- LOGIN
- MemberShip
- 2026-04-04 13:41:29
- Policy
- Will generics dominate the oral psoriasis treatment market?
- by Lee, Tak-Sun Oct 14, 2024 05:49am
- Dong-A ST The global market for oral psoriasis treatment amounts to KRW 5 trillion. In the Korean market, generic medicines are likely to dominate. The original medicine company withdrew its drug from the Korean market due to dissatisfaction with the reimbursement decision, whereas generic medicines are likely to accept the term. A new type of oral medicine is likely to be competitive because psoriasis treatments that are available in South Korea are primarily injectables. The Drug Reimbursement Evaluation Committee (DREC) of the Health Insurance Review held its 10th meeting for 2024 on October 10th and ruled that medicines containing apremilast would be appropriate for reimbursement coverage if the company accepted the drug price below the evaluated amount. These medicines include 5 products: Otelia (Dong-A ST), Apsola (Daeowoong Pharmaceutical), Otebell (Chong Kun Dang), Otemila (Dongkoo Bio), and Psopre Tab (Hanlim Pharm). The originial medicine containing apremilast is Amgen's 'Otezla.' Otezla received marketing authorization in South Korea in November 2017. However, the company voluntarily withdrew approval in 2022 due to dissatisfaction with the domestic reimbursement decision. Otezla is a PDE4 (phosphodiesterase 4) inhibitor used to treat psoriasis. A PDE4 inhibitor blocks the activation of PDE4 enzyme that causes inflammatory responses. The Korean market for psoriasis treatments is led by injectable interleukin agents. These include Stelara (Janssen) and Cosentyx (Novartis). Like the case of generics, Otezla also received a conditional pass during the DREC review. In May 2018, the DREC review decided that Otezla is non-inferior to Enbrel inj for the treatment of psoriasis and Stelara for the treatment of psoriatic arthritis, but the drug is not cost-effective due to its high cost relevant to the treatment duration. The government said it would agree on reimbursement appropriateness if the pharmaceutical company accepted the drug price below the weighted mean price of substitute medicines. However, the pharmaceutical company did not accept it. Although the original medicine did not accept the conditional agreement for reimbursement, generic companies are likely to wrap up the reimbursement listing process by accepting it. Dong-A ST has already launched Otelia as non-reimbursable in July and began sales·marketing. Generic companies have no problems launching their products after avoiding patents and reaching an agreement with Amgen. When generic companies accept the DREC review decision, they will start a negotiation with the National Health Insurance Service (NHIS). If a company accepts a drug price negotiation exemption criterion (90% below the weighted average price of substitute medicines), it can conclude the negotiation early by skipping the drug price negotiation and starting the estimated claim amount negotiation. "Patients would have had difficulty accessing the medicine containing this active ingredient if it had not been for the Korean pharmaceutical company," pharmaceutical industry personnel said. "We look forward to seeing whether generic companies with new types of oral products would take the market share in the psoriasis treatment market dominated by foreign pharmaceutical companies."
- Policy
- NA-MFDS clash on the approval of abortion pills
- by Lee, Jeong-Hwan Oct 14, 2024 05:49am
- With the National Assembly strongly pressing the need for domestic marketing authorization of the abortion drug ‘Mifegymiso,’ the NA’s request is set to affect the future administration of the MFDS’s marketing authorization review. The MFDS has repeatedly argued that the Criminal Act and the Mother and Child Health Act must be amended before the drug receives marketing authorization, but the National Assembly responded that this is an unacceptable excuse and that the drug’s listing should not be delayed any longer. On the 10th, Democratic Party of Korea lawmaker In-soon Nam made inquires to Yu-Kyoung Oh, the head of the Minister of Food and Drug Safety, that the government should take steps to identify the illegal distribution, trade, misuse, and side effects of Mifegymiso by granting marketing authorization for the abortion drug. In fact, 705 cases of illegal sales of abortion drugs such as Mifegymiso were found by July this year. Rep Nam pointed to the fact that doctors, pharmacists, and civil society organizations have filed multiple requests for the designation of abortion drugs as essential medicine and their urgent introduction, and requested the MFDS to be proactive in grating their marketing authorization. “The Board of Audit received an audit claim that the MFDS is neglecting its responsibility to introduce abortion drugs,” Nam said, adding, “I think the MFDS should respond quickly.” Rep. Nam added, “There are WHO guidelines, and preparations (permits) that need to be made. Please study cases overseas and review and submit these contents until the general audit. You shouldn't just blame it on the law. Women are being harmed.” Minister Oh said that she would submit the data that the MFDS had prepared for the marketing authorization, but replied that “MFDS is a licensing agency” and that “We lack the requirements to grant marketing authorization (for abortion pills).” So what does Minister Oh mean by ‘lack of requirements’? Hyundai Pharm, which had been preparing to distribute the abortion drug Mifegymiso in Korea, applied for marketing authorization to MFDS several times. Specifically, Hyundai applied for the marketing authorization of Mifegymiso in July 2021, and then voluntarily withdrew the application in December 2022. In March 2023, the company reapplied for Mifegymiso, and the MFDS currently has the application and supporting data. The MFDS has repeatedly explained that the Criminal Act and the Mother and Child Health Act must be amended before granting marketing authorization for the drug. The amendments to the Criminal Act and the Mother and Child Health Act need to be made to clarify the period of abortion permitted by law so that the risk management plan required for the approval and review of abortion drugs can be confirmed. In other words, the MFDS’s position is that the relevant laws must be amended first, and then the pharmaceutical company must submit the risk management plan approval data for the Ministry to resume the review and decide whether to approve the drug for marketing authorization. However, members of the National Assembly's Ministry of Health and Welfare, including Rep Nam, have been pointing out that the MFDS’s position is difficult to accept. The criticism is that the agency is using the risk management plan as an excuse to avoid getting involved in the controversy over the approval of the abortion pill. “It is difficult to understand the MFDS’s explanation that it cannot approve abortion pills because the National Assembly has not passed subsequent legislations related to abortion, such as the Criminal Act and the Mother and Child Health Act,” said an official from the National Assembly's Welfare Committee. “Drugs should be approved based on safety and efficacy based on scientific and medical review data. Whether the abortion period is set at 16 weeks or 36 weeks should not affect MFDS’s safety and efficacy review.”
- Policy
- Approval process for 'Leqembi' heavily debated
- by Lee, Hye-Kyung Oct 14, 2024 05:49am
- A heated debate is expected during the National Assembly regarding the approval process for Leqembi (lecanemab), a new drug for treating dementia that received domestic approval in May. Rep. Jeon Jin-sook, a member of the Democratic Party of Korea.At a parliamentary audit of the Health and Welfare Committee held at the National Assembly on October 10th, Rep. Jeon Jin-sook, a member of the Democratic Party of Korea, issued an allegation that the approval of a new drug for dementia in South Korea has been granted without a review by the Central Pharmaceutical Affairs Council. This drug received a recommendation for non-approval from the European Medicines Agency's (EMA) Committee for Medicinal Products for Human Use (CHMP) due to side effects. "Although this drug is a new drug, approval has been granted without seeking expert opinion," Rep. Jeon said. "In the United States, this drug was approved with the required warning label statement in the prescribing information after the FDA's advisory committee meeting. Europe postponed approval," Rep. Jeon explained. Although the product name of the drug had not been disclosed during the parliamentary audit, the only new drug to have received approval as a treatment for dementia is Eisai Korea's Leqembi. Leqembi was approved for an indication to treat 'Mild cognitive impairment (MCI) due to Alzheimer's disease (AD) and mild AD dementia.' The drug's effects and safety have not yet been confirmed for AD patients with moderate symptoms or higher. "No medicines can guarantee a 0% side effects, even for innovative products," Rep. Jeon said. "This drug is known to damage walls of the blood vessels, thereby causing edema of the brain, cerebral hemorrhage, confusion, and convulsion." The representative also pointed out a diagnostic test that needs to be periodically performed when using Leqembi. "To continuously check on side effects of this drug, a targeted medicine, patients are required to take expensive diagnostic tests," Rep. Jeon said, adding, "Stock traders are saying that a new diagnostic test era has begun." "We have an allegation that (during the approval process for this new drug) a privilege has been granted to high-priced diagnostic testings," Rep. Jeon said. "It may require an official audit. We want a detailed explanation before the comprehensive review about skipping expert review during the approval process for this dementia drug."
- Policy
- Drug pricing negotiations for Qarziba gather pace
- by Lee, Tak-Sun Oct 14, 2024 05:49am
- With Qarziba Inj (dinutuximab beta, Recordati Korea), the first drug that has been applied the approval-evaluation-negotiation pilot project, passing the Health Insurance Review and Assessment Service's Drug Reimbursement Evaluation Committee, the drug price negotiation for the drug is also expected to progress quickly. However, the drug’s post-listing management is expected to be key rather than the speed of approval. Qarziba was recognized as adequate for reimbursement at the 10th Drug Reimbursement Evaluation Committee (DREC) meeting in 2024 that was held on the 10th of this month. The committee had made a non-reimbursement decision in August, but after reconsideration, the drug passed HIRA’s reimbursement review stage. Qarziba is the first drug in the approval-evaluation-negotiation pilot project, which received MFDS approval, drug price evaluation, and drug price negotiation in parallel to support its prompt reimbursement listing. It also succeeded in setting reimbursement standards before approval. On May 29, the 4th Cancer Disease Deliberation Committee set the reimbursement standard for Qarziba as children aged 12 months or older with ▲high-risk neuroblastoma who have previously received myeloablative therapy and stem cell transplantation and shown partial response or after induction chemotherapy, and ▲recurrent or refractory neuroblastoma. On June 19th, the company also received formal marketing authorization from the MFDS. The approval period was also shortened from 115 days to 90 days as it was designated a drug for the Global Innovative Product Fast Track (GIFT) support system. Its drug price negotiation period is also expected to be shortened. This is because the negotiation period for drugs in the approval-evaluation-negotiation pilot project is shortened from 60 days to 30 days through preliminary discussions before passing the Drug Reimbursement Evaluation Committee. Therefore, its reimbursement is expected within the year. However, it was pointed out that there are limitations to sufficient pre-validation of the drug due to its fast-track status. Therefore, it is likely that its financial sharing plan will be considered through a post-listing evaluation process. In fact, HIRA is reportedly reviewing applying patient-level performance evaluations. The patient-level performance evaluation measure was applied to the one-shot high-priced drugs Kymriah and Zolgensma. It mainly involves a contract that monitors the performance of each patient, after which the pharmaceutical company reimburses a percentage of the drug cost if the treatment fails. This type of post-listing management measure is likely to be set as a prerequisite during the NHIS pricing negotiations. If Qarziba is listed within the year, it will have taken just one and a half years from approval to reimbursement. Normally, the process takes 3 years. With more approval-evaluation-negotiation pilot projects being processed, Qarziba’s reimbursement listing will help solidify the review and negotiation processes of the project. An industry official said, ‘The key to Qarziba’s drug price negotiation will be in the financial sharing plan after registration,’ adding, ‘As it is a fast-track drug, the NHIS would also have much to consider.”
- Company
- Dong-A ST’s biosimilar first enters the U.S. market
- by Chon, Seung-Hyun Oct 14, 2024 05:49am
- Dong-A S.T. has succeeded in entering the US market 13 years after declaring its entry into the biosimilar business. It has received approval in the US for a biosimilar version of Stelara, which owns a global market worth KRW 14 trillion. It was the company’s second overseas market with a self-developed biosimilar. The biosimilar's entry into the U.S. market secured additional technology fee revenues and added a new item for the company. Pic of Dong-A ST headquarters According to industry sources, Dong-A ST's Stelara biosimilar ‘Imuldosa’ was approved by the US Food and Drug Administration (FDA) on the 12th. Stelara is a treatment for inflammatory diseases such as plaque psoriasis, psoriatic arthritis, Crohn's disease, and ulcerative colitis. It is a high-grossing product that generated more than KRW 14 trillion in global sales last year. Dong-A ST is the second Korean company to receive approval for a Stelara biosimilar in the US following Samsung Bioepis. Dong-A ST passed the US market gateway 11 years after it started developing its Stelara biosimilar in 2013. Dong-A Socio Holdings began codeveloping Imuldosa with Japan's Meiji Seika Pharma in 2013. In July 2020, the development and commercialization rights were transferred to Dong-A ST for efficient execution of the global project. From 2021 to the end of 2022, Dong-A ST conducted a global Phase III clinical trial of Imuldosa in 9 countries including the United States, Poland, and Estonia, on a total of 605 patients. Trial results confirmed that Imuldosa’s efficacy and safety was equivalent to is equivalent to Stelara for marketing authorization by the U.S. Food and Drug Administration (FDA) and European Medicines Agency (EMA) Imuldosa's FDA approval is expected to generate additional technology fees. In July 2021, Dong-A ST signed a technology export agreement with the multinational pharmaceutical company Intas Pharmaceutical to license out Imuldosa. Intas paid a non-refundable upfront payment of USD 10 million. The payments based on clinical, licensing, and sales milestones were set at up to USD 95 million. Royalties on product sales are guaranteed to be at least 10%. In addition, payments from Intas will be shared by Dong-A ST, Dong-A Socio Holdings, and Meiji Seika Pharma. Intas has secured exclusive rights to license and market the product globally, excluding South Korea, Japan, and select Asian countries. Intas is an Indian multinational pharmaceutical company with a global sales network in more than 85 countries. Global commercialization will be handled by Accord Healthcare, a subsidiary of Intas Pharmaceuticals. Accord Healthcare submitted a marketing authorization application for Imuldosa to the European Medicines Agency (EMA) in June last year and submitted an application to the FDA in October last year. By the end of the first half of last year, Dong-A ST had recognized KRW 41 billion as development costs for Imuldosa as an intangible asset. The Financial Supervisory Service has identified Phase III clinical trials as the stage at which new drug R&D costs can be capitalized. This means that KRW 41 billion was spent on global Phase III clinical trials of Imuldosa. Dong-A ST announced its entry into the biosimilar business in 2011. In 2011, Dong-A Socio Holdings established DM Bio with an investment of KRW 57 billion from Meiji Seika Pharma to build a biopharmaceutical plant. In March 2015, Dong-A Socio Holdings spun off DM Bio into a 100% subsidiary and transferred 49% of its shares to Meiji Seika Pharma. In 2021, Dong-A Socio Holdings acquired 1,117,200 shares of DM Bio from Meiji Seika Pharma for KRW 42.1 billion. The company's stake in DM Bio increased to 80.4% as it took over 60% of the 1.86 million DM Bio’s shares held by Meiji Seika Pharma. In 2022, DM Bio changed its name to STgen Bio. STgen Bio will be responsible for the production of Imuldosa. Imuldosa is the second biosimilar product that Dong-A ST has successfully commercialized in overseas markets. Dong-A ST sells Nesp's biosimilar version, ‘darbepoetin alfa’ in Japan. Dong-A ST conducted Phase I clinical trials of darbepoetin alfa and transferred the development and sales rights in Japan to Sanwa Kagaku Kenkyusho (SKK) in January 2014. Based on the results of a local Phase III clinical trial comparing the original Nesp with darbepoetin alfa, SKK received marketing authorization from the Japanese Ministry of Health, Labour and Welfare in September 2019, and launched the drug in late November of the same year. Dong-A ST will export the finished product manufactured on consignment by STgen Bio to SKK, and SKK is in charge of local sales. Last year, Dong-A ST recorded 20.6 billion won in exports with its dabepoetin alfa.
- Company
- ERT demonstrates effectiveness in treating Fabry disease
- by Whang, byung-woo Oct 11, 2024 06:25am
- "'It has been 20 years since ERT treatments became available for patients with Fabry disease. More treatment options are available to treat Fabry disease, but selecting treatment options and strategy requires precise attention based on research data." Analysis suggests that the treatment environment for rare diseases has improved due to the emergence of Enzyme Replacement Therapy (ERT) to treat lysosomal storage disease (LSD), such as Fabry disease. New treatment strategies and research for treatments are being conducted to complement the limitations of ERTs. For example, studies on treatments like Substrate Reduction Therapy (SRT) are being conducted. Antonio Pisani, a professor in the Department of Nephrology at the University of Naples Federico II. However, considering the nature of rare diseases, using available treatment resources to the fullest remains equally important. Antonio Pisani, a professor in the Department of Nephrology at the University of Naples Federico II, has emphasized the importance of monitoring when switching between medicines for treating Fabry disease during a meeting with Daily Pharm. A study comparing ERT→oral drug switching…disease management through monitoring is essential During the WORLD Symposium 2024, held in San Diego, USA, in February, a study result was presented that close monitoring for medication switching is essential. It is because after a patient switch from Fabrazyme to oral drugs, a long-term change in treatment outcomes has been reported. The study is expected to aid in selecting treatments as it compares the efficacy and safety of the ERT treatment, Fabrazyme, to an oral drug, migalastat, using registry data on patients with Fabry disease. "Migalastat has been approved in Europe in 2016. However, the use of the drug has been limited because there is no real-world evidence (RWE) besides pre-clinical or clinical results," Professor Pisani, who conducted the research, said, "The study analyzed data of patients who had been treated with Fabrazyme over a year and then switched to migalasta and continued treatment over six months. It confirmed various biomarkers for Fabry disease, changes to patient symptoms, whether a patient reached first-line treatment goal and clinical symptoms." Based on research results, migalastat treatment, compared to Fabrazyme, worsened an estimated glomerular filtration rate (GFR), a biomarker for Fabry disease, and GL-3 level, a glycolipid in cells. Additionally, a classical-type patient with Fabry disease who switched to migalastat had worsened UPCR and heart index, demonstrating that Fabrazyme is much more effective in treating patients with Fabry disease. "The study confirmed that migalastat has variability in efficacy in a clinical setting," Professor Pisani said, "We concluded that a close monitoring and patient follow-up is important when a patient has been switched to migalastat following Fabrazyme treatment." "A close monitoring of enzyme activation and changes to clinical symptoms is necessary. A change in enzyme activation is expected once a patient starts taking migalastat. Therefore, medication switching requires patient follow-up," Professor Pisani emphasized. Migalastat is approved in South Korea as a long-term treatment for patients over 12 years old diagnosed with Fabry disease with a gene variant. An oral drug can be reimbursed for second-line treatment when a patient has used ERT for over 12 months in a first-line treatment or cannot use ERT. If the study results were to apply to Korea, what could be the possible analysis? Professor Pisani advises that physicians must carefully consider medication switching based on treatment guidelines for Fabry disease. "There are studies implicating positive efficacy of migalastat. However, there are opposite results," Professor Pisani said, "When treating with migalastat, physicians must monitor patients by checking biomarkers, such as eGRF and proteinuria, to confirm the efficacy of the use." Treatment outcomes of migalastat may vary depending on the patient's condition. For example, a classical-type patient with Fabry disease may have a stable or worsened heart-related index upon switching medication to migalastat, but worsening renal functions may accelerate significantly. "In the end, a follow-up of patients is essential, and it is important to closely monitor symptoms and disease progression of patients with poor baseline indexes," Professor Pisani said. Still there are limitations to Fabry disease treatment…what are unmet needs? New Fabry disease treatments are available, and real-world data have been presented. Although these improvements have been made for patients with Fabry disease, there are still unmet needs. Professor Pisani highly values the benefits brought by ERT treatments to patients with Fabry disease. Yet, he emphasizes the need for new drug development. Studies being conducted related to new treatment strategies and drugs to complement ERT treatment limitations. For example, studies on substrate reduction therapy and gene therapy are being conducted. "We can consider possibilities, such as treatment development, including new ERT and chaperone, a combination therapy containing chaperone, or Fabrazyme in combination with gene therapy," Professor Pisani said. "We can approach Fabry disease with new treatments, such as SRT, as it is a lysosomal storage disorder." Yet, new treatment development takes time. Therefore, a strategic approach is necessary using known research results. "There are several possibilities for Fabry disease treatment. Physicians should now plan treatment option selection and strategy using research data," Professor Pisani said. "The dosage of treatment is an important factor for Fabry disease. A sufficient dosage administration can delay the disease progression." "I would like to emphasize the importance of early treatment through early diagnosis. Early treatment can delay the disease progression and worsening," Professor Pisani emphasizes.
- Company
- ‘Switching between AD drugs’ discussed at NA audit
- by Whang, byung-woo Oct 11, 2024 05:54am
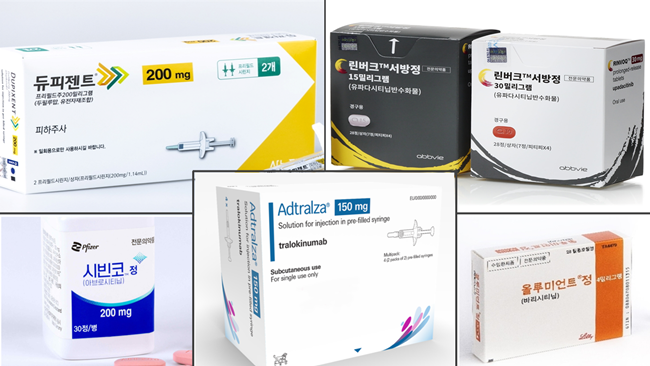
- The issue of switching between medications for severe atopic dermatitis, whose need had been voiced constantly in the clinical field, has been mentioned during the National Assembly Audit, attracting attention to whether the reimbursement environment will change. (Clockwise from top left) Pic of Dupixent, RInvoq, Olumiant, Adtralza, Civinqo During the National Audit of the National Assembly's Health and Welfare Committee on the 8th of this month, Democratic Party Rep Jin-Suk Jeon asked Minister of Health and Welfare Kyoo-Hong Cho about the issue of switching between medication for atopic dermatitis. Currently, the special calculation and reimbursement standards for switching between medications in severe atopic dermatitis stipulate that ‘starting treatment with one of the biologics or JAK inhibitors and then changing to another’ is not eligible for special calculation and reimbursement. However, experts have consistently expressed the opinion that atopic dermatitis is a disease that features various characteristics in each patient, which is why it is necessary to switch between treatments for personalized treatment. The Korean Atopic Dermatitis Association’s ‘2024 Korean Atopic Dermatitis Treatment Guidelines’ which was revised after 9 years, also made specific recommendations to address this issue of switching. The association’s position is that patients should be able to switch between medicines regardless of the line of therapy or class of drug, without having to decide which drug is more appropriate, as it is difficult to be sure of the decision. “Patients cannot switch from one drug to another even through other options are available,” said Jo-Eun Park, CEO of the Severe Atopic Dermatitis, Association who attended the meeting as a witness. “The government does not apply health insurance and special calculation cases when switching drugs, so patients have to pay for up to KRW 17 million on drugs per year if they switch to another drug.” “Even when a new drug is released, the only drug available to patients is the first drug they choose. If they want to change their medication due to severe side effects or ineffectiveness, they will have to stop treatment and worsen their condition in order to meet the criteria for reimbursement and special calculation of the other drug.” Park also pointed out that patients with psoriasis, a skin condition similar to severe atopic dermatitis, can switch to different medications when they are ineffective or have side effects, which shows the disparity in the treatment environment of the two. In this regard, Rep Jeon asked Minister Cho to review the need for switching between severe atopic dermatitis drugs and prepare measures. Minister Cho said, ‘I understand that switching between drugs for atopic dermatitis is an important issue, and I think the evidence is accumulating now. I was told that the Health Insurance Review and Assessment Service will actively review the issue.” Despite the positive response, the key to its outcome may depend on the budget budget, including Korea’s health insurance finances. In fact, the notification of the amendment related to the recognition of insurance reimbursement benefits for switching between JAK inhibitors in rheumatoid arthritis, which was scheduled to be implemented in October, has been put on hold. According to the industry, the delay is due to budgetary issues. The government is likely to face similar challenges to rheumatoid arthritis, as the core issue in atopy dermatitis is also focused on switching between biologics and JAK inhibitors. According to the drug market research institution UBIST, the outpatient prescription market for JAK inhibitors reached KRW 27.5 billion in the first half of last year. This is a 54% increase from the KRW 17.8 billion made in the first half of last year.
- Policy
- MFDS Minister ‘will work with MOHW on INN prescriptions’
- by Lee, Hye-Kyung Oct 11, 2024 05:54am
- International non-proprietary names (INNs) and ingredient-based prescriptions should be introduced to prevent patients from circling pharmacies due to drug shortages, said a lawmaker. ‘Institutional inducements such as the introduction of INNs and ingredient-name prescriptions are needed to prevent drug supply disruptions and pharmacy bouncing issues from occurring again,’ said Representative Young-Seok Seo (Democratic Party of Korea) during the National Assembly Health and Welfare Committee's NA audit of the Ministry of Food and Drug Safety “According to a recent survey, the public's trust in generic quality is about 50%, but 80% responded that they will take generic versions if doctors prescribe them,” said Rep. Seo, adding, “There seems to be low awareness of the bioequivalence of generics drugs and original drugs, but hasn't the MFDS recommended making International Nonproprietary Names (INN) prescriptions?” Regarding the inquiry, Yu-Kyoung Oh, Minister of Food and Drug Safety responded, “The Ministry of Health and Welfare is the main ministry in charge of INN prescriptions, and the MFDS once said that we would cooperate if the Ministry of Health and Welfare takes initiative.” Oh added, “We can say that an effect of a drug is equivalent if we conduct bioequivalence tests. In the case of INN prescriptions, the MFDS will be able to cooperate if the MOHW initiates the discussion.” It was also pointed out that the public-private consultative body for the unstable supply and demand of drugs, which involves both the MOHW and the MFDS, is not working organically due to the disconnect between ministries. “I wonder if the disconnect between the ministries is aggravating the supply and demand instability. Why should there be a shortage of medicines when there is a consultative body ready?’ Seo asked, stressing that ’inter-ministerial discussions are needed to minimize the disconnect.’ In response, Oh said, “The MFDS receives reports of supply shortages from pharmaceutical companies, and the MOHW receives reports from pharmacies and hospitals, so the report process is different. So we create a system when we meet as part of the public-private consultative body, but as there are various causes of supply and demand disruptions, we plan to discuss them in depth at the consultative body’s meeting.”
- Opinion
- [Reporter's view] Creating a virtuous cycle for K-bio growth
- by Son, Hyung Min Oct 11, 2024 05:54am
- The research and development (R&D) trend in the biopharmaceutical industry is focusing on new anticancer drugs. The field is gaining interest, especially following the clinical success of Yuhan Corp's Leclaza (ingredient: Lazertinib) and HLB's rivoceranib. In particular, most biotech companies in South Korea are confirming the clinical potential of drugs in combination with Keytruda. Keytruda is an immune checkpoint inhibitor developed by MSD and a successful blockbuster medicine with over 30 indications in South Korea alone. Keytruda's global sales this year are expected to amount to KRW 3.5 billion. Almost all biotech companies in South Korea aim to out-license their technologies to MSD through clinical trials of combination therapy with Keytruda. A combination therapy involving medicine with proven effects is highly likely to be commercialized. However, R&D in the Korean industry seems to be focusing only on anticancer drugs for the purpose of out-licensing them to a big global pharmaceutical company. To date, several biopharmaceutical companies in South Korea are reporting confirmation of the efficacy of their drugs in combination with Keytruda through preclinical trials or early-stage clinical trials. However, there have been no reports of entering late-stage clinical trials, thereby nearing commercialization, or of outstanding out-licensing. In addition to Keytruda, the next target of the biopharmaceutical industry in South Korea is Enhertu. A second-generation antibody-drug conjugate, Enhertu (ingredient: trastuzumab deruxtecan), has demonstrated efficacy and is effective for breast cancer, gastric cancer, non-small cell lung cancer, and colorectal cancer. The biopharmaceutical industry in South Korea is exploring the market for ADC anticancer drugs. Even the long-standing pharmaceutical companies and the biotech industry have shown interest in ADC development. Several companies have already begun clinical trials involving combination therapy with Enhertu. It is common for Korean companies to pursue out-licensing as it allows them to secure funds for investments in other pipelines through out-licensing and provides opportunity to discover new drugs. However, if the industry continues to chase after blockbuster new anticancer drugs, it will lead to a difficult system to develop new innovative drugs domestically. Consequently, companies must explore new fields besides anticancer drugs. Instead of pursuing a partner in a combination therapy involving a well-selling drug, they should explore a field with unmet needs to create various out-licensing opportunities. The R&D costs in the biopharmaceutical industry in South Korea are incomparably smaller than those of global pharmaceutical companies. A stable source of funds is essential to sustain a virtuous cycle. Running a company by continuously developing competitive new drug candidates and successfully out-licensing is almost impossible. As a result, it is important to have experience collaborating with other companies to secure Korean and Asian rights when discussing out-licensing agreements with a global pharmaceutical company. Pharmaceutical companies can only sustain stable earnings through selling drugs. The biopharmaceutical industry is one of the industries with a large gap between Korean and global companies. The biopharmaceutical industry cannot benefit from good deals because it cannot produce good products and sell them cheaply. Now, the biopharmaceutical industry in South Korea must consider challenging various fields and creating a system to profit from selling new drugs. Clinical trials involving combination therapy containing new drugs are already supersaturated.
- Company
- Will Tevimbra be reimbursed promptly in Korea?
- by Eo, Yun-Ho Oct 11, 2024 05:54am
- Whether an immuno-oncology treatment option will arise in the oesophageal cancer space is garnering attention. BeiGene Korea's immuno-oncology drug Tevimbra (tislelizumab) passed the Health Insurance Review and Assessment Service’s Cancer Disease Review Committee in August during its second attempt. Tevimbra is a PD-1 inhibiting immuno-oncology drug that has demonstrated clinical utility in second-line oesophageal squamous cell carcinoma and was approved in Korea in November last year. Currently, there are seven immuno-oncology drugs licensed and marketed in Korea, including ▲Keytruda, ▲Opdivo, ▲Tecentriq, ▲Imfinai, ▲Bavencio, ▲Jemperli, and ▲Tevimbra, which owns a total of 64 indications. However, only 21 indications (around 33%) are currently reimbursed. Also, none of these drugs are yet reimbursed for esophageal cancer. Currently, only platinum-based chemotherapy is reimbursed in Korea as both first-line and second-line treatment options for oesophageal squamous cell carcinoma. Reimbursement rates for immuno-oncology drugs by indication, including oesophageal cancer, are low due to high drug costs and finances. After being reimbursed for some cancers, such as lung cancer, overall claims for immuno-oncology drugs and their share of health insurance expenditures have increased significantly, leading to an increased burden on national health insurance finances. As of 2023, the total claims for anticancer drugs was around KRW 2.4 trillion, with immuno-oncology drugs accounting for about KRW 500 billion, or 20% of the total claims for anticancer drugs. This is why BeiGene plan to supply Tevimbra at a relatively low price is raising expectations. BeiGene’s corporate philosophy of providing ‘innovative new medicines at reasonable prices’ to eliminate underserved patients, has already been demonstrated through the reimbursement process it had shown with its blood cancer drug ‘Brukinsa (zanubrutinib).’ The company has also made Tevimbra available at no cost to select patients with oesophageal cancer through its Expanded Access Program (EAP). It remains to be seen if Tevimbra will make it onto the reimbursement list after passing discussions with the Pharmacoeconomic Evaluation Subcommittee, Risk Sharing Subcommittee, and Drug Reimbursement Evaluation Committee. In the global Phase III RATIONALE-302 study, Tevimbra prolonged median overall survival (OS) by 2.3 months (8.6 months vs. 6.3 months) compared to chemotherapy, resulting in a statistically significant 30% reduction in the risk of death. Compared to chemotherapy, Tevimbra resulted in more than twice as many patients responding to treatment (20% vs. 10%), and showed an improvement in the median duration of response of approximately 3 months, from 4.0 months to 7.1 months, with sustained responses and a reduction in tumor size, which is directly related to quality of life for esophageal cancer patients. As a result, the U.S. National Comprehensive Cancer Network (NCCN) revised its guidelines to recommend Tevimbra as a Category 1 preferred option for second-line treatment of esophageal squamous cell carcinoma.