Korea Suhee Shin, the former head of Novartis Korea, is coming back to head another Korean subsidiary of a multinational pharmaceutical company after two and a half years. According to industry sources, Director Suhee Shin, who had been leading the Healthcare Innovation Cluster at Roche Korea, has been appointed to take over as the General Manager of Amgen Korea following the retirement of the current GM, Sang-kyung Noh. Shin resigned in 2022 when Novartis Korea's specialty drug and anticancer business units were merged as one and the current president, Byung-Jae Yoo took over as head of the new combined Novartis Korea. Since then, Shin joined Roche in February 2023. She left Roche last week after accepting the General Manager role at Amgen Korea. Since joining Handok Pharmaceuticals in 1999, Shin and has held commercial business unit leadership roles in various chronic disease areas including diabetes at Sanofi Korea and AstraZeneca Korea. In 2018, Shin served as the Head of the Hematology Business Franchise of Novartis Oncology and was appointed as the General Manager of Novartis Oncology in 2019, where she led the successful launch and reimbursement of various innovative oncology pipelines. Shin graduated from Ewha Womans University College of Pharmacy and earned an MBA from New York University Stern School of Business.
- Company
- New multiple sclerosis drug Ocrevus is approved in Korea
- by Son, Hyung-Min Jun 19, 2024 05:46am
- Dr. Ho Jin Kim, Professor of Neurology, the National Cancer Center A new drug for multiple sclerosis (MS), an intractable disease characterized by a high relapse rate, has been introduced to the market. Roche's Ocrevus was approved in Korea for the treatment of relapsing-remitting MS as well as primary progressive MS, for which there had been no treatment options available. Medical experts have expressed the importance of starting treatment with a high-potency agent early in the disease to prevent relapses. On the 18th, Roche Korea held a press conference at the Lotte Hotel in Jung-gu, Seoul, to celebrate the approval of Ocrevus (ocrelizumab) as a treatment for multiple sclerosis in Korea. Ocrevus was approved in Korea on March 13 as an autoimmune disease treatment that targets CD20-expressing B cells that affect the demyelinating process that causes neurological disorders in MS patients. With the approval, Ocrevus is available for the treatment of Relapsing forms of MS, to include clinically isolated syndrome, relapsing-remitting disease, and active secondary progressive disease, in adults, and primary progressive MS, in adults. MS is a chronic disease in which myelin sheaths are damaged by an autoimmune inflammatory response. Damage to the myelin sheath causes symptoms such as muscle weakness, fatigue, and vision impairment, and can lead to non-traumatic neurological disability. As of 2022, an estimated 2,674 people in Korea are living with MS, with more than 62% of them in the 20-40 age group. Until now, antibody drugs such as Tysabri (natalizumab), Gilenya (fingolimod), and MabThera (rituximab) were used for the disease, but there had been a steady need for additional high-potency drugs. Various new drugs have been developed overseas, including Novartis' Kesimpta (ofatumumab) and TG Therapeutics' Briumvi (ublituximab), but Roche's Ocrevus is the only one introduced in Korea. Ocrevus also offers greater dosing convenience over Kesimpta (administered once a month), as it can be administered every 6 months. The approval was based on the Phase III OPERA-I and II trials. The trials evaluated the efficacy and safety of Ocrevus versus Biogen's interferon therapy Plegridy (peginterferon beta-1a) in patients with relapsing-remitting MS. In the trials, Ocrevus reduced the annualized relapse rate (ARR) by nearly half compared to Plegridy. Specifically, in the OPERA I trial, the ARR was 0.156 in the 96-week Ocrevus arm and 0.292 in the control arm, and in the OPERA II trial, the ARR was 0.155 in the 96-week Ocrevus arm and 0.290 in the control arm. Ocrevus also showed efficacy in the Phase III ORATIORIO trial that studied patients with primary progressive MS. In this study, Ocrevus reduced confirmed disability progression (CDP) by 24% over 12 weeks compared to the control arm. In terms of safety, the most common adverse events were infusion-related reactions (IRRs) and upper respiratory tract infections, most of which were mild to moderate in severity. Dr. Ho Jin Kim, Professor of Neurology at the National Cancer Center, said, "The unmet need for MS treatments remains high. In Korea, there is no opportunity to use high-potency drugs in the treatment of MS, and we have low access to such drugs. Overseas, high-potency drugs have been used as first-line treatment for MS since 2020. Ocrevus was approved overseas in 2017, but it took 7 years for it to be approved in Korea." He added, “In MS, even the smallest differences in its early stages can have enormous cumulative effects. This is why there are significant benefits to having early access to highly effective treatments. These treatments will not only improve the quality of life for the patients but will also help reduce socioeconomic burden. Ocrevus will be well utilized because it owns ample data on its efficacy as well as on long-term administration.”
- Company
- "Novotech is a global CRO partner for Korean biotech"
- by Lee, Tak-Sun Jun 19, 2024 05:46am
- Novotech is a global full-service clinical Contact Research Organization (CRO) focused on partnering with biotech companies to accelerate the development of innovative and novel therapies at every clinical phase. Recognized for its CRO industry-leading contributions, Novotech received numerous prestigious awards, including the CRO Leadership Award 2023, Best Cell & Gene Therapy CRO 2023, and Asia-Pacific Contract Research Organization Company of the Year Award 2023, since 2006. Novotech was founded in 1997 and provides comprehensive services, including a research center, phase 1 clinical trial facility, drug development consulting, and regulatory expertise. The company has experience in over 5000 clinical projects, including Phase 1 to Phase 4 clinical trials and bioequivalence tests. Furthermore, Novotech has 34 offices globally and has over 3000 staff. The company partners with over 1500 CRO firms, establishing itself as a partner with an end-to-end strategy. Commencing in Asia Pacific, which is one of the regions with the most complicated clinical trials, Novotech has strategically expanded its geological position with increased customer needs for global clinical trials. In 2008, Novotech opened a subsidiary in South Korea, one of the leading global countries in clinical trials. The decision was based on South Korea’s continuous investment in research and development, rapidly growing with the government support, and focusing on life sciences and biotechnology. In 2020, Novotech acquired PPC, which has subsidiaries in Taiwan, China, and South Korea. Through this acquisition, Novotech was able to fulfill the growing biotech needs, particularly in China. In 2022 and 2023, Novotech acquired NCGS (May 2022), EastHORN (November 2023), and CBR International (January 2023). The company entered the United States and European markets, strengthening its global position. Sanghee Kim (53), Korea Country Managing Director, is leading Novotech Korea, which is growing as a biotech hub. Kim has led the growth of PPC in South Korea through integration with Biosuntek Laboratory, which was one of the CROs in South Korea, and later PPC integrated with Novotech. "Previously, Novotech provided multinational clinical trial services, and PPC focused on phase 1 to phase 4 trials in South Korea and PMS. With the acquisition of Biosuntek, which specializes in bioequivalence tests and PK analysis, Novotech now offers the most comprehensive service among global and domestic CROs," Kim said. Sanghee Kim, Novotech Korea The Korea subsidiary of Novotech focuses on novel drug development consulting, protocol development, project management and clinical monitoring, pharmacovigilance, data management (DM), and statistical analysis. Furthermore, with people specializing in areas such as site management organization (SMO), the company can offer full-service for domestic and global clinical trials. "Most global CROs do not have people specializing in DM/statistical analysis and medical, Lab, and SMO in South Korea," Kim said. "Novotech Korea has advantages and can be differentiated from other countries, with a specialty workforce offering optimized comprehensive service to fulfill the needs of biotech and pharmaceutical companies in all phases, including the early and late phase clinical trials," Kim explained. After graduating from the College of Pharmacy at Chung-Ang University, Kim has been working in the pharmaceutical and CRO industry since 1994. She started her career in a pharmaceutical company in Korea, focusing on approval applications and academic training, and relocated to a multinational pharmaceutical company, taking on various roles related to clinical trials in the medical department. "While working in the pharmaceutical industry, I had interest in various businesses and took on the roles. I have gained valuable experiences working for 15 years in clinical trial planning and management, pharmacovigilance, and quality management," Kim said. As many pharmaceutcial companies considered clinical trial outsourcing as the key strategy in mid-2000, Kim beame interested in CRO and started her CRO career at PPC Korea with a passion for working in a new field. "PPC was a small company, less than a year since commencement. As the first country manager in the Korean subsidiary, I was involved in setting up the departments, and the company gradually grew into CRO with the full-service. In the beginning, colleagues and employers I met in my previous work helped in many ways, and it became a motivation. Afterward, I established a reputation from clients," Kim said. With a 30-year career in pharmaceuticals and CRO, Kim says fulfilling the needs of everyone involved in the business is a responsibility and an important task as a leader. "As a Country Managing Director, I value stakeholder management. Many leaders in the CRO industry value human resources management as a key task. I believe, like other service businesses, that CRO operations ultimately aim for balanced stakeholder management and management that contribute to better health outcomes for employees, customers, shareholders, local communities, and patients. If we can achieve this, it will be a win-win situation for everyone involved," Kim commented. Novotech has been making efforts to promote a lateral organization and corporate culture that respects and supports each member. As part of our ongoing efforts to establish this corporate culture, we are honored to be recognized as one of the top 100 companies to work for in South Korea in 2022 (Great Place To Work® Korea). In response to a question about the most memorable project, "Whether it's clinical trials for regulatory approval or post-market studies, all projects aim to generate the basis of efficacy, safety, and utility," Kim said, adding, "Once a project completes and receives market approval from regulatory authorities, receiving a letter of appreciation from the client is a memorable and fulfilling experience. However, because all projects are meaningful and important to our clients, it's difficult to single out just one project." "South Korea has excellent facilities and infrastructure in clinical trial institutions (hospitals) and outstanding researchers, creating an environment for active clinical research," Kim said. However, Kim also analyzed, "In recent years, the market has not seen significant growth, and competition has intensified with the entry of numerous global CROs both domestically and internationally." "Regulatory adjustments are necessary since the digital transformation of clinical trials has accelerated since COVID-19," Kim said. "Improving clinical trial regulations sometimes requires understanding and cooperation from multiple government agencies depending on the case, which hinders rapid regulatory improvements," Kim added. "We understand that the needs vary among biotech companies, large domestic pharmaceutical companies, small to medium-sized pharmaceutical companies, and multinational companies. Accordingly, we aim to be a trusted partner in every stage, from consulting on development strategies, depending on whether our clients' R&D goals are focused on obtaining domestic market approval, licensing out after initial clinical results, or conducting clinical trials for global market entry and subsequent market approvals in multiple countries," Kim concluded.
- Company
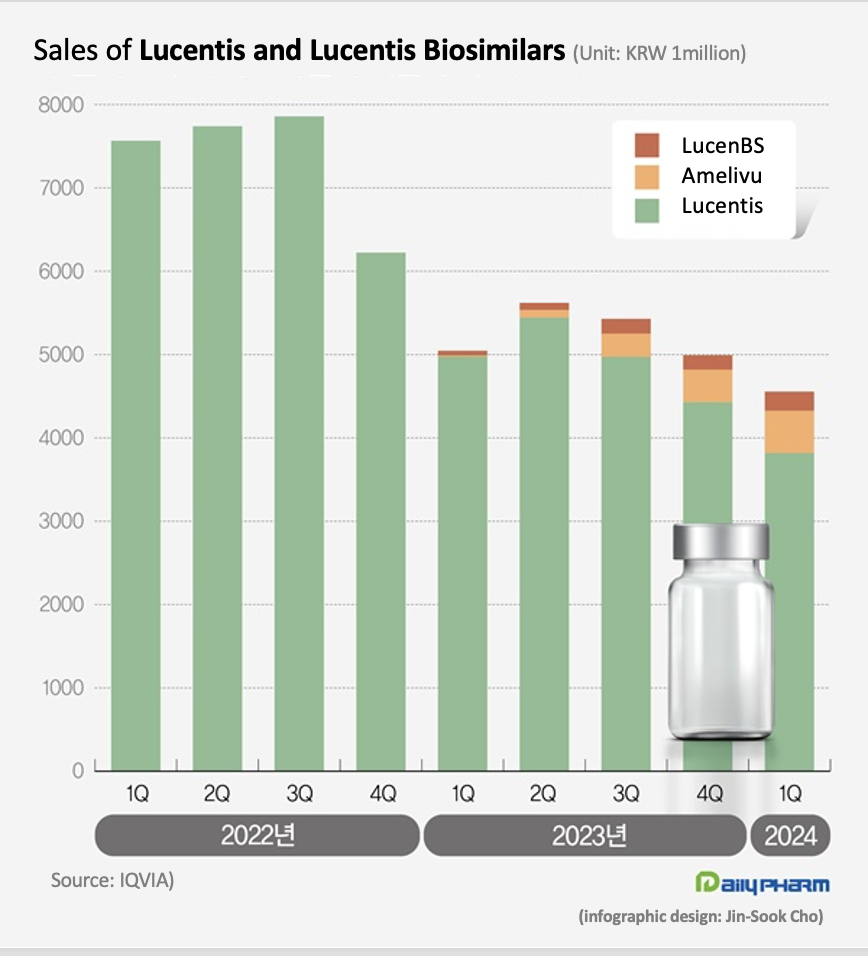
- Lucentis biosimilars occupy 16% of mkt in 1 year
- by Chon, Seung-Hyun Jun 19, 2024 05:46am
- The market size for the eye disease drug Lucentis has shrunk significantly. Last year, its biosimilars entered the market and reduced the drug price of Lucentis, reducing the market size. Although the market share of the two biosimilars remains a mere 16%, the price reduction of Lucentis saved more than KRW 10 billion in annual health insurance finances. According to drug research institution IQVIA, the market size of ranibizumab in Q1 was KRW 4.6 billion, down 9.7% YoY. Ranibizumab is the active ingredient contained in Lucentis. Lucentis, which is marketed by Roche and Novartis, is a drug used to treat eye diseases such as macular degeneration and diabetic macular edema. It is indicated for the treatment of ▲neovascular (wet) age-related macular degeneration, ▲diabetic macular edema, ▲proliferative diabetic retinopathy, ▲ vision impairment due to macular edema following retinal vein occlusion, ▲and vision impairment due to choroidal neovascularization. The ranibizumab recorded KRW 7.6 billion in sales in Q1 2022, down 33.3% from KRW 5 billion in Q1 last year. The market size for Lucentis shrank due to the drug price cut that followed the entry of its biosimilars. Samsung Bioepis and Chong Kun Dang received approvals for their Lucentis biosimilar products. Samsung Bioepis received approval for its Lucentis biosimilar Amelivu in May 2022, and Chong Kun Dang received approval for its LucenBS in October 2022. Amelivu and LucenBS have been reimbursed since January last year. The insurance price ceiling of Lucentis has been cut by 30% since February last year. The price of Lucentis 10mg (2.3mg/0.23mL) had fallen 30% from KRW 828,166 to KRW 579,716. The price of Lucentis Prefilled Syringe (KRW 826,231→KRW 578,362) also fell 30%. As a result, sales of Lucentis in Q1 were 3.8 billion won, down 23.3% YoY. Compared to Q1 2021, which was before the price cut, the company's sales have fallen by 49.5% in 2 years. While domestically developed biosimilar versions of Lucentis are working to accelerate market penetration, their current share in the market is less significant. In Q1, Amelivu sold KRW 500 million. Since its sales exceeded KRW 100 million in Q3 last year, its sales scale has gradually expanded, but its gap with the original drug is still large. Amelivu’s market share in Q1 was 11.1%. LucenBS’s Q1 sales were KRW 200 million, accounting for only 5.0% of the total market. The two biosimilars combined occupied 16.2% of the market, falling far behind Lucentis’s share. However, Amelivu and LucenBS’s supply at a relatively low price in the market is said to have significantly contributed to reducing the cost of medication for patients. The insurance ceiling price of Amelivu 10mg/ml is KRW 350,000, which is only at a 60.4% level of Lucentis’ price. Compared to the price of Lucentis before the price cut, it costs 42.3% of Lucentis’ previous price. The insurance price of LucenBS is KRW 150,000, which is 74.1% lower than Lucentis. This is more than 80% lower than the price of Lucentis before the biosimilar was launched. Initially, Chong Kun Dang listed LucenBS at an insurance price of KRW 300,000, then further reduced the price by 50% this year. In Q1, the Lucentis market shrank by 40.0% compared to 2 years ago. However, considering the drug price cut and the market entry of cheaper biosimilars, their usage has not decreased. The emergence of domestically developed biosimilars has resulted in annual health insurance savings of more than KRW 10 billion.
- Company
- Targeted therapies for HER2m NSCLC actively developed
- by Son, Hyung-Min Jun 18, 2024 05:49am
- The domestic and foreign pharmaceutical industry has taken up the challenge of developing a new drug for HER2-positive NSCLC. After Enhertu opened the door by obtaining the first marketing authorization as an anticancer drug targeting the HER2 mutation in Korea, many later entrants such as Yuhan Corp, Boehringer Ingelheim, and Hanmi Pharmaceutical have also started clinical trials. Until now, there have been a number of drugs targeting various gene mutations such as EGFR, ALK, ROS1, BRAF, MET, and RET in NSCLC, but none has targeted HER2. Approximately 2-4% of patients with NSCLC have a HER2 mutation. Due to its low prevalence, the companies had difficulty developing targeted therapies. This is why the clinical results of the latecomers are gaining interest. Boehringer Ingelheim disclosed early phase clinical trial results confirming the efficacy of its HER2-targeted antitumor candidate, and Yuhan Corp secured multinational IND approval for its HER2-mutation targeted antitumor drug candidate after Leclaza. Hanmi Pharmaceuticals also launched a new HER2-targeted NSCLC drug after failing with poziotinib. According to industry sources on the 18th, Boehringer Ingelheim's zongertinib (Development code name: BI-1810631) showed an effect in HER2-positive NSCLC. Zongertinib is a tyrosine kinase inhibitor (TKI) that binds to the HER2 mutation without inhibiting the wild-type EGFR. The Phase 1 trial, named BEAMION-Lung01, evaluated the efficacy of zongertinib in 36 patients with metastatic/advanced NSCLC who were refractory to standard of care and had HER2 mutations. The study was designed to determine if zongertinib can slow the progression of advanced NSCLC compared to the current standard of care, Keytruda plus platinum-based chemotherapy. The primary endpoint was set as an investigator-assessed overall response rate (ORR). Trial results as of July 31, 2023, showed that the ORR was 58% with zongertinib with a disease control rate (DCR) of 97%. In terms of safety, the most common treatment-related adverse events (TRAEs) were diarrhea and rash. Based on the tolerability and safety of the drug demonstrated in the Phase 1 trial, Boehringer Ingelheim plans to conduct a full efficacy evaluation of zongertinib through the Phase 2 trial. Korean companies including Hanmi and Yuhan also start developing treatments for HER2 NSCLC Yanghwa has also jumped into the development of HER2-targeted anticancer drugs. The company plans to develop a new drug for NSCLC to add on to its EGFR (HER1)-targeting anticancer drug Leclaza. The company’s candidate, YH42946, targets NSCLC patients with EGFR exon 20 mutations along with HER2 positivity. YH42946 was approved by the U.S. Food and Drug Administration (FDA) last month and was then granted to start a multinational Phase I/II clinical trial in Korea in the middle of this month. The company acquired the new anticancer drug candidate and its pipeline last year from a local biotech J Ints Bio. The Phase I/II trial initiated this time is the first trial evaluating the tolerability and safety of YH4294 in humans. In preclinical studies, YH42946 has shown anti-tumor effects against HER2 mutations and EGFR exon 20. It has also shown an effect on solid tumors such as breast and colorectal cancers. Hanmi Pharmaceutical is also out to develop new treatments after the failure of poziotinib. Its new anticancer pipeline, the ‘selective HER2 Exon20 insertion mutation inhibitor', which had not been disclosed until now, was found to have an anti-cancer effect based on its strong activity against HER2 exon20 insertion mutation and high selectivity for EGFR and has been confirmed to be a viable treatment for NSCLC. The company has a history of developing an oral treatment for HER2-mutant NSCLC. Hanmi Pharmaceutical and its U.S. partner Spectrum (now Assertio) developed poziotinib for locally advanced or metastatic NSCLC with HER2 exon 20 insertion mutations but ultimately failed to gain FDA approval. In 2022, the U.S. Oncologic Drugs Advisory Committee (ODAC) voted (9:4) that the benefits of poziotinib did not outweigh the risks, prior to the FDA's decision on whether to grant it marketing authorization. At the time, the ODAC noted that poziotinib lacks efficacy compared to Enhertu, which also targets HER2. Currently, the only targeted therapy option available for HER2-mutant NSCLC is Enhertu, developed by Daiichi Sankyo and AstraZeneca. On March 20, Enhertu’s indication was extended to the treatment of patients with unresectable or metastatic NSCLC whose tumors harbor an activating HER2 (ERBB2) mutation and who have received prior systemic therapy, including platinum-based chemotherapy. In the DESTINY-Lung02 study, Enhertu achieved a confirmed objective response rate (ORR) of 49%, complete response (CR) of 1%, and partial response (PR) of 48% as assessed by an independent centralized blinded review (BICR). Poziotinib achieved an ORR of 28% in the ZENITH20 cohort 2 study. Following the failure to receive approval, Spectrum deprioritized the development of poziotinib and reduced its R&D workforce by 75%. Therefore, it will be interesting to see if Hanmi Pharmaceutical’s newly developed HER2-targeted cancer drug will be able to go on further and receive approval.
- Policy
- "People do not recognize generic equivalence"…
- by Lee, Hye-Kyung Jun 18, 2024 05:48am
- "80% of the medicines approved in Korea are generics, which account for 53% of medical expenses. However, consumer perception of generics’ equivalence to original medicines remains at 50%. The Ministry of Food and Drug Safety (MFDS) should be concerned and ashamed of this outcome." Lee Eui-Kyung, a professor at the School of Pharmacy at Sungkyunkwan University who served previously as the Minister to the Ministry of Food and Drug Safety (MFDS), pointed out that stifling generic competition limits patient access to medicines. Lee Eui-Kyung, a professor at the School of Pharmacy at Sungkyunkwan University.Lee delivered a speech at the plenary session on the topic of 'Regulatory Science Innovation and Patient Access to Medicines' at the Korean Society of Food, Drug & Cosmetic Regulatory Sciences (KFDC)’s spring academic conference on June 14th. Lee said factors contributing to patient access to medicines could include ▲delays in pharmaceutical entry ▲stifling generic competition ▲a short supply of pharmaceuticals. Lee is particularly disappointed that several experts are voicing the differences in product qualities and people’s perceptions of generic and original medicines. "I wish people would recognize the equivalence of generics that have demonstrated equivalence through bioequivalence tests, and doctors prescribing also recognize them," Lee said. "Half of the people in Korea feel difference of generics in cultural and societal aspects is stifling patient access to medicines," she added. According to a survey presented at the conference (document prepared by researcher Park Hye-Kyung), around 50.9% answered ‘YES’ to the question, 'Do you think the effectiveness of generics is equivalent to original medicines?' "Arguments about the quality difference between originals and generics hinder improvements to the system, such as drug substitution preparation and drug pricing," Lee said. "The U.S. FDA is putting efforts into resolving arguments related to inequivalence by marketing generic equivalence. I tried to solve this problem during my tenure as the MFDS director but could not due to the COVID-19 pandemic,” Lee expressed concerns. Furthermore, Lee suggested that the MFDS should provide regulatory support for medicines with patent expired that do not yet have generics developed. According to the MFDS documents in October 2022, 476 of 1004 products with expired patents do not have generics available. For instance, Celltrion Pharm’s 'Godex Cap,' with annual production sales of approximately KRW 73 billion, is reimbursable, but the 53.55% price reduction has not been applied due to the absence of generics. "For Godex, having made of seven ingredient composition, complex generic development is difficult," Lee said. "The FDA established a 'research center for complex generics' to facilitate complex generics market entry and communications and information sharing among the government, academics, and pharmaceutical companies." Therefore, it is argued that if the Korean government also prepares solutions for developing complex generics, the prices of drugs with expired patents could be reduced, leading to savings in insurance finances. Lee delivered a speech at the plenary session on the topic of Lee expressed disappointment towards the conditional approval system and expedited review system introduced and implemented by the MFDS to address patient accessibility issues caused by delays in drug approval. "Expedited reviews and conditional approvals shorten the review period for new drugs, which is positive for early treatment access for severely ill patients. However, proceeding with conditional approval while clinical trials are not fully completed has increased uncertainty regarding the evidence," Lee said. From 2012 to 2021, the MFDS gave conditional approvals for 35 products. Among these, 15 products did not submit clinical data, siz had their approvals revoked, and eight had their Phase 3 clinical trial report submissions delayed. Only seven products, approximately 20%, submitted regular reports as required. "Out of all products with conditional approval, ten are new drugs developed in South Korea. Among these, eight items had not submitted clinical documents," said Lee. "Two products, 'tertomotide generic' and 'Olita,' have had their approvals withdrawn," she stated. "The MFDS is responsible for making the initial decision on new drugs in Korea, but the basis for the approval should not be influenced by conditional approvals," Lee said. "Efforts should be made to secure the workforce for reviewing regulatory standards and meeting requirements from the start of R&D,” LEE emphasized.