- LOGIN
- MemberShip
- 2026-04-03 12:18:27
- Company
- K-BIO expands its presence at the international convention
- by Son, Hyung Min Jun 23, 2025 06:01am
- Korean pharmaceutical and biotech companies showed their presence at the BIO International Convention 2025 (BIO USA 2025), the world's largest biotech business event. Major domestic pharmaceutical and biotech firms from South Korea attended the BIO USA 2025, held in Boston, USA, from June 16 to 19, showcasing their new drug pipelines and Contract Development and Manufacturing Organization (CDMO) technological capabilities. According to the Korea BIO on June 21, over 20,000 participants from 70 countries attended this year's BIO USA. Among them, the number of Korean attendees exceeded 1,300, marking the third consecutive year that South Korea has been the largest participating country from overseas. BIO USA is the world's largest pharmaceutical and bio exhibition, serving as a platform for global pharmaceutical and biotech companies and research institutions to explore opportunities for new drug pipelines, technology transfer, and collaborative research. Over 300 Korean companies participated in this year's event. Samsung Biologics expressed its commitment to expanding collaborations with global pharmaceutical companies through this event. Samsung Biologics plans to increase its production capacity by securing drug manufacturing contracts from pharmaceutical companies ranked among the top 20 to top 40 globally. Samsung Biologics has signed a total of 5 new contracts based on public disclosures this year alone. Starting with a $1.41 billion (approximately KRW 2 trillion) contract signed with a European pharmaceutical company in January, the company continued to secure new orders globally, including those from the U.S., Asia, and Europe. Samsung Biologics currently holds 17 out of the top 20 global pharmaceutical companies as clients. Through core competencies based on overwhelming production capacity, quality, and numerous track records, its cumulative total orders since its establishment have exceeded approximately $18.2 billion. Lotte Biologics announced the securing of new contracts through BIO USA. The company held a Contract Manufacturing Organization (CMO) agreement signing ceremony for antibody drugs with the British biopharmaceutical company Ottimo Pharma. This ceremony took place at the Lotte Biologics booth at the Boston Convention & Exhibition Center in the United States. Lotte Biologics announced the securing of new contracts through BIO USA Through this agreement, Lotte Biologics will produce the drug substance (DS) for Ottimo Pharma's new antibody drug, 'Jankistomig,' at its biotech campus in Syracuse, New York. Ottimo Pharma is a company developing a new drug with a PD1/VEGFR2 bispecific antibody mechanism, aiming to extend the lives of patients with cancer. Established in 2020, it has offices in the UK. Lotte Biologics offers CDMO services at the Syracuse biotech campus, including drug cell line development and large-scale contract manufacturing. Furthermore, it aims to operate Plant 1 within its Songdo Bio Campus starting in 2027. Plant 1 is a large-scale biopharmaceutical manufacturing facility with a production capacity of 120,000 liters, enabling it to secure significant global contracts. Celltrion held over 150 meetings at this event, discussing various collaboration strategies with global pharmaceutical and bio-companies. Notably, beyond CDMO and biosimilars, the company showcased various potential partnership opportunities for its pipelines under development, including antibody-drug conjugates (ADCs), multispecific antibodies, novel antibodies, and peptide new drugs. Celltrion also discussed open innovation aimed at finding promising technologies related to new drug development. Celltrion plans to thoroughly review the meetings held at this BIO USA to identify potential collaborators with growth potential and capabilities. Celltrion is pursuing the development of new ADC drugs. Earlier this year, Celltrion disclosed the preclinical results of its ADC candidate 'CT-P71'. CT-P71 utilized the ADC platform of the Korean ADC development company Pinotbio. CT-P71 is an ADC therapeutic agent under development targeting general solid tumors, including bladder cancer. It targets Nectin-4, a cell surface protein overexpressed in various solid tumors such as urothelial carcinoma and breast cancer. Celltrion also received approval for a Phase 1 clinical trial of CT-P70. CT-P70 is an ADC therapeutic agent targeting solid tumors such as non-small cell lung cancer, specifically targeting 'c-MET,' which, when activated in cancer cells, induces tumor growth. Korean companies promoted R&D competitiveness for new drug development This year, 51 companies participated in the Korea Section, operated by the Korea Bio Association, introducing technologies and pipelines across the entire biotech industry, including contract manufacturing, clinical services, materials/components/equipment business, new drug development, and platforms. Over 450 consultations were held throughout the exhibition hall. Notably, 24 pre-registered companies garnered attention from global partners through technology presentations at the Open Stage within the Korea Section. This year, both the number of participating companies and the exhibition space expanded compared to the previous year. A special area for materials, components, and equipment business was also operated separately, showcasing the competitiveness of Korea's biotech industry supply chain. Photo of BIO USA 2025 Korea Section (source=Korea BIO organization) In this event, Korean companies also focused on promoting their competitiveness in new drug development. Through BIO USA, Aptamer Sciences actively discussed strategic collaborations with major ADC-specialized companies in North America, Europe, and China, exploring concrete cooperation opportunities such as joint development, clinical collaboration, expansion into new indications, and technology transfer. Aptamer Sciences has proprietary ADC platform technology, ApDC (Aptamer Drug Conjugate). ApDC is a next-generation precision drug delivery platform that utilizes aptamers instead of antibodies, using an in-house modified nucleic acid technology. According to Aptamer Sciences, anti-cancer drugs developed using the ApDC platform have demonstrated various advantages in comparative experiments with ADC anti-cancer drugs, including rapid drug action through quick internalization into target cells after surface binding, excellent permeability into tumor tissue, rapid targeting after administration in animal models, and consequently, superior anti-tumor efficacy. Currently, Aptamer Sciences is expanding its platform to allow conjugation with various mechanisms of action beyond cytotoxic drugs, including radioisotopes, targeted protein degraders (TPDs), and immunostimulants. GI Innovation introduced its new pipelines and global business strategy as its next growth engines. GI Innovation unveiled its GI-128, which utilizes macrophages (a next-generation target gaining attention in the immunotherapy field), along with a trispecific pipeline that aims to surpass the rapidly emerging aPD-(L)1/VEGF bispecific antibodies in the global market. GI Innovation's newly introduced pipeline features a trispecific antibody structure that fuses a self-discovered aPD-L1 antibody with a VEGF antibody and a macrophage engager. It is evaluated as having a differentiated mechanism of action by overcoming the limitations of bispecific antibodies and activating tumor-immune responses. SK Biopharmaceuticals is engaging in artificial intelligence (AI)-driven drug discovery through a business agreement with PhnyX Lab. Through this agreement, the two companies plan to jointly develop customized solutions based on PhnyX Lab's generative AI solution 'Cheiron', automating tasks such as literature search, data analysis, and document creation required in the new drug development process. The agreement signing ceremony took place at the SK Biopharmaceuticals exhibition booth. (from left) Changho Yu, SK Pharmaceuticals VP/Chief Strategy Officer & Head of Strategy Division and Minseok Bae, CEO of PhnyX Lab Notably, SK Biopharmaceuticals plans to accelerate its 'AI Transformation' of the new drug development process, primarily focusing on automating tasks such as preparing regulatory documents required at the clinical entry stage, thereby advancing it with the use of AI. Through this, SK Biopharmaceuticals aims to maximize R&D productivity and significantly reduce the time and cost associated with development and approval. Samjin Pharmaceutical, making its first official corporate presentation at this year's BIO USA, showcased its competitiveness in developing new anti-cancer drugs, including ADCs. Currently, the company is developing various candidates, including ▲solid tumor therapeutic candidates 'SJN301' and 'SJN309' ▲antibody-drug conjugate (ADC) projects 'SJA20' and 'SJA70' ▲immune/inflammatory disease therapeutic candidate 'SJN314'.
- Policy
- Handok and JW’s new imported drugs reimbursed from July
- by Lee, Tak-Sun Jun 23, 2025 06:00am
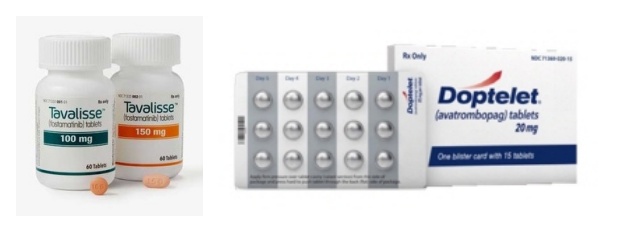
- Tavalisse (JW Pharmaceutical) and Doptelet (Handok) will both be reimbursed for ITP from next month In July, four new drugs, including an oral drug for paroxysmal nocturnal hemoglobinuria (PNH), a new biological agent for severe atopic dermatitis, and a new drug for immune thrombocytopenia (ITP), will be reimbursed by health insurance and be available with coverage for patients. On the 19th, the MOHW announced the establishment of reimbursement standards for four new drugs, including Fabhalta Cap 200 mg (Iptacopan hydrochloride monohydrate, Novartis Korea), a new drug for the treatment of PNH. The reimbursement will take effect on the 1st of next month. In addition to Fabhalta Cap 200 mg, a treatment for severe atopic dermatitis, Ebglyss Autoinjector 250 mg (lebrikizumab-lbkz, Lilly Korea), ‘Doptelet Tab 20mg (avatrombopag maleate, Handok),’ and ‘Tavalisse Tab 100·150mg (fostamatinib sodium hydrate, JW Pharmaceutical).’ Fabhalta Cap 200 mg is an oral treatment for paroxysmal nocturnal hemoglobinuria and is expected to be more convenient than the injectable drugs that have been used until now. In addition, its hemolysis control effect is expected to be better than existing C5 inhibitors (Soliris and Ultomiris). PNH is a rare condition that affects about 1.5 people per 1 million worldwide. Until now, Soliris (eculizumab) and Ultomiris (ravulizumab) have been the main C5 inhibitors used for PNH. In November last year, Empaveli (pegcetacoplan, Handok), a subcutaneous injection that binds to C3 and C3b to inhibit the complement cascade, was also approved for reimbursement. The reimbursement of the new oral drug Fabhalta is expected to improve access to treatment and offer better therapeutic effects. Ebglyss Autoinjector 250 mg is reimbursed for adult (18 years of age or older) and adolescent (12 to 17 years of age, weighing 40 kg or more) patients with chronic severe atopic dermatitis whose symptoms have persisted for three years or more. This drug is the third biological agent for atopic dermatitis, following Dupixent (dupilumab) and Adtralza (tralokinumab). Ebglyss has demonstrated clinical efficacy and safety profiles through a Phase III clinical trial and is expected to become a first-line treatment option for atopic dermatitis patients in Korea. Doptelet Tab and Tavalisse Tab will be reimbursed for the treatment of adult chronic immune thrombocytopenia (ITP) that is unresponsive to corticosteroids and immunoglobulin. ITP is an autoimmune disease in which the immune system mistakes platelets for viruses and attacks them, causing platelet counts to fall below normal levels and increasing the risk of bleeding. As a result, patients may experience easy bruising and frequent bleeding, which in severe cases can lead to cerebral hemorrhage or gastrointestinal bleeding. According to the ITP Clinical Practice Guidelines issued by the Korean Society of Hematology, steroids and immunoglobulins are recommended as first-line treatments, while splenectomy or thrombopoietin-receptor agonists (TPO-RA) are recommended as second-line treatments for chronic ITP patients. With rare disease drugs imported by domestic pharmaceutical companies such as Handok and JW Pharmaceutical now reimbursed, industry eyes are on how the drugs will be received in the market.
- Company
- "6-in-1 vaccine Hexaxim may enhance preventive effect of NIP
- by Whang, byung-woo Jun 23, 2025 06:00am
- "Hexaxim is Korea's first hexavalent vaccine. It is expected to play a crucial role in helping protect children's health." Following the inclusion of Hexaxim, a hexavalent (6-in-1) DTaP vaccine, in the National Immunization Program (NIP) this year, the medical field is holding high hopes for increased convenience of immunization and improvement in vaccination rates. The analysis is that since immunization through NIP has already been conducted, the field is already experiencing practical benefits, such as a reduced number of immunizations. It is believed that, in the long term, Hexaxim will lessen the burden of hospital visits for caretakers, alleviate the stress of infant injections, and prevent the skipping of immunizations. Dr. Byung Wook Eun, Professor of Department of Pediatrics at Nowon Eulji Medical CenterDaily Pharm met with Dr. Byung Wook Eun, a professor at Nowon Eulji Medical Center, and listened to the background of the introduction of Hexaxim and its potential effects. Hexaxim is Korea's first and only fully liquid hexavalent fully liquid formulation vaccine, preventing six diseases, including diphtheria, tetanus, pertussis (DTaP), inactivated polio vaccine (IPV), Haemophilus influenzae type b (Hib), and hepatitis B (HepB), with a single injection. As of January 2, it has been officially introduced into the NIP, allowing the previous separate administration of the pentavalent (5-in-1) vaccine (DTaP-IPV-Hib) and the monovalent Hepatitis B vaccine to now be given in a single shot. According to Dr. Eun, since the introduction of Hexaxim into the NIP, there has been an increase in inquiries regarding new vaccination schedules and methods in actual clinical settings. Dr. Eun said, "With the introduction of the hexavalent vaccine, the vaccination schedule differs from the existing pentavalent vaccine, leading to many questions from both guardians and medical staff regarding vaccination criteria, interchangeability, and delayed vaccinations." Hexaxim is already a proven vaccine overseas, having received its first approval in Europe in 2013. It is now used in over 120 countries worldwide and is recommended as a mandatory vaccination in more than 40 countries, including Europe, Canada, and Australia. Dr. Eun explained, "The immunogenicity and safety of Hexaxim against all six infectious diseases through global clinical studies, including those conducted in Korea," and added, "In Korea, non-inferiority related to immunogenicity was confirmed through a clinical trial comparing the Hexaxim vaccination group with the group receiving the existing pentavalent DTaP combination vaccine concurrently with the monovalent Hepatitis B vaccine." Fewer injections due to schedule changes help improve convenience The introduction of Hexaxim has brought significant changes to the infant vaccination schedule. Previously, infants needed to receive the Hepatitis B vaccine at 0, 1, and 6 months of age and the pentavalent DTaP vaccine at 2, 4, and 6 months. However, starting this year, the schedule has changed. After the first Hepatitis B vaccination immediately after birth, infants will now receive Hexaxim at 2, 4, and 6 months, with no additional vaccination at 1 month. Dr. Eun stressed that "The introduction of Hexaxim reduces the total number of vaccinations by two, bringing the total to four injections." He added, "The hexavalent DTaP vaccine can administer six antigens at once, which can help improve vaccination rates compared to administering individual vaccines separately." However, as with any new vaccine introduction, there's some initial confusion in the field. Dr. Eun explained that there have been inquiries regarding the switching to the hexavalent vaccine at 6 months if the infant has already received the pentavalent combination vaccine at 2 or 4 months. The Korea Disease Control and Prevention Agency (KDCA) is addressing this confusion with clear guidelines. Dr. Eun stressed, "According to KDCA's official guidelines, DTaP-containing vaccines vary by manufacturer. Therefore, for the primary 3-dose series, it is recommended to administer vaccines from the same manufacturer consistently." Dr. Eun also said, "However, since most newborns are currently starting their vaccinations with Hexaxim, inquiries about interchangeability will gradually decrease in the future," and added, "There are also questions about vaccination age and intervals. Hexaxim's recommended vaccination schedule is at 2, 4, and 6 months of age (8-week intervals), with the recommended age for the first dose being 8 weeks (2 months of age)." However, in unavoidable circumstances, the first dose can be administered as early as 6 weeks of age. While a 2-month (8-week) interval is generally recommended, the vaccination schedule can be adjusted to a minimum of 4-week intervals. For example, if the first dose was given at 3 months of age, the second dose can be given 4 weeks later. Dr. Eun stated, "If there are any changes to the vaccination schedule, it is crucial to consult with a healthcare professional to get guidance on the timing and vaccine selection." There are, however, exceptional cases where Hexaxim cannot be administered. For instance, newborns born to mothers who are positive for the Hepatitis B virus must receive Hepatitis B immunoglobulin and the Hepatitis B vaccine within 12 hours of birth. These high-risk infants also require additional Hepatitis B vaccine doses at 1, 2, and 6 months of age, thus excluding them from the Hexaxim program. Furthermore, infants who have already completed their second Hepatitis B vaccination by 1 month of age cannot switch to Hexaxim and must continue their remaining vaccinations with the existing combination of the pentavalent vaccine and the Hepatitis B vaccine. "Hexaxim with increased preventive effects... high hopes for increasing vaccination rates" Dr. Eun stated that concerns about Hepatitis B antibody formation, which were previously raised by some, have been addressed through research. In the previous schedule, Hepatitis B vaccine was administered at 0 and 1 months of age. However, with the Hexaxim schedule, the 1-month vaccination is omitted, changing the schedule to 0-2-4~6 months. Regarding this, Dr. Eun responded, "The 0-2-4~6 month Hepatitis B vaccination schedule using Hexaxim showed immunogenicity similar to the existing 'pentavalent vaccine+Hepatitis B vaccine' schedule," and added, "Although the hexavalent vaccine includes a Hepatitis B component in addition to the existing pentavalent combination vaccine, its safety profile was confirmed to be similar to separate administrations." One of the anticipated effects of including Hexaxim in the NIP is an improvement in vaccination rates. Dr. Eun said, "Because a hexavalent vaccine can introduce six antigens in one shot, it can help improve vaccination rates compared to administering individual vaccines separately," and added, "Currently, infant primary vaccination rates exceed 90%, but we expect to push this figure higher with Hexaxim's introduction." As mentioned earlier, the reduced number of vaccinations helps prevent delayed vaccinations, which in turn can lead to a higher 'right-time vaccination rate,' thereby completing vaccinations at the recommended period, thus improving overall vaccination rates. Indeed, improvements in vaccination rates have been observed in other countries after the introduction of hexavalent combination vaccines. In Australia, after the hexavalent vaccine was included in their NIP, the vaccination rate for infants aged 12 months increased from 84.9% in 2009 to 92.6% in 2018. Lastly, Dr. Eun added, "Misinformation about vaccines can lead to a drop in vaccination rates, and previously well-managed infectious diseases could potentially re-emerge," and urged, "We hope the public would utilize the NIP to help protect children's health."
- Policy
- Rapid adjustment of insurance prices for rare drugs granted
- by Lee, Hye-Kyung Jun 20, 2025 06:08am
- Verorab (pictured above), for which a price adjustment has been completed in response to exchange rate fluctuations, and Ivexproglycem (pictured below) for which a price adjustment application is currently under negotiations. The insurance price ceiling adjustment term for insured drugs supplied by the Korea Orphan Drug Center (KOEDC) is expected to be significantly reduced from the initial 8-9 months to around 4 months. Previously, it took at least 8-9 months to adjust the price cap, raising concerns about supply disruptions and financial losses for the center, so the government decided to take proactive measures to resolve the issue by significantly simplifying the price adjustment process for urgently needed drugs. During a meeting with journalists from the Ministry of Food and Drug Safety’s press corps on the 17th, the KOEDC said that it is operating a consultation system to promptly adjust reimbursement price ceilings for publicly procured orphan drugs in order to ease the supply burden caused by sharp exchange rate fluctuations. The KOEDC added that it adjusted the insurance price ceiling for Verorab through the system in January. The insurance price of Verorab was KRW 63,000 before the adjustment, but after the adjustment, it was raised by 65.9% to 104,887 won. According to the center, most orphan drugs are highly dependent on overseas imports, and import prices are sensitive to exchange rate fluctuations. However, the reimbursement ceiling was fixed, so there was a structural problem where the center had to continue supplying the drugs at a loss when the exchange rate rose sharply. According to the center, the exchange rate has risen by about 20% in the last three years, and in the case of some items, the KOEDC incurred losses of more than KRW 100 million per case. This has directly impacted patients' access to treatment. When the center delays or suspends supply due to budget constraints, patients experience treatment gaps because there are no domestic alternatives for orphan drugs. As a result, patient groups and relevant experts have consistently raised the need for system improvements. Kim Ki-young, Director of KOEDC, explained, “There has been around a 20% fluctuation in exchange rates over the past 3 years. For orphan drugs distributed in the market based on the reimbursement price ceiling, the increased costs have led to losses exceeding KRW 100 million per drug. In practice, the total budget for drug purchases has decreased, which has also caused disruptions in the supply of subsequent orphan drugs.” In response, the center established an exceptional price adjustment procedure in collaboration with the Ministry of Health and Welfare, the Ministry of Food and Drug Safety, the Health Insurance Review and Assessment Service (HIRA), and the National Health Insurance Service (NHIS). This streamlined process applies exclusively to publicly procured items that meet specific criteria. It significantly shortens the price ceiling adjustment period from several months to within 10 days, thereby minimizing supply disruptions and ensuring continuity of patient care. Notable examples of the expedited adjustment procedure include Verorab, which was adjusted in January this year, and Ivexproglycem, which is currently undergoing price adjustment. Kim said, “Previously, adjustments to the reimbursement price ceiling took eight to nine months due to various procedures, which inevitably resulted in losses for the center. The MFDS requested cooperation from the MOHW to establish a procedure to correct supply instability so that adjustments can be made quickly in response to exchange rate fluctuations.” Just like with exchange rate increases, price adjustments are also promptly made in the event of a decrease. Director Kim said, “If an exchange rate drop results in a surplus, the revised amount can be reflected starting on the first day of the following month. This new cooperative framework enables more reasonable adjustments and contributes to the stability and sustainability of public procurement by government agencies.” In addition, KOEDC is pursuing various policies to improve access to orphan drugs. Key initiatives include operating patient assistance programs in partnership with pharmaceutical companies and providing free or cost-based supply of drugs for which price negotiations are delayed. Also, the center is working to establish overseas supply chains to introduce medications for self-treatment and is running an early distribution program for pediatric orphan disease treatments.
- Company
- Cream JAKi Delgocitinib to be commercialized in Korea
- by Eo, Yun-Ho Jun 20, 2025 06:06am
- JAK inhibitors will soon be available for hand eczema in Korea as well. The Ministry of Food and Drug Safety is currently conducting a final review of LEO Pharma Korea's treatment for moderate-to-severe chronic hand eczema (CHE), Anzupgo (delgocitinib). When approved, the drug is expected to be officially commercialized in the second half of the year in Korea. Anzupgo was officially approved in Europe in November last year and is currently awaiting approval from the US FDA. This cream formulation is known as a pan-JAK inhibitor, as it targets JAK1, 2, and 3, as well as TKY2. The efficacy of Anzupgo has been demonstrated through the DELTA FORCE and DELTA 2 clinical trials, which directly compared Anzupgo with GSK's alitretinoin (Toctino). In the DELTA FORCE study, the Hand Eczema Severity Index (HECSI) score from baseline to week 12 of delgocitinib demonstrated superiority over alitretinoin capsule, meeting the primary endpoint. The DELTA 2 study included 473 patients with moderate-to-severe chronic hand eczema (CHE). Study participants were assigned to either the delgocitinib cream group or the placebo cream group and received treatment twice daily for 16 weeks. The primary endpoint was set as an IGA-CHE score of 0/1 at Week 16 of treatment. The primary secondary endpoints included IGA-CHE and the Hand Eczema Symptom Diary (HESD) assessed at Weeks 4 and 8 of treatment. The results showed that the delgocitinib group achieved significant improvement in chronic hand eczema at Week 16 compared to the placebo group, meeting the primary and primary secondary endpoints. Chronic hand eczema can be triggered by various factors such as irritants, allergies, genetic predisposition, and occupational exposure. It often leads to recurring inflammation, peeling, cracking, and pain, significantly impacting daily life. However, to date, effective topical treatments specifically targeting hand eczema remain limited. In many cases, patients show insufficient response even to corticosteroids or immunosuppressants, underscoring the ongoing need for new therapeutic alternatives. Meanwhile, LEO Pharma obtained exclusive rights in 2014 from the Japanese company Japan Tobacco to develop and commercialize a topical delgocitinib cream for dermatological indications worldwide, excluding Japan.
- Policy
- SGLT2 Jardiance likely to receive expanded reimb for CKD
- by Lee, Tak-Sun Jun 20, 2025 06:06am
- Product photo of JardianceThe SGLT-2 inhibitor Jardiance (empagliflozin, Boehringer Ingelheim) is expected to be reimbursed for the treatment of chronic kidney disease (CKD). This drug is currently reimbursed for the treatment of diabetes and chronic heart failure. If expanded reimbursement is approved for CKD, the volume of usage is likely to be increased. Furthermore, its market presence is expected to be strengthened in the SGLT-2 inhibitors market. According to industry sources on June 19, the agenda related to Jardiance's expanded reimbursement to include CKD passed the Drug Reimbursement Evaluation Committee (DREC) held on the 12th. Once it undergoes the National Health Insurance Service's simplified negotiation process and reports to the Health Insurance Policy Deliberation Committee, Jardiance is anticipated to be reimbursed for treating CKD. Since the company already completed drug price estimation process, reimbursement may be approved as early as July 1. It has been reported that Jardiance's expanded reimbursement for CKD was approved for the pre-drug price reduction program for expanded usage scope drugs. This program is designed to quickly enhance patient access to treatments by omitting the cost-effectiveness evaluation and applying a pre-reduction rate table, with a maximum 5% reduction in the ceiling cap, considering the estimated additional claim amounts due to the expanded reimbursement criteria. If a drug's ceiling price is adjusted via this program, its company will only have to undergo negotiations related to supply requirements, such as those required for other reimbursed medicines. Jardiance's company applied to the Health Insurance Review & Assessment Service (HIRA) for expanded reimbursement for Jardiance's CKD indication in the first half of last year. Jardiance was the first SGLT-2 inhibitor to file. Jardiance Tab 10mg is currently indicated for the treatment of 1. Type 2 diabetes mellitus, 2. chronic heart failure, and 3. chronic kidney disease. Jardiance Tab, which was listed for reimbursement as a diabetes treatment in 2017, has also been reimbursed for chronic heart failure since February 2024. Since January this year, the reimbursement criteria have been expanded, allowing patients with heart failure with preserved ejection fraction (HFpEF) who have symptoms and signs of heart failure and a left ventricular ejection fraction exceeding 40% to receive national health insurance benefits. Currently, the only SGLT-2 drugs covered for diabetes and chronic heart failure patients, besides Jardiance, are Forxiga (dapagliflozin) and HK inno.N's DapaN Tab, which transferred Forxiga's indications. However, there is currently no drug reimbursable for CKD. If the reimbursement expansion procedure for Jardiance is completed, it is expected to be the only SGLT-2 inhibitor with coverage for CKD reimbursement. The efficacy of Jardiance has been demonstrated through clinical trials, showing a statistically significant 28% relative risk reduction in the progression of kidney disease or cardiovascular death compared to placebo. The clinical trials that Jardiance significantly reduced a relative risk in the progression of kidney disease or cardiovascular death compared to placebo by 28%. The expanded scope of use will provide advantage in competition with generic drugs. Jardiance's substance patent expires in October this year. Therefore, tens of domestic generic drugs are likely to enter the market. Jardiance, jointly sold by Boehringer Ingelheim and Yuhan, recorded outpatient prescription sales of KRW 66.3 billion last year, according to UBIST.
- Company
- Interest in Lotte Biologcs’ partner Ottimo Pharma rises
- by Kim, Jin-Gu Jun 20, 2025 06:05am
- Interest is growing in Ottimo Pharma, a biotech company that has signed a contract manufacturing agreement for its antibody-drug with Lotte Biologics. Founded in 2017, this UK-based biotech venture owns a new drug candidate called ‘Jankistomig’. The drug candidate bifunctional antibody targeting solid tumors, and the company plans to submit an Investigational New Drug (IND) application to the US Food and Drug Administration (FDA) within this year. Lotte Biologics announced on the 19th that it has signed an antibody-drug contract manufacturing agreement with Ottimo Pharma at the BIO INTERNATIONAL 2025 (Bio USA) event. The contract covers the production of drug substance (DS) for Ottimo Pharma's antibody drug Jankistomig at the Syracuse Bio Campus in New York. Ottimo Pharma was founded in 2017 in Kent, England, under the name Ultrahuman Eight Limited. In October last year, the company changed its name to Ottimo Pharma. At that time, Medicxi Ventures UK, a UK-based life science venture capital, participated as an initial investor. Medicxi led Ottimo Pharma's Series A investment round. Ottimo Pharma successfully secured USD 140 million (approximately KRW 190 billion) in Series A investment in December last year. To date, Ottimo Pharma’s only pipeline is Jankistomig. This candidate drug works by simultaneously inhibiting PD-1 and VEGFR2. The drug candidate was known to be designed based on camrelizumab, developed by China's Jiangsu Hengrui Pharmaceuticals. It is designed to reduce VEGF-related side effects while providing immune checkpoint inhibition effects. Jankistomig is in the preclinical stage and is being tested in the UK for solid tumors. There is no clinical trial number registered on ClinicalTrials.gov, a clinical trial registration site. This suggests that no official clinical trials have been initiated in any country, including the US and the UK. The company announced last year that it had secured Series A investment and would submit an Investigational New Drug (IND) application to the US FDA by the end of this year. At the time, Ottimo mentioned its development of other pipelines in addition to Jankistomig, but did not disclose specific substance names or stages.
- Company
- New pneumococcal vaccine expected to be launched
- by Whang, byung-woo Jun 19, 2025 06:04am
- As 'Capvaxive,' a 21-valent pneumococcal conjugate vaccine (PCV21) developed by MSD, is anticipated to receive marketing authorization in South Korea, competition in the market is likely to heat up. Product photo of CapvaxiveAccording to pharmaceutical industry sources, MSD has filed with the Ministry of Food and Drug Safety (MFDS) for marketing authorization of Capvaxive. It is expected to be approved by the second half of 2025. Capvaxive is a vaccine designed to prevent adults from serotype that causes most of the invasive pneumococcal disease (IPD). The safety and immunogenicity of Capvaxive were cofirnmed based on the Phase 3 STRIDE clinical trial, comparing Capvaxive to PCV20 in adults aged 18 years and above who have no prior history of pneumococcal vaccination. Capvaxive was found to be nonequivalent to PCV20 regarding 10 serotypes (3, 6A, 7F, 8, 10A, 11A, 12F, 19A, 22F, 33F) that are commonly included in PCV20. 10 out of 11 serotypes (9N, 15A, 16F, 17F, 20A, 23A, 23B, 24F, 31, 35B) that are included in Capvaxive but not in PCV20 were demonstrated to be superior to PCV20. Capvaxive was approved in the United States in June 2024 based on these study results, and it also obtained European approval in March. There is growing attention on whether Capvaxive will obtain Korean approval during the second half of this year, as it will be the third consecutive year a new pneumococcal vaccine is approved in South Korea. In late 2023, MSD's 15-valent vaccine, 'Vaxneuvance,' was expedited for inclusion in the pediatric National Immunization Program (NIP). Then, a year later, in October 2024, Pfizer's 20-valent vaccine, Prevenar 20, won MFDS approval. As the 21-valent vaccine, which is the higher serotype vaccine, is expected to be introduced in less than a year, competition is likely to get intense. If there are no setbacks to the approval process for Capvaxive, it is expected to be launched at the very end of the first half of next year. For instance, Vaxneuvance was launched in late April, and Prevenar 20 was launched in June exclusively for adults aged 18 years and above. The market is also highly likely to be competitive, with Vaxneuvance and Prevenar 20 competing for the pediatric NIP and Prevenar 20 and Capvaxive competing for the adult NIP. Regarding this, MSD Korea is expected to employ a marketing strategy that differentiates its vaccine portfolio for pediatric (15-valent) and adult (21-valent) populations. Indeed, MSD previously announced the use of tailored strategies for pediatric and adult populations during its Vaxneuvance launch 1st-anniversary media seminar. In the long term, Pfizer's Prevenar 20, with its first-mover advantage, will be competing directly with MSD's 21-valent Capvaxive, which includes a higher number of serotypes. Capvaxive will reportedly be preventing approximately 84-85% of adult IPD. This estimate is higher than the coverage for Prevenar 20. In this case, Pfizer is expected to defend its position by highlighting the performance and extensive clinical experience of Prevenar 20. Currently, Pfizer emphasizes that Prevenar 20 offers safety and convenience based on the well-established technology of Prevenar 13, validated through long-term pediatric and adult vaccinations, and with its 20-serotype coverage. Additionally, potential competition against Sanofi-SK bioscience is another variable. Although their commercialization timeline is the latest, if they succeed in developing a 21-valent vaccine, another equally strong competitor will emerge. Notably, the Sanofi vaccine is being developed for pediatric use, suggesting that the company will employ a future strategy to cover all age groups, from infants and young children to adults.
- Company
- K-Bios face string of clinical failures in H1
- by Son, Hyung Min Jun 19, 2025 06:04am
- A series of clinical trial failures for new drug candidates under development by Korean biotech companies in the first half of the year have raised concerns about the feasibility of future technology exports. Orum Therapeutics halted a clinical trial due to safety concerns, while Genexine and Bridge Biotherapeutics both failed to demonstrate statistical significance in their respective Phase II trials for glioblastoma and idiopathic pulmonary fibrosis. Stem cell therapy developers such as Anterogen and SCM LifeScience are also struggling to prove efficacy in clinical settings. According to industry sources on the 19th, Orum Therapeutics recently suspended its Phase 1 trial of ORM-5029. ORM-5029 was the company’s only pipeline in clinical trials targeting human epidermal growth factor receptor 2 (HER2), a major biomarker for solid tumors. The company received IND approval for ORM-5029 from the U.S. FDA in 2022. However, a severe adverse event (sAE) occurred during the trial, upon which the company reported it to the FDA. Due to toxicity issues, administration had to be halted even at low doses. ORM-5029 is a Degrader Antibody Conjugate (DAC) candidate. DACs combine Targeted Protein Degradation (TPD) mechanisms with Antibody Drug Conjugates (ADCs) and are expected to offer higher safety due to the use of TPD, which are small-molecule degraders. Orum emphasized that the sAE was limited to only the ORM-5029 substance and that there were no issues with the company's technology or platform itself. Orum plans to focus its resources on its blood cancer candidate ORM-1153, which also utilizes the company’s DAC platform. The company explained that it has shown strong GSPT1 degradation and robust anti-proliferative effects in blood cancer cell lines. Genexine and Bridge Biotherapeutics fail Phase II trials Genexine and Bridge Biotherapeutics both faced setbacks in Phase II trials. In March, Genexine's GX-I7 (Interleukin-7), an immune-oncology drug candidate, failed to demonstrate efficacy in glioblastoma mulifrome (GBM) patients. GX-I7 is a new drug candidate that maximizes immune anticancer effects by inducing T-cell amplification in the body. GBM is a type of glioma, a malignant tumor that originates in the brain. Despite surgery and chemotherapy, the five-year survival rate for GBM is only 5%, with an average survival time of about a year. The Phase II trial for GX-I7 enrolled 20 patients with recurrent or progressive glioblastoma, and evaluated a combination of the GX-I7 and bevacizumab (Avastin), a VEGF inhibitor used as a targeted therapy. Bevacizumab inhibits angiogenesis to prevent tumor growth, and its combination with existing anticancer drugs was expected to enhance therapeutic efficacy. However, no significant improvement was observed in the primary endpoints of progression-free survival (PFS) and overall survival (OS). Meanwhile, Bridge Biotherapeutics announced in April that its top-line data analysis results showed that its idiopathic pulmonary fibrosis (IPF) candidate BBT-877 failed to demonstrate a statistically significant improvement in the primary endpoint of forced vital capacity (FVC) change at 24 weeks. BBT-877 is an innovative novel drug candidate that selectively inhibits the novel target protein autotaxin. Autotaxin is a protein known to bind to intracellular receptors and be involved in pathological mechanisms such as fibrosis and tumorigenesis. BridgeBio previously secured global exclusive rights to BBT-877 from LegoChem Bio (now LigaChem Bio) in 2017. In May, BridgeBio received a recommendation from the IDMC to continue the clinical trial. The Phase 2 clinical trial of BBT-877 was conducted in 5 countries - South Korea, the United States, Australia, Poland, and Israel - to evaluate the efficacy, safety, and tolerability of the drug in patients with idiopathic pulmonary fibrosis (IPF). A total of 129 patients participated, and the study results showed that changes in FVC were observed in both the drug group and the placebo group; however, there was no statistically significant difference between the two groups. Bridge Biotherapeutics licensed out BBT-877 to Boehringer Ingelheim in 2019 in a deal worth up to KRW 1.5 trillion. Upon transferring BBT-877, which was in Phase 1 clinical trials, the company received approximately KRW 600 billion in upfront and milestone payments (short-term milestones). In late 2019, following the completion of Phase I clinical trials for BBT-877, BridgeBio paid approximately KRW 50 billion to LigaChem Bio as milestone revenue sharing. However, in 2020, Boehringer Ingelheim returned the rights to BBT-877 due to potential toxicity issues. BridgeBio determined that the toxicity issues were caused by high-dose drug administration in additional experiments and decided to develop the candidate on its own, but failed to demonstrate its efficacy in trials. stem cell therapy developers also struggling with commercialization Stem cell therapy developers are also facing commercialization hurdles. SCM LifeScience failed to achieve statistical significance in Phase 2 clinical trials of its stem cell therapy candidate SCM-CGH. This is the company's second failed attempt at commercialization following the failure of its acute pancreatitis clinical trial in 2022. The trial, which targeted patients with steroid-resistant or steroid-dependent chronic graft-versus-host disease, was conducted from 2017 to 2024 at 11 hospitals in South Korea, including Seoul St. Mary's Hospital. The results of the Phase II clinical trial of SCM-CGH showed no statistically significant difference in the primary efficacy endpoint, the overall response rate (ORR) at 12 weeks. Upon closer examination, the ORR at 12 weeks was higher in the placebo group than in the SCM-CGH group, and the results were not statistically significant. Anterogen failed to demonstrate the efficacy of its stem cell therapy ALLO-ASC-DFU in the U.S. Phase III clinical trial. In the trial, ALLO-ASC-DFU recorded a complete wound closure rate of 46%, which was lower than the 60% in the control group that was treated with hydrogel sheets. The therapy had garnered attention as a treatment for diabetic foot ulcers (DFU), but its failure to meet the key primary endpoint has significantly reduced the likelihood of its FDA approval. Anterogen is conducting further analyses to revise its development strategy.
- Company
- KOR-JPN jointly launches Healthcare Distribution Alliance
- by Son, Hyung Min Jun 19, 2025 06:03am
- (From the left) Jun-Jae Hyeon (CEO, Dongwon Healthcare), Jun-ho Hyun (CEO, Dongwon Pharmaceutical Wholesale), Seung-Uk Eom (CEO, Boksan Nice), and Seongwook Cho (Country Manager, Suzuken Korea) Three pharmaceutical distribution companies in Korea and Japan have joined forces to launch the Healthcare Distribution Alliance to lead the domestic market by introducing advanced overseas models. The alliance aims to go beyond simple logistics agreements – it seeks to build an innovative cooperation structure where companies can share capital and operational know-how, and combine each company's strengths to transform the pharmaceutical distribution market. Jun-Jae Hyeon (CEO, Dongwon Healthcare), Jun-ho Hyun (CEO, Dongwon Pharmaceutical Wholesale), Seung-Uk Eom (CEO, Boksan Nice), and Seongwook Cho (Country Manager, Suzuken Korea) recently met with reporters to explain the alliance's goals. Eight affiliates of Dongwon Pharmaceutical Group, Boksan Nice, and Suzuken have signed a business partnership agreement and established an organizational framework for cooperative operations at the alliance level. As part of the collaboration, the companies also entered into a capital partnership, with Suzuken acquiring a 33.6% stake in Gyeongnam Dongwon Pharmaceutical, and Boksan Nice acquiring a 3.4% stake in Gyeongnam Dongwon Pharmaceutical. This alliance goes beyond simple logistics cooperation by sharing capital and strategy direction of the companies. With the direct participation and investment of Suzuken, a major Japanese pharmaceutical distribution company, the alliance aims to pursue a long-term model that pursues the maximization of distribution productivity, supply chain stability, and function as part of a social infrastructure. CEO Seung-Uk Eom said, “We decided to pursue this alliance to survive in the rapidly changing pharmaceutical distribution industry and create growth opportunities through innovation. We aim to realize economies of scale through the alliance between Dongwon Pharmaceutical, Boksan Nice, and Suzuken and maximize productivity in the pharmaceutical distribution market while driving innovation for mutual growth.” Industry observers expect synergy from the partnership. Dongwon Pharmaceutical Group and Boksan Nice each reported over KRW 1 trillion in annual sales last year. Suzuken, one of Japan's top three pharmaceutical distributors, posted annual revenue exceeding JPY 2 trillion (approx. KRW 19 trillion) in 2023. CEO Jun-ho Hyun emphasized, “As the pharmaceutical distribution environment evolves and capital requirements grow, scaling up is no longer an option – it’s a necessity. We aim to establish a Korean-style large-scale distribution model and guide the future direction of the market.” The alliance anticipates increased distribution-related costs and volatility in the coming years. To address this, it aims to build a robust infrastructure and reduce labor dependency. Plans include exploring hospital market strategies, logistics outsourcing services, private-label (PB) healthcare products, and the potential introduction of Suzuken’s current Japanese business operations into the Korean market. CEO Seung-Uk Eom noted, “In the short term, we’ll focus on collaboration between logistics centers within the alliance, which is expected to reduce stockouts and delivery lead times through optimal inventory and shipping operations.” He added, “In the long term, we plan to build systems such as enterprise resource planning (ERP), web order systems (WOS), and customer relationship management (CRM). Given the significant time and cost required for IT system development, combining the long-standing expertise and ideas of Suzuken, Boksan Nice, and Dongwon Pharmaceutical will not only facilitate joint development but also greatly contribute to future logistics innovations such as the modernization of logistics and improvements in operational efficiency involving robots and AI. CEO Seung-Uk Eom added, “Beyond transportation management systems (TMS) and quality control standards, we will also build a foundation system for environmental, social, and governance (ESG) and seek ways to advance them.” CEO Jun-ho Hyun said, “Profit margins for pharmaceutical distributors have been steadily shrinking. Survival through sales promotion activities alone is becoming difficult. We must scale up and differentiate through cost reduction and pharmaceutical partnerships.” ”Will seek to implement Japanese-style wholesale structure in Korea" The alliance is eyeing the Japanese model, where pharmaceutical distribution is treated as a core part of national infrastructure, with government, pharma companies, wholesalers, and hospitals working in unison. Even logistics center placements are coordinated with government authorities, and disaster response systems are embedded into the distribution network. Japan’s market is dominated by major distributors like Medipal, Alfresa, and Suzuken, which fulfill roles as social infrastructure through close cooperation across the pharmaceutical supply chain. CEO Jun-jae Hyeon noted, “In Japan, systems are in place to ensure medicine continues to flow even during national disasters like earthquakes and tsunamis. We aspire to build such a socially integrated distribution system here in Korea.” Country Manager Seongwook Cho said, “, “Japan has established a virtuous cycle model that contributes to the national health insurance budget by minimizing the deterioration of medicine quality and the amount of expired medicines through infrastructure development. Although this may not be immediately achievable in South Korea, we will do our best to prepare for it." In addition, as more and more pharmaceutical companies are expected to develop new drugs such as biological agents, anticancer drugs, and orphan drugs, it is necessary to establish a system to manage and deliver these drugs. The association aims to provide one-stop services tailored to their needs. Country Manager Seongwook Cho said, “Suzuken already communicates and conducts business with many multinational pharmaceutical companies in Japan. We are aware that the companies have high standards for quality control and other global requirements. Our association’s goal is to meet the standards set by such global companies in various areas, including logistics and cold chain.” CEO Jun-jae Hyeon said, “In Japan, there are various pharmaceutical platforms, with distribution companies at the center of each. All transactions between healthcare institutions and related organizations are conducted through distribution companies. We will strive to establish a similar structure in Korea, where distribution companies play a central role in facilitating various activities.”